
Why am I suddenly lactose intolerant when I had no issues with dairy for years? You are not alone.
Millions of adults wake up one day and realize that the glass of milk or bowl of ice cream they once enjoyed now leaves them bloated, gassy, and running to the bathroom.
Lactose intolerance can develop at any stage of life, even in your 30s, 40s, or beyond. Understanding what triggers it, how to spot the signs, and what you can do about it is the first step toward feeling better.

Lactose intolerance is the inability to fully digest lactose, the natural sugar found in milk and dairy products. It is not a food allergy. It is a digestive issue.
Your small intestine produces an enzyme called lactase. Lactase breaks lactose down into two simpler sugars, glucose and galactose, which are then absorbed into your bloodstream.
When lactase levels drop too low, lactose passes undigested into the colon. Bacteria in the colon ferment it, producing gas and acids that cause uncomfortable symptoms.
Lactose intolerance is far more widespread than most people realize. The global numbers are striking.
| Population Group | Estimated Prevalence of Lactose Intolerance |
|---|---|
| Global average | ~68% have reduced lactose digestion after infancy |
| East Asian adults | Up to 90% |
| Black adults (US) | ~85% |
| Hispanic adults (US) | ~50–80% |
| White adults (US) | ~15% |
| Northern Europeans | As low as 5% |
The condition is especially common in people of Asian, African, Hispanic, Native American, and Jewish descent. If you are suddenly experiencing symptoms, your ethnic background can be a contributing factor.
Sudden onset lactose intolerance in adults is more common than many doctors once believed. Several key factors can trigger it.
The most common reason is simple biology. As children grow older, the body naturally produces less lactase. This process, called lactase nonpersistence, usually begins between ages 3 and 5.
For many people, lactase levels remain just high enough to handle dairy throughout their teens and twenties. But as the years pass, levels continue to drop. By middle age, many people cross the threshold where dairy starts causing symptoms.
This is why you may have eaten cheese and yogurt your whole life with no problem, but now suddenly cannot tolerate them.
An illness, infection, or injury to the small intestine can damage the cells that produce lactase. This is called secondary lactose intolerance.
Common triggers include:
Celiac disease, Crohn’s disease, gut infections, bacterial overgrowth in the intestines, and surgery involving the small intestine. When the underlying condition is treated, lactase production may recover over time.
If your symptoms appeared shortly after a stomach bug or a period of illness, secondary intolerance is very likely the cause.
A bad bout of food poisoning or gastroenteritis can temporarily wipe out lactase-producing cells in the intestinal lining.
Even after the infection is gone, it can take weeks or months for lactase levels to recover. During that time, dairy causes the same symptoms as regular lactose intolerance.
This is sometimes called transient or temporary lactose intolerance. Many people recover full dairy tolerance once the gut heals.
Both Crohn’s disease and celiac disease cause chronic inflammation and damage to the lining of the small intestine. This damage directly reduces lactase production.
Many people are diagnosed with these conditions only after they notice new dairy intolerance. If you also experience unexplained weight loss, persistent diarrhea, or fatigue, it is worth ruling these out with a doctor.
Antibiotics can disrupt the gut microbiome. They kill off both harmful and helpful bacteria, altering the environment in your colon.
Since the gut bacteria play a role in how lactose is fermented, changes in your microbiome after a course of antibiotics can make lactose symptoms appear or worsen for a period of time.
Radiation therapy to the abdomen or surgery involving the digestive tract can damage the small intestine and reduce lactase output.
If you have recently undergone such treatment and are now struggling with dairy, this is very likely the reason. Talk to your gastroenterologist for a personalized plan.
Some women notice changes in dairy tolerance during or after pregnancy. Hormonal shifts can affect gut motility and how food is processed, making symptoms more noticeable.
Ironically, a sudden increase in how much dairy you eat can also trigger symptoms. If you have borderline lactase levels and start consuming much more milk, cheese, or cream, you can push your gut past its tolerance threshold.
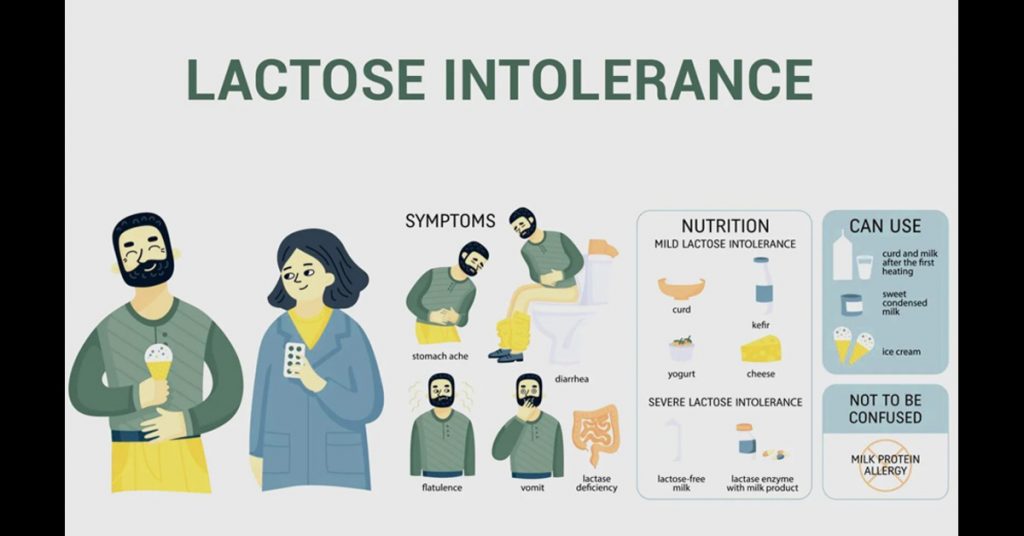
Knowing the signs helps you identify whether dairy is the culprit. Symptoms usually appear within 30 minutes to 2 hours after consuming lactose. In some people, symptoms may take up to 24 to 48 hours.
