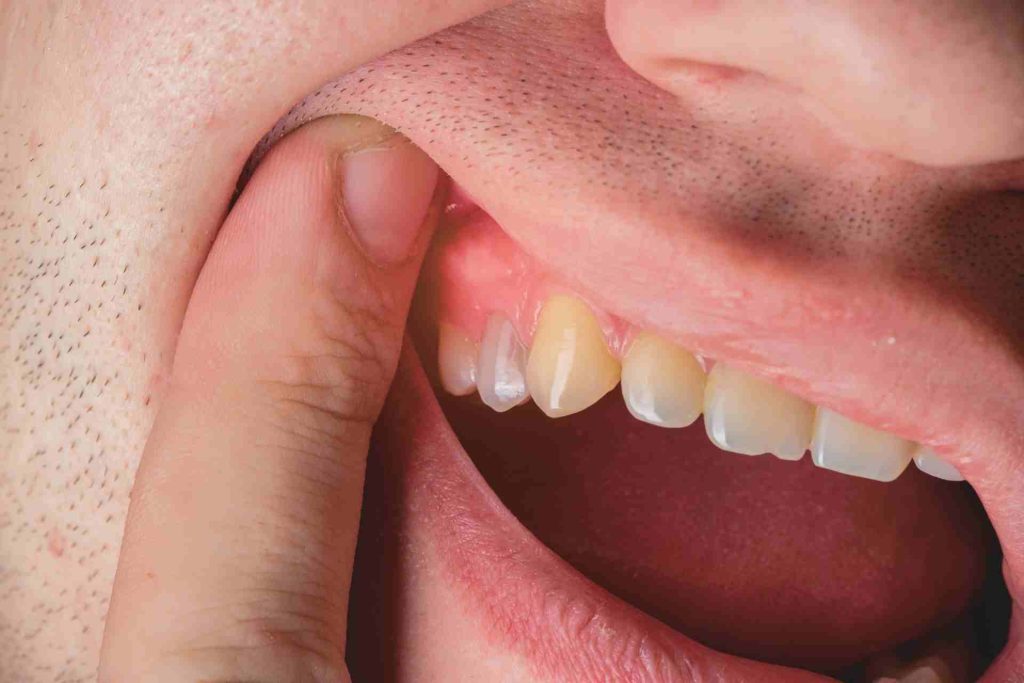
Why is my gum swollen around one tooth in the back? This is one of the most common dental complaints people search for — and for good reason. Localized gum swelling around a single back tooth can be alarming, painful, and confusing.
It could be something as simple as trapped food debris or as serious as a dental abscess. Either way, ignoring it is never the right move.
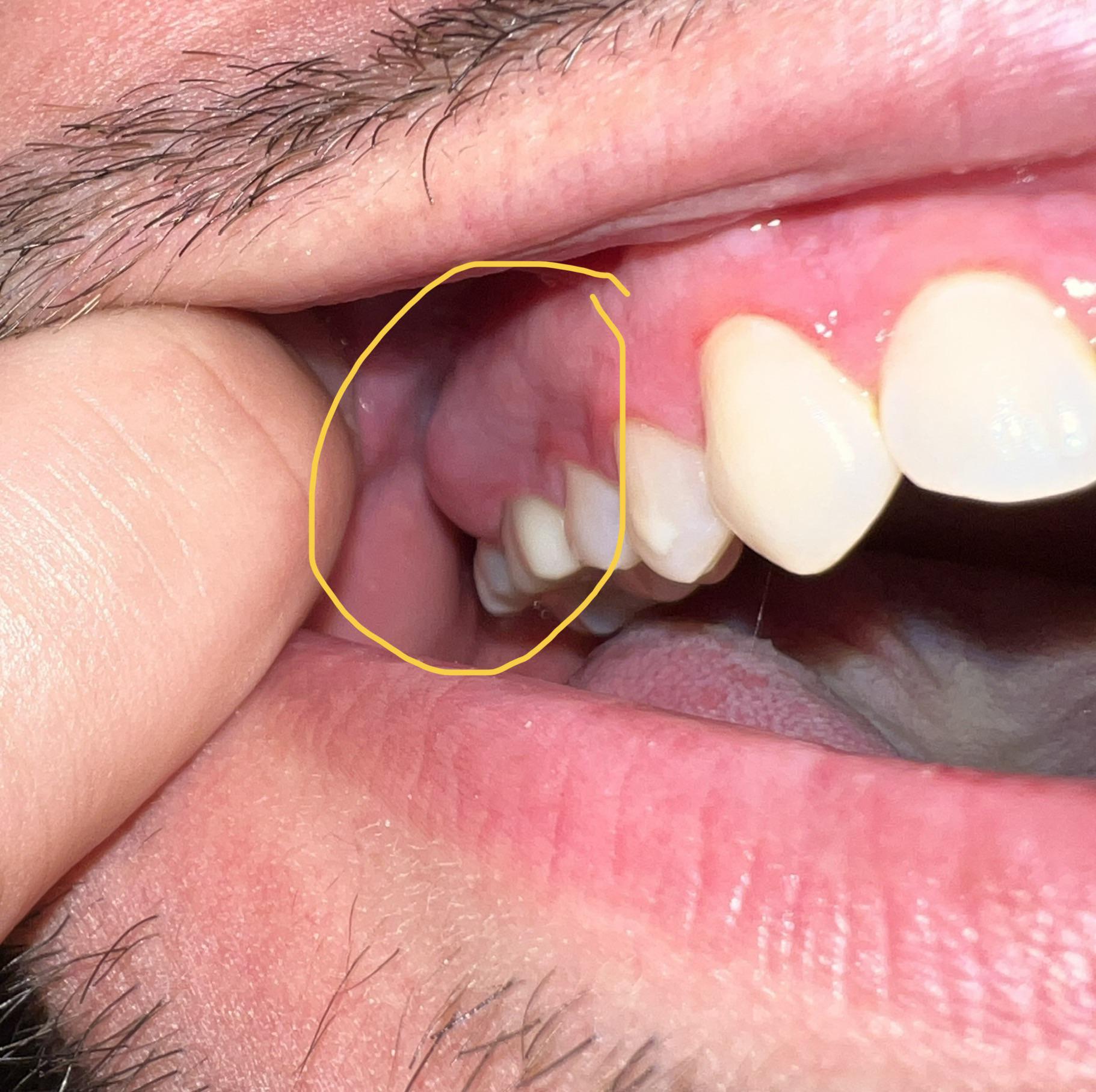
When only one area of your mouth is swollen, it usually means something is happening in that specific spot.
Your body is sending a signal. Gum tissue swells because your immune system is fighting irritation, infection, or injury near that tooth.
Back teeth — especially molars and wisdom teeth — are harder to clean. That makes them more vulnerable to the problems listed below.
This is the simplest and most overlooked cause.
When food particles get stuck between the gum and tooth — especially popcorn husks, meat fibers, or seeds — they irritate the soft tissue. The gum responds by swelling.
Brushing and flossing right after meals can remove the debris early. If the swelling does not go away within two days, see a dentist.
Gum disease does not always affect your whole mouth at once. It can target one tooth — especially one that is harder to clean.
