Why is the roof of my mouth sore — and what is actually causing that pain? The roof of your mouth, known as the palate, is one of the most sensitive areas in your entire oral cavity.
When it hurts, even simple things like eating, drinking, or speaking become uncomfortable. Soreness in this area can come from something as minor as a hot pizza burn or as serious as a fungal infection.
The roof of your mouth is made up of two distinct sections that serve different functions.
The hard palate is the bony front portion covered by a thick layer of mucous membrane. It is firm to the touch and forms the ceiling of the front part of your mouth. The soft palate is the flexible tissue at the back of your mouth. It moves during swallowing and speaking, and it prevents food from entering the nasal cavity.
Both sections can become sore, swollen, or irritated — and the location of the pain often gives clues about the cause.
Yes — palate soreness is one of the most frequently reported oral complaints.
Most cases are caused by minor issues like burns, cuts, or canker sores. These heal on their own within a few days to two weeks. Less commonly, the soreness points to an infection, allergic reaction, or underlying health condition that needs professional care.
The key is knowing the difference between everyday soreness and something that needs a dentist or doctor.
The most common cause of a sore palate is burning the roof of your mouth with hot food or liquid.
Hot coffee, tea, soup, melted cheese, or fresh pizza can scald the thin, sensitive tissue of the palate instantly. The area turns red, feels raw, and may blister. This is sometimes called “pizza palate” because it happens so often with fresh hot pizza slices.
Most thermal burns on the palate heal completely within three to seven days without any treatment beyond avoiding further irritation.
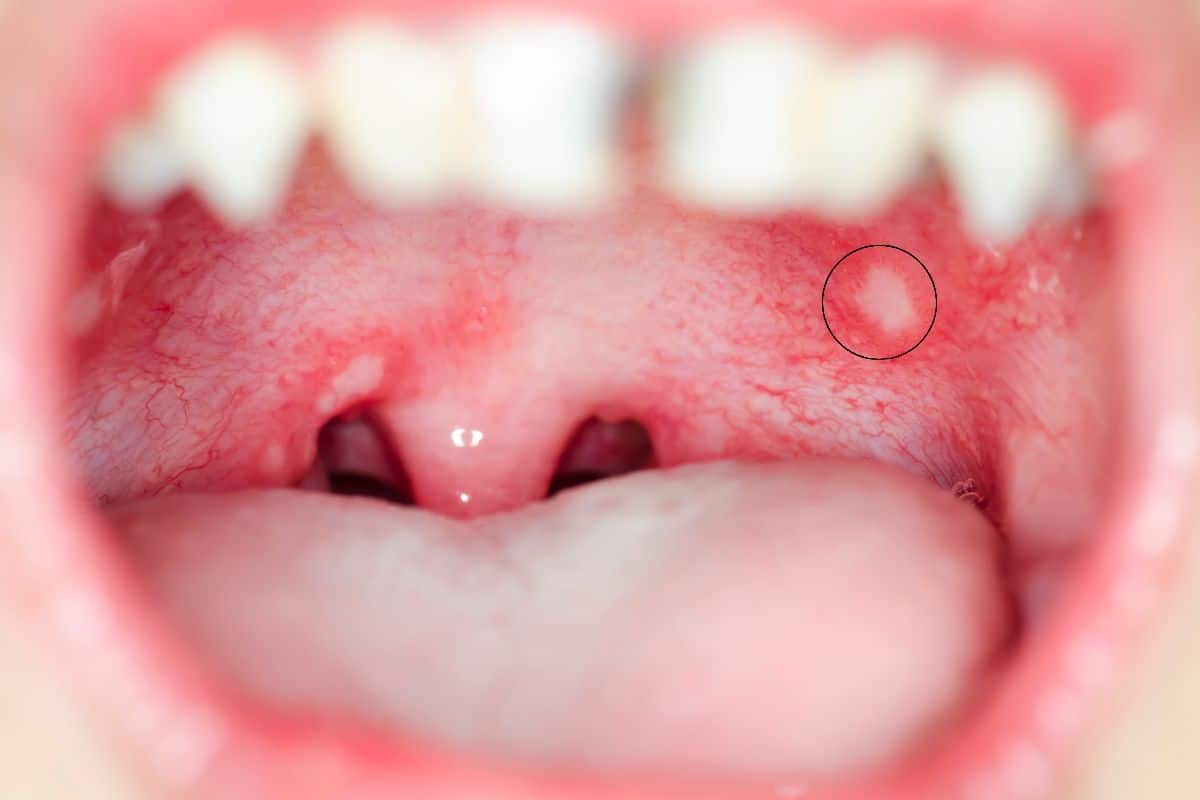
Canker sores are small, painful lesions that can appear on the hard or soft palate.