| Symptom | Description |
|---|---|
| Bloating | A swollen, tight feeling in the abdomen |
| Gas and flatulence | Excess gas produced by bacterial fermentation of lactose |
| Diarrhea | Loose, watery stools after eating dairy |
| Stomach cramping | Pain or spasms in the lower abdomen |
| Nausea | A queasy feeling, sometimes leading to vomiting |
| Stomach gurgling | Loud rumbling sounds from the intestines |
| Urgency | A sudden, pressing need to use the bathroom |
The severity of your symptoms depends on how much lactase your body still makes and how much lactose you consumed.

Understanding the type of lactose intolerance you have matters for treatment.
Primary lactose intolerance is the most common type. It is caused by the natural, genetic decline of lactase production over time. It is permanent but manageable.
Secondary lactose intolerance develops because of damage to the small intestine from disease, infection, or injury. It can be temporary if the underlying cause is treated successfully.
Congenital lactose intolerance is extremely rare. Babies are born without the ability to produce any lactase at all. It is caused by a mutation in the LCT gene.
Developmental lactose intolerance occurs in premature babies whose small intestines have not yet developed enough to produce adequate lactase. It usually resolves as the baby matures.
Not all dairy is equal. Some foods have very high lactose content, while others are naturally low. Knowing the difference helps you manage your intake without cutting out all dairy completely.
| Food | Lactose Content | Tolerance Level |
|---|---|---|
| Fresh whole milk (1 cup) | ~12g | High – often problematic |
| Ice cream (1/2 cup) | ~6g | Moderate |
| Soft cheese (ricotta, cottage) | ~3–6g | Moderate |
| Yogurt (1 cup) | ~4–5g | Often tolerated due to live cultures |
| Hard aged cheese (cheddar, parmesan) | ~0–2g | Usually well tolerated |
| Butter | ~0.1g | Rarely causes symptoms |
| Lactose-free milk | ~0g | Safe for most people |
| Cream-based soups, sauces | Varies | Check labels |
Many people who believe they must avoid all dairy can actually enjoy hard cheeses, butter, and yogurt without symptoms. The fermentation process in aged cheeses and yogurt breaks down most of the lactose naturally.
If you suspect lactose intolerance, a healthcare provider can confirm it through specific tests. Self-diagnosis is not always reliable.
This is the most commonly used and most accurate test. You drink a solution containing a set amount of lactose (usually 25 to 50 grams). A provider then measures the hydrogen in your breath at regular intervals.
If your body is not digesting lactose, bacteria in your colon ferment it and produce hydrogen gas. A rise of 20 parts per million or more above your baseline confirms lactose malabsorption.
You drink a lactose solution, and blood samples are taken over two hours to measure your glucose levels. If your blood sugar does not rise, your body is not absorbing lactose properly.
This test is mainly used for infants and young children. Undigested lactose in the colon produces lactic acid and other acids detectable in a stool sample.
A blood or saliva sample can reveal variants in your LCT and MCM6 genes that influence lactase persistence. This test can confirm whether your intolerance is genetic.
A simpler approach is removing all dairy from your diet for two to four weeks and observing whether symptoms resolve. Then reintroduce dairy gradually and note what happens.
The good news is that lactose intolerance is very manageable. Most people do not need to eliminate all dairy completely.
Over-the-counter lactase supplements like Lactaid give your body the enzyme it is missing. Take them right before you eat or drink dairy to prevent symptoms from occurring.
They are widely available, affordable, and effective for most people.
Lactose-free milk, cheese, yogurt, and ice cream taste the same as regular dairy. The lactose has been pre-digested by adding lactase, so your gut does not need to do the work.
Your body may tolerate small amounts of lactose better than large portions. Instead of a full glass of milk, try a splash in your coffee. Spread your dairy intake throughout the day rather than consuming it all at once.
Consuming dairy as part of a meal slows digestion. This gives whatever lactase you still produce more time to work, reducing the chance of symptoms.