According to the CDC, nearly half of adults over 30 in the US have some form of gum disease. In its earliest stage, called gingivitis, gums become red, swollen, and may bleed slightly when you brush.
If gingivitis goes untreated, it advances to periodontitis. At that stage, gums pull away from the tooth, bone starts to break down, and the tooth can eventually loosen and fall out.
Signs of gum disease around one tooth:
| Symptom | Stage |
|---|---|
| Red, puffy gums | Gingivitis |
| Bleeding when brushing | Gingivitis |
| Gum pulling away from tooth | Early periodontitis |
| Persistent bad breath | Gingivitis / Periodontitis |
| Loose-feeling tooth | Advanced periodontitis |
| Bone loss visible on X-ray | Periodontitis |
A dental abscess is a pocket of pus caused by bacterial infection. It is one of the most painful causes of localized gum swelling.
There are two main types. A periapical abscess forms at the tip of the tooth root — usually due to untreated tooth decay or a cracked tooth. A periodontal abscess forms in the gum tissue itself.
Both types cause significant swelling, throbbing pain, redness, and sometimes a bad taste or fever. If you suspect an abscess, see your dentist immediately — the infection can spread.
Pericoronitis is one of the most common reasons why gum is swollen around one tooth in the back — specifically around wisdom teeth.