They appear as round or oval sores with a white or yellow center and a red border. Unlike cold sores, canker sores are not contagious and are not caused by a virus. They are typically triggered by stress, minor mouth injuries, hormonal changes, food sensitivities, or nutritional deficiencies — particularly low levels of iron, folate, or vitamin B12.
Most canker sores heal on their own within seven to fourteen days. Larger or persistent ones may need professional evaluation.
A sharp chip, cracker edge, hard bread crust, or bone fragment can scratch or cut the roof of your mouth while eating.
Dental appliances — including braces, retainers, dentures, and night guards — can also rub against the palate and cause irritation or sores over time. Even brushing too aggressively can irritate the delicate palate tissue.
Minor cuts and abrasions usually heal within a few days with proper oral hygiene and a soft diet.
Cold sores are caused by the herpes simplex virus type 1 (HSV-1) and most commonly appear on or around the lips.
In some cases, they form on the roof of the mouth — especially on the soft palate. They begin as small fluid-filled blisters that break open and form a scab. Cold sores are contagious and tend to recur, especially during periods of stress, illness, or sun exposure.
Antiviral medications such as acyclovir can reduce the severity and duration of outbreaks if taken early.
Oral thrush is a fungal infection caused by an overgrowth of Candida yeast in the mouth.
It produces creamy white or yellowish patches on the tongue, inner cheeks, and roof of the mouth. The patches may look like cottage cheese and can be painful, especially when eating or swallowing. Thrush is more common in infants, older adults, people taking antibiotics, and those with weakened immune systems or diabetes.
Treatment requires prescription antifungal medication such as nystatin or fluconazole.
Food allergies and environmental allergens can cause the soft tissues of the mouth — including the palate — to swell, tingle, or become sore.
Oral allergy syndrome is a condition where certain raw fruits, vegetables, or nuts trigger an immediate allergic reaction in the mouth. The roof of the mouth may feel itchy, tingly, or sore shortly after eating the trigger food. Seasonal allergens like pollen, dust, and pet dander can also inflame oral tissues, especially the soft palate.
If you notice a pattern of soreness after eating specific foods, speak to an allergist.
The sinuses sit directly above the hard palate, separated only by a thin layer of bone.
When the sinuses become infected or inflamed, that pressure and inflammation can radiate downward and cause pain or soreness on the roof of your mouth. Postnasal drip — excess mucus running down the back of the throat — can also irritate the soft palate, especially during colds, flu, or allergy season.
Sinus-related palate pain typically resolves once the underlying sinus condition is treated.
Saliva plays a critical role in protecting the oral tissues from drying out, irritation, and infection.
When saliva production drops — due to certain medications, dehydration, mouth breathing, or conditions like diabetes or Sjögren’s syndrome — the palate becomes dry, cracked, and prone to soreness. Dry mouth is also a significant risk factor for oral thrush, canker sores, and gum disease, all of which contribute to palate pain.
Staying well hydrated and using a saliva-substitute spray can provide relief.
An infected tooth or abscess, particularly involving the upper back teeth, can spread inflammation directly into the palate.
The roots of the upper molars and premolars sit very close to the palate. When a bacterial infection develops at the root tip, the surrounding tissue swells and becomes painful — and that pain is often felt on the roof of the mouth. Signs include throbbing pain, swelling, bad breath, and sensitivity to temperature.
A dental abscess is a dental emergency. It requires prompt treatment with antibiotics and often a root canal or extraction.