Hard aged cheeses like parmesan, aged cheddar, and Swiss contain very little lactose. Yogurt with live active cultures is also easier to digest because the bacteria in yogurt help break down lactose.
Plant-based milks made from oats, almonds, soy, or rice contain no lactose at all. Many are now fortified with calcium and vitamin D to match the nutritional profile of cow’s milk.
If you reduce dairy, make sure you are getting enough calcium and vitamin D from other sources. Deficiency in these nutrients over time can lead to bone loss.
| Non-Dairy Calcium Source | Calcium Per Serving |
|---|---|
| Fortified oat milk (1 cup) | ~350mg |
| Canned sardines with bones (3 oz) | ~325mg |
| Cooked kale (1 cup) | ~177mg |
| Fortified soy milk (1 cup) | ~300mg |
| Almonds (1 oz) | ~76mg |
| Broccoli (1 cup cooked) | ~62mg |
| White beans (1/2 cup) | ~131mg |
Probiotic supplements or probiotic-rich foods like kefir and kimchi can improve your gut microbiome. A healthier gut environment may improve how your body handles lactose over time.
You should speak with a healthcare provider if:
Your symptoms are severe or getting worse quickly. You notice blood in your stool. You are losing weight without trying. You have persistent diarrhea or cramping beyond a few days. Symptoms do not improve after cutting out dairy. You have a personal or family history of celiac disease or Crohn’s disease.
A gastroenterologist can confirm your diagnosis and check whether a more serious condition like celiac or Crohn’s disease is behind your new dairy intolerance.

These two conditions are often confused but are fundamentally different.
| Feature | Lactose Intolerance | Milk Allergy |
|---|---|---|
| Cause | Digestive enzyme deficiency | Immune system response to milk protein |
| Symptoms | Digestive (bloating, gas, diarrhea) | Can include hives, wheezing, anaphylaxis |
| Dangerous? | No, not life-threatening | Yes, can be life-threatening in severe cases |
| Age of onset | Any age, common in adults | Usually appears in first year of life |
| Treatment | Diet management, lactase supplements | Strict dairy avoidance, epinephrine if needed |
If you experience hives, swelling, difficulty breathing, or anaphylaxis after eating dairy, that is a milk allergy and requires immediate medical attention. An allergist can perform allergy testing to differentiate the two.
Irritable bowel syndrome (IBS) and lactose intolerance share many of the same symptoms. Bloating, cramping, and diarrhea are common in both.
Some people with IBS find that dairy worsens their symptoms significantly, even if they do not test positive for lactose intolerance on clinical tests. A low-FODMAP diet, which restricts fermentable sugars including lactose, is often recommended for IBS patients and may help both conditions.
Whether lactose intolerance is reversible depends on the type.
Primary lactose intolerance caused by genetic lactase decline is permanent. Lactase enzyme levels will not recover on their own.
Secondary lactose intolerance caused by illness or gut damage can improve or fully resolve if the underlying condition is treated and the intestinal lining heals. This process may take months.
Temporary intolerance following a gut infection often resolves within a few weeks as the gut heals.
Lactase production naturally declines with age. Once levels drop below what your body needs to digest dairy comfortably, symptoms appear even if you had no issues before.
It can feel sudden, but the decline in lactase is gradual. What seems overnight is usually a threshold being crossed after years of slowly dropping enzyme levels.
It can be. Secondary intolerance can be triggered by celiac disease, Crohn’s disease, or gut infections. See a doctor if symptoms are severe or accompanied by weight loss or blood in stool.
Yes. A gut infection can temporarily damage lactase-producing cells, causing secondary lactose intolerance that may last weeks to months while your gut heals.
It varies. Most people recover within a few weeks to a few months after the intestinal lining heals, especially with proper diet and probiotics.
Yes. Hard aged cheeses and yogurt with live cultures contain very little lactose and are well-tolerated by most lactose-intolerant people.
Yes, they are effective for most people. Take them just before eating dairy to provide the enzyme your body is not producing enough of.
No. Lactose intolerance is a digestive issue caused by low lactase enzyme levels. A milk allergy is an immune system reaction that can be life-threatening.
Stress can worsen gut sensitivity and slow or speed up digestion, which may make lactose intolerance symptoms more noticeable even with the same amount of dairy.
Yes, though it is more common in adults. It can develop during childhood, particularly in teens, as lactase production continues to decline after early childhood.
Why am I suddenly lactose intolerant? The answer often comes down to your body’s natural decline in lactase enzyme production over time, combined with factors like illness, gut damage, genetics, or changes in your microbiome.
The good news is that sudden lactose intolerance is very common, well understood, and highly manageable. You do not have to give up all dairy. With the right combination of lactase supplements, smarter dairy choices, and dietary adjustments, most people can continue to enjoy dairy in some form without misery.
If your symptoms are severe, persistent, or paired with other warning signs, a visit to your doctor or gastroenterologist can rule out more serious underlying conditions and put you on the right path to relief in 2026 and beyond.