When a wisdom tooth only partially erupts, a flap of gum tissue called an operculum forms over it. Food, bacteria, and debris get trapped under this flap and cause infection and swelling.
It is most common in people aged 20 to 29 and can be either acute (short-term) or chronic (long-term).
Symptoms of pericoronitis:
Left untreated, pericoronitis can develop into a serious abscess and in rare cases become life-threatening by spreading to the throat and neck.
Plaque is a sticky, colorless film of bacteria that forms on your teeth throughout the day.
When plaque is not removed by brushing and flossing, it hardens into tartar. Tartar cannot be removed at home — it requires a professional cleaning. Tartar buildup around one tooth irritates the gum and causes localized swelling.
A crack in a tooth allows bacteria to enter deep into the tooth structure. Once bacteria reach the pulp — the soft inner layer containing nerves and blood vessels — infection sets in fast.
The result is swelling, pain, and sometimes visible redness around just that one tooth. A cracked tooth often needs a root canal or extraction, depending on the severity.
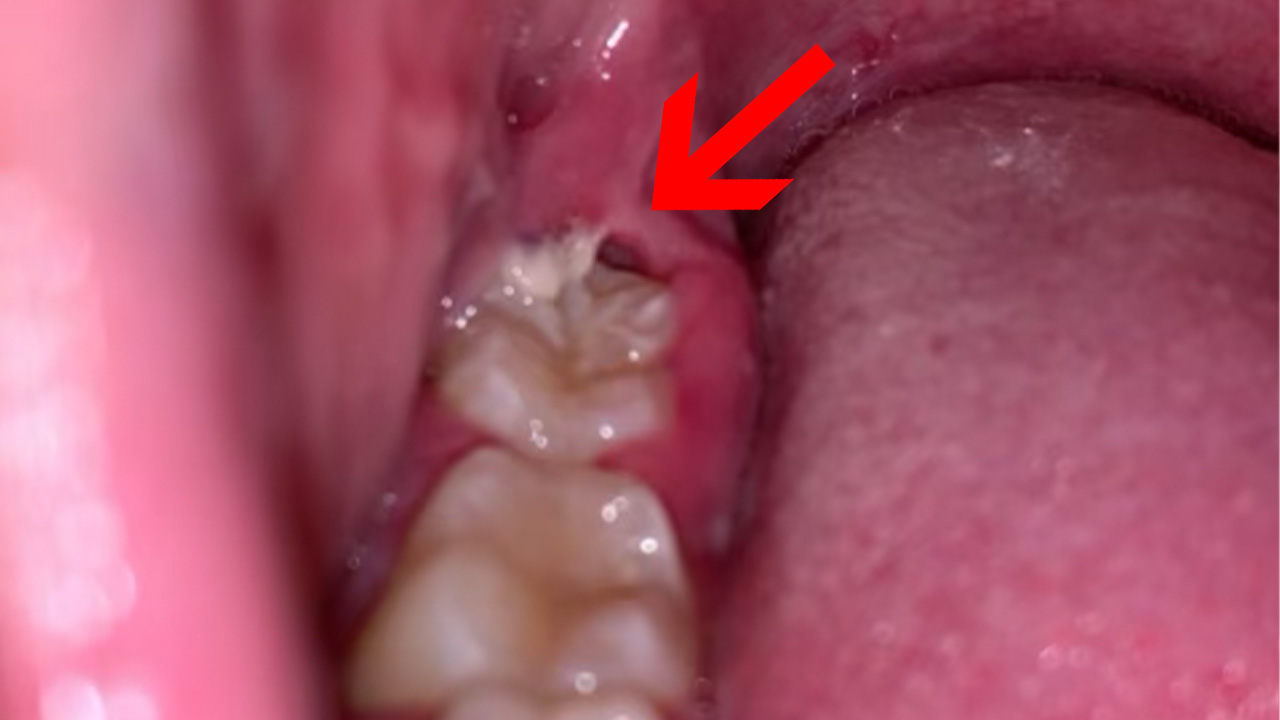
Rushing your brushing or skipping flossing regularly lets plaque and bacteria build up around specific teeth — especially the back ones that are hardest to reach.
Over time, this localized neglect causes the gum to become inflamed. Improving your routine and getting a professional cleaning is usually enough to reverse early-stage swelling.