Burning mouth syndrome (BMS) is a chronic pain condition that causes a persistent burning or scalding sensation in the mouth — including the palate — without any visible sores or injuries.
It is more common in women, particularly around and after menopause. Contributing factors include nerve damage, hormonal changes, nutritional deficiencies (B vitamins, iron, zinc), anxiety, and dry mouth. The burning sensation often worsens throughout the day and may be accompanied by altered taste or a metallic taste in the mouth.
Treatment typically involves addressing the underlying cause, along with nerve pain medications or cognitive behavioral therapy.
Chronic smoking is a significant irritant to the oral mucosa.
Tobacco smoke contains hundreds of chemical compounds that dry out, inflame, and damage the delicate lining of the mouth and palate. Heavy smokers can develop nicotinic stomatitis — a condition where the hard palate develops a whitish, thickened appearance with small red bumps. This is considered a precancerous change and needs immediate dental evaluation.
Pipe and cigar smokers are at particularly high risk because they tend to hold smoke in the mouth longer.
Low levels of certain vitamins and minerals can cause the oral tissues to become thin, inflamed, and prone to sores.
Deficiencies most commonly linked to palate and mouth soreness include:
A blood test from your doctor can identify deficiencies, which are easily corrected with dietary changes or supplements.
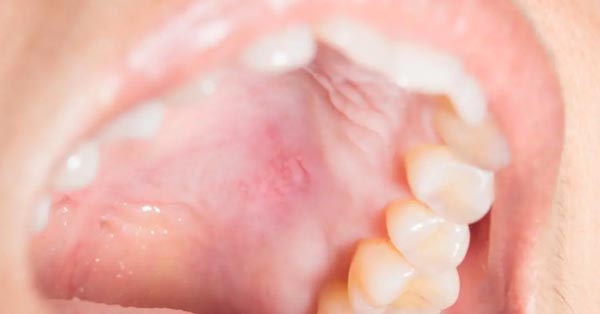
In rare cases, a persistent sore on the roof of the mouth can be a sign of oral cancer.
Oral cancers of the palate are more common in people who smoke, drink alcohol heavily, or have had prolonged HPV exposure. Warning signs include a sore or lump that does not heal after two weeks, unexplained bleeding, a white or red patch on the palate, numbness, or difficulty swallowing.
Oral cancer is highly treatable when caught early. Any unhealing sore lasting more than two weeks must be evaluated by a dentist or oral surgeon.
A mucocele is a small, round, fluid-filled cyst that forms when a salivary gland duct becomes blocked or damaged.
They usually appear on the inner lip but can also form on the roof of the mouth. They are typically painless and bluish or translucent in color. A mucocele on the soft palate may be called a ranula. While harmless, they can be bothersome if they are large or frequently bitten. A dentist can remove them with minor surgery if needed.
| Cause | Key Symptom | Typical Healing Time | Treatment |
|---|---|---|---|
| Thermal burn | Raw, red, blistered palate | 3–7 days | Cool foods, avoid irritants |
| Canker sore | White/yellow sore, red border | 7–14 days | Saltwater rinse, OTC gel |
| Physical cut/trauma | Sharp pain, visible scratch | 3–5 days | Soft diet, gentle rinsing |
| Cold sore (HSV-1) | Fluid-filled blisters | 7–10 days | Antiviral medication |
| Oral thrush | White patches, burning | Varies | Prescription antifungal |
| Allergic reaction | Tingling, swelling, itching | Hours to days | Antihistamine, avoid trigger |
| Sinus infection | Dull pressure, postnasal drip | Days to weeks | Decongestants, antibiotics |
| Dry mouth | Dry, cracked, sore palate | Ongoing | Hydration, saliva substitute |
| Dental abscess | Throbbing, swelling, bad breath | Needs treatment | Dentist — antibiotics/procedure |
| Burning mouth syndrome | Chronic burning, no visible sore | Chronic | Treat underlying cause |
| Smoking/tobacco | Thickened white patches | Varies | Quit smoking, dental check |
| Nutritional deficiency | Recurring sores, fatigue | Weeks | Supplements, diet changes |
| Oral cancer | Non-healing sore, lump | Does not heal alone | Urgent dental/medical evaluation |
| Mucocele | Painless fluid-filled cyst | Months or persistent | Surgical removal if needed |
The symptoms that accompany the soreness are just as important as the soreness itself.