Recent dental work — like a filling, crown, or extraction — can sometimes cause temporary gum swelling around the treated tooth.
A dental appliance like braces or ill-fitting dentures can also irritate the gum tissue in one specific area. Plaque that accumulates around braces brackets is a common culprit.
Decay under the gum line irritates surrounding gum tissue directly.
When a cavity goes untreated, it spreads deeper into the tooth. This triggers inflammation in the gum tissue directly surrounding that tooth, causing noticeable localized swelling.
A fracture that extends to the root of the tooth is serious.
Root fractures are difficult to see without an X-ray, but they allow bacteria to enter and cause infection deep in the gum tissue. The swelling caused by a root fracture is often persistent and does not respond to home care.
Waking up with a swollen gum around one tooth can feel terrifying — especially when there was no pain the night before.
Here is what usually happens. A small infection or irritation has been building up silently for days or weeks. When the body can no longer hold it back, it responds with rapid swelling — often overnight. A dental abscess is the most common reason for this sudden overnight swelling.
The process typically looks like this:
If gum swelling appears suddenly overnight, do not wait. Contact a dentist as soon as possible.
Use this table to narrow down what might be causing your swollen gum.
| Possible Cause | Key Symptoms | Onset |
|---|---|---|
| Trapped food | Mild soreness, no fever | Gradual |
| Gingivitis | Bleeding gums, redness | Gradual |
| Periodontitis | Gum recession, loose tooth | Slow and progressive |
| Dental abscess | Throbbing pain, pus, fever | Sudden |
| Pericoronitis | Back of mouth, difficulty swallowing, bad taste | Sudden or gradual |
| Cracked tooth | Sharp pain when biting, sensitivity | Sudden |
| Plaque buildup | General soreness, bad breath | Gradual |
| Tooth decay | Sensitivity, visible cavity | Gradual |
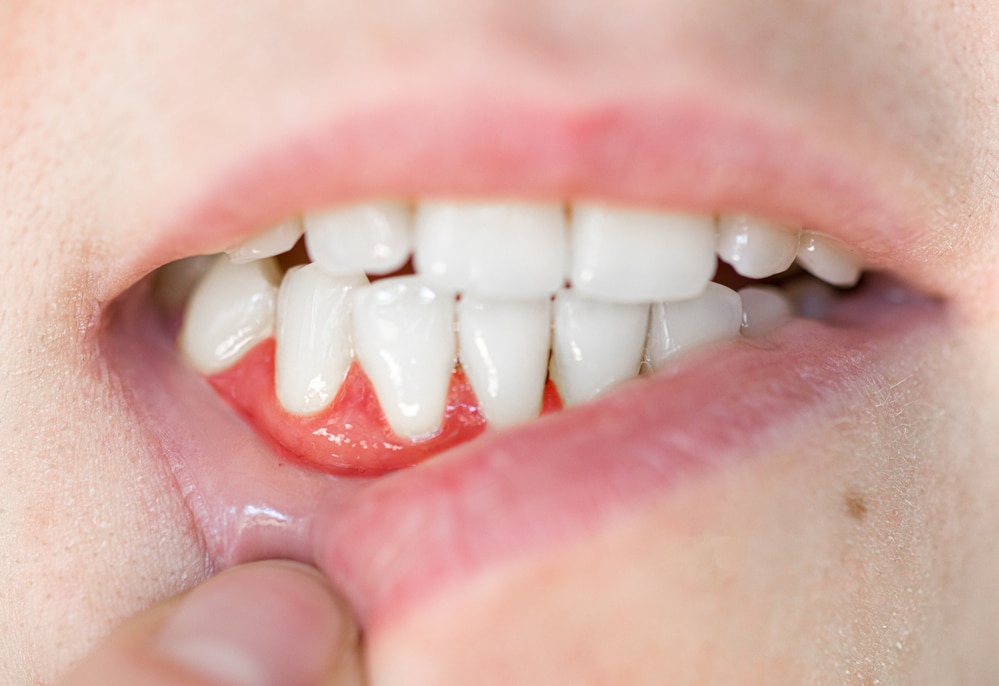
These methods can reduce mild inflammation and provide temporary relief. They do not replace a dental visit for serious conditions.
| Treatment | When It Is Used |
|---|---|
| Professional Cleaning / Scaling | Plaque and tartar buildup |
| Deep Cleaning (Root Planing) | Gum disease / periodontitis |
| Antibiotics | Abscess, pericoronitis, spreading infection |
| Root Canal Therapy | Infected tooth pulp, periapical abscess |
| Tooth Extraction | Severely damaged or infected tooth |
| Incision and Drainage | Draining a dental abscess |
| Operculum Removal (Operculectomy) | Recurrent pericoronitis |
| Wisdom Tooth Extraction | Impacted or problematic wisdom teeth |
| Osseous Surgery | Reducing deep pockets around teeth |
| LANAP (Laser Therapy) | Advanced periodontitis |
Pericoronitis deserves its own section because it is so frequently the answer to “why is my gum swollen around one tooth in the back?”
It is essentially a wisdom tooth infection. Up to 81% of individuals with partially erupted third molars may experience some form of pericoronitis during their lifetime.
The partially erupted tooth creates a gum flap. That flap traps food and bacteria. Infection follows. Swelling, pain, and sometimes fever result.
Acute pericoronitis hits fast — intense pain, difficulty opening the mouth, fever, and swollen lymph nodes.
Chronic pericoronitis is milder and longer-lasting — a dull ache, bad taste, and persistent mild swelling that comes and goes.
Mild cases:
Moderate to severe cases:
Recovery with treatment typically takes one to two weeks.
Some situations cannot wait. Go to a dentist or emergency dental clinic right away if you experience:
These can be signs of a spreading infection that requires urgent treatment. In severe cases, an untreated abscess or pericoronitis can become life-threatening.
See your dentist within a few days if:
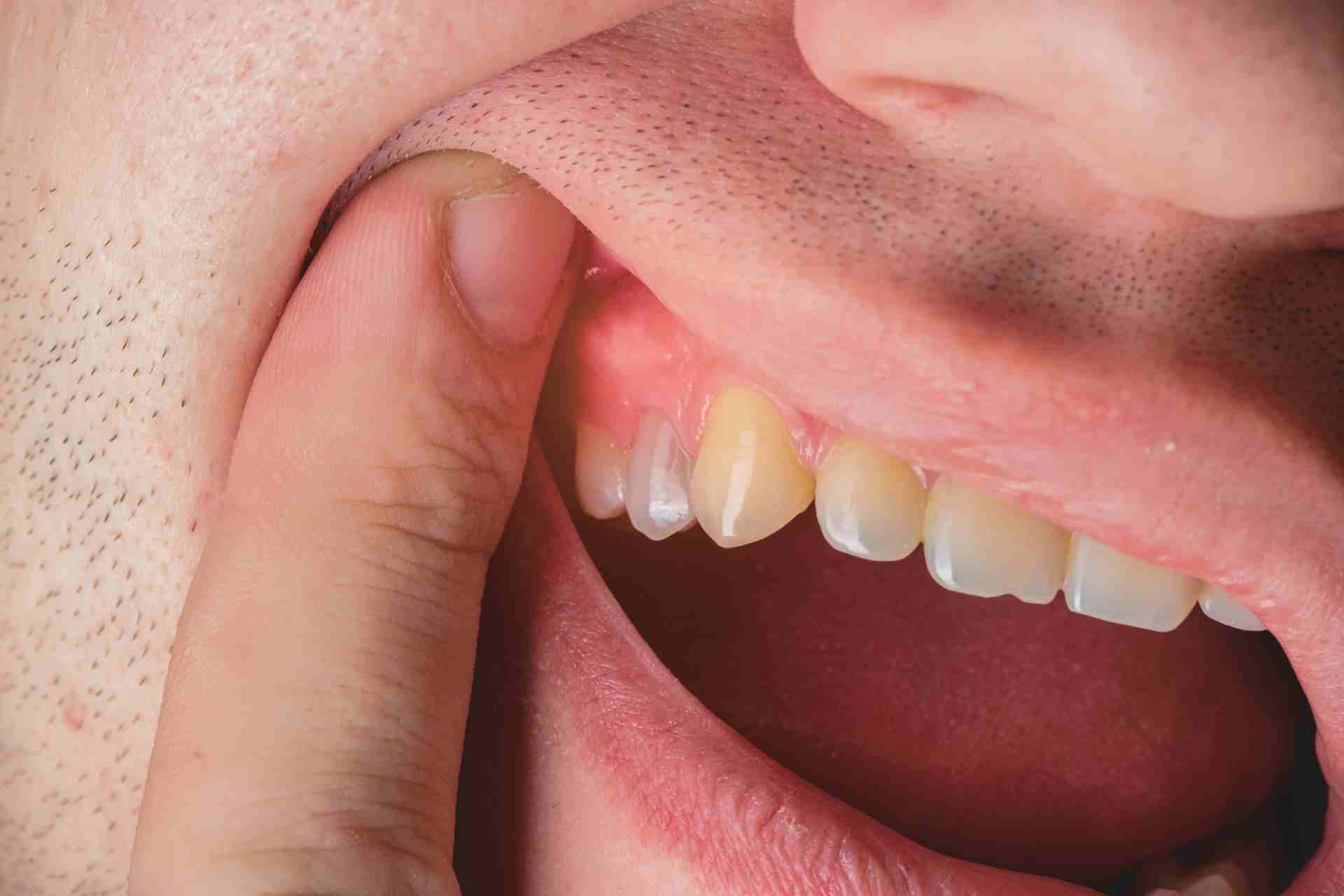
Prevention is far easier than treatment. Good habits protect your gum tissue and reduce your risk significantly.