Pain when swallowing often points to a soft palate issue, sinus infection, or throat involvement. Visible white patches suggest oral thrush or, in smokers, nicotinic stomatitis. Fluid-filled blisters indicate cold sores or a thermal burn blister. Throbbing pain and swelling in the upper jaw point to a dental abscess.
Unexplained bleeding or a lump on the palate with no clear cause is always a red flag that needs urgent professional evaluation.
A warm saltwater rinse is one of the most effective home treatments for palate soreness.
Dissolve half a teaspoon of table salt in one cup of warm water. Rinse gently for 30 seconds, two to three times a day. Salt reduces inflammation, draws out fluid from swollen tissue, and creates an environment that discourages bacterial growth. This works well for canker sores, minor cuts, and post-burn soreness.
Eating cold, soft foods is one of the simplest ways to soothe a sore palate.
Yogurt, smoothies, applesauce, ice cream, and chilled soups provide relief without further irritating the damaged tissue. Ice chips or cold water held in the mouth for a few seconds can also temporarily numb the area. Avoid hot, spicy, acidic, crunchy, or salty foods until the palate heals.
OTC oral anesthetic gels containing benzocaine can provide fast, temporary pain relief when applied directly to the sore area.
Products like Orajel or Anbesol numb the tissue within minutes. They are especially useful before meals when eating is particularly painful. Use as directed and avoid applying them to large areas of the mouth repeatedly.
Keeping the mouth clean promotes faster healing and prevents secondary infections.
Brush gently twice a day using a soft-bristled toothbrush. Avoid toothpastes containing sodium lauryl sulfate (SLS) — this ingredient is a known trigger for canker sores in sensitive individuals. Use an alcohol-free mouthwash to avoid further drying out the tissue.
Drinking plenty of water throughout the day keeps the oral tissues moist and supports healing.
Dehydration reduces saliva flow, which means the palate loses one of its key natural defenses. Aim for at least eight glasses of water a day, more in hot weather or after exercise. Avoid alcohol and caffeine, which dehydrate oral tissues and slow healing.
Stopping behaviors that irritate the palate is critical to allowing it to heal.
Avoid smoking, drinking alcohol, and eating trigger foods during healing. If a dental appliance is causing the soreness, contact your dentist about adjusting or replacing it. If a specific food is consistently triggering a reaction, keep a food diary and discuss it with your doctor.
| Eat These | Avoid These |
|---|---|
| Yogurt, smoothies, milkshakes | Hot beverages (coffee, tea, soup) |
| Chilled applesauce, pudding | Spicy foods (hot sauce, chili) |
| Scrambled eggs, soft tofu | Acidic foods (citrus, tomatoes, vinegar) |
| Mashed potatoes, soft rice | Crunchy or sharp foods (chips, crackers) |
| Ice cream, cold soups | Alcohol and carbonated drinks |
| Oatmeal (cooled to lukewarm) | Salty snacks and processed foods |
| Water, herbal teas (lukewarm) | Very hard bread or raw vegetables |
Most palate soreness resolves on its own, but some situations need professional attention right away.
See a dentist or doctor if the sore or pain lasts more than two weeks with no sign of improvement. You should also seek care if you notice significant swelling, pus, or a lump forming on the palate. Trouble swallowing, breathing, or opening your mouth fully are urgent symptoms that need same-day evaluation.
Fever alongside mouth pain suggests an active infection that may need antibiotics. Recurring sores that keep coming back in the same location, or white and red patches that do not resolve, need to be biopsied to rule out oral cancer.
Any child who develops palate sores with fever or difficulty eating should be seen by a pediatrician promptly.
Your provider will examine the palate visually and feel for any lumps or irregularities.