This article is written at a Grade 7–8 reading level. Short paragraphs and plain language are used throughout so the information is accessible whether you are reading on your phone at 2 AM with a throbbing tooth or doing research for a dentist visit.
Localized swelling usually points to a specific local problem — trapped food, an infection, plaque buildup, a dental abscess, or pericoronitis (wisdom tooth infection). A dentist can pinpoint the exact cause with an examination and X-ray.
Minor swelling caused by trapped food may resolve within 1–2 days with better brushing and flossing. Swelling caused by infection, abscess, or gum disease will not resolve on its own and needs professional treatment.
It becomes an emergency if you have fever, face swelling, difficulty swallowing, trouble opening your mouth, or rapidly worsening pain. These signs mean the infection may be spreading and you need urgent dental care.
A gum abscess causes throbbing or pulsating pain, visible swelling, redness, a bad taste, and sometimes a pus-filled bump. You may also feel general illness or have a low-grade fever.
With proper treatment, mild swelling clears in 2–7 days. Infections like a dental abscess or pericoronitis may take 1–2 weeks to resolve with antibiotics and professional care.
Yes. Untreated tooth decay spreads deeper into the tooth and can infect the pulp or surrounding gum tissue, causing localized inflammation and swelling directly around that tooth.
The most effective home remedy is a warm saltwater rinse — half a teaspoon of salt dissolved in 8 ounces of warm water, swished gently for 30 seconds, 3–4 times a day. Pair it with ibuprofen for pain relief and gentle flossing to remove debris.
Yes, absolutely. Partially erupted wisdom teeth are one of the most common causes of swollen back gum tissue. This condition is called pericoronitis and requires dental evaluation. It may need antibiotics, cleaning, or tooth extraction.
Yes. An alcohol-free antibacterial mouthwash helps reduce bacteria and soothe inflamed tissue. Avoid mouthwash with high alcohol content on irritated gums as it can worsen burning and dryness.
Gum disease develops slowly with widespread or progressive symptoms like bleeding, recession, and bone loss. An abscess appears more suddenly with intense localized pain, a pus-filled bump, possible fever, and a bad taste. A dentist and dental X-ray can confirm which one it is.
Why is my gum swollen around one tooth in the back? Now you know it is not always a single answer. The causes range from something as minor as trapped popcorn to something as serious as a spreading dental abscess or impacted wisdom tooth infection.
The key takeaway is this — localized gum swelling is your body telling you something specific is wrong in that exact spot. Early action makes all the difference. A saltwater rinse and ibuprofen can manage mild discomfort short-term, but they are not cures. If swelling lasts more than 48 hours, worsens, or comes with fever or facial swelling, call your dentist immediately.
Routine brushing, flossing, and professional cleanings twice a year are your strongest defense against all the causes listed here. Most of these conditions are preventable — and those that are not are far easier to treat when caught early.
Do not let a swollen gum become a dental emergency. Listen to what your mouth is telling you, act early, and work with your dentist to keep your gum health in top shape in 2026 and beyond.