They will ask about your medical history, medications, diet, and how long the soreness has been present. Depending on what they find, they may order blood tests to check for nutritional deficiencies or infections, take a swab culture if thrush or a bacterial infection is suspected, or refer you for a biopsy if a suspicious lesion is present.
For dental causes like an abscess, they will take X-rays to assess the extent of infection and recommend either antibiotics, a root canal, or an extraction depending on severity.
You cannot prevent every cause of palate soreness, but you can significantly reduce your risk.
Let hot food and drinks cool before eating or drinking. Test temperature with your lip, not your tongue. Eat slowly and chew carefully to avoid scraping the palate with hard or sharp-edged foods. Maintain consistent oral hygiene — brush twice a day, floss daily, and use an alcohol-free rinse.
Stay hydrated to keep oral tissues moist and well-protected by saliva. Quit smoking — it is one of the single most damaging habits for long-term oral health. Eat a balanced diet rich in B vitamins, iron, and vitamin C to keep oral tissues resilient. Schedule a dental checkup twice a year so any developing issues are caught before they become painful.

| Nutrient | Oral Symptom When Deficient | Food Sources |
|---|---|---|
| Vitamin B12 | Sore, inflamed mouth lining, tongue pain | Meat, eggs, dairy, fortified cereals |
| Iron | Mouth ulcers, angular cheilitis, pale gums | Red meat, lentils, spinach, tofu |
| Folate (B9) | Recurring canker sores | Leafy greens, beans, citrus, liver |
| Vitamin C | Sore, swollen, bleeding gums | Oranges, kiwi, bell peppers, broccoli |
| Zinc | Slow wound healing in the mouth | Pumpkin seeds, chickpeas, beef, cashews |
| Vitamin D | Linked to recurring aphthous ulcers | Fatty fish, egg yolks, fortified milk |
It may be a canker sore forming before it becomes visible, early-stage burning mouth syndrome, or a nutritional deficiency. If it lasts more than two weeks, see a dentist to rule out anything serious.
Yes. The sinuses sit directly above the hard palate, and sinus pressure or infection can cause referred pain that feels like it is coming from inside your mouth.
Minor burns and cuts heal in 3 to 7 days. Canker sores and cold sores typically resolve within 7 to 14 days. Sores lasting longer than two weeks need professional evaluation.
Yes. Stress weakens the immune system and is a well-known trigger for canker sores and cold sore outbreaks, both of which can appear on the palate.
Rarely, but it can be. A sore that does not heal after two weeks, bleeds, or comes with a lump or discolored patch needs to be evaluated by a dentist or oral surgeon immediately.
Pain when swallowing often involves the soft palate or throat. Causes include tonsillitis, a sinus infection, postnasal drip, or a dental abscess spreading to surrounding tissue.
Yes. Reduced saliva dries out the palate tissue, making it more prone to irritation, cracking, and infection — including oral thrush, which is a common dry mouth complication.
A warm saltwater rinse, cool soft foods, OTC numbing gel, staying hydrated, and avoiding spicy or acidic foods all speed healing. Good oral hygiene is also essential.
Yes. Toothpastes containing sodium lauryl sulfate (SLS) are a known trigger for canker sores in some people. Switching to an SLS-free toothpaste can reduce recurrence.
See a dentist if pain lasts more than two weeks, if there is visible swelling, a lump, pus, difficulty swallowing, or if the sore is accompanied by fever or significant bleeding.
The roof of your mouth is sore for a reason — and in most cases, that reason is straightforward and easy to treat at home. A thermal burn from hot food, a canker sore triggered by stress, or a minor cut from a sharp chip are all common and heal on their own within days.
But not every case is that simple. Oral thrush, dental abscesses, nutritional deficiencies, and sinus infections all need targeted treatment to resolve properly. And in rare cases, a non-healing sore is a sign of oral cancer that must not be ignored.
The two-week rule is your best guide. If palate soreness has not improved after two weeks, or if it comes with swelling, a lump, bleeding, difficulty swallowing, or fever, it is time to see a professional. Caught early, almost every condition that causes a sore roof of mouth is highly manageable. Do not wait until the pain becomes unbearable — your oral health is worth protecting.