Why does my tongue hurt is one of the most common oral health questions people search for in 2026. Your tongue works hard every single day — chewing, tasting, swallowing, and speaking — and when it hurts, everything becomes uncomfortable.
Tongue pain can range from a mild, short-lived sting to a persistent ache that hints at something deeper. Most cases are manageable with simple home care, but some need professional attention.

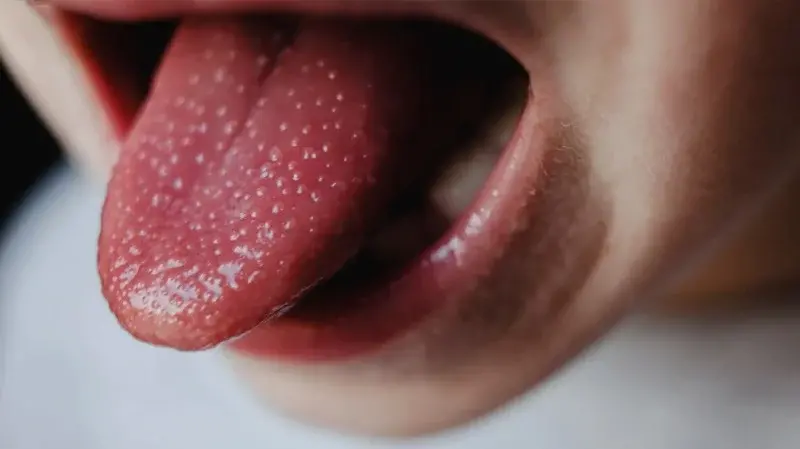
A normal tongue is pinkish-red on top with small raised bumps called papillae. The underside is smooth with a slightly bluish tone from visible veins.
The tongue should rest comfortably in the mouth without soreness, burning, or unusual patches. Any change in color, texture, or sensation deserves attention.
A healthy tongue should never ache, burn, or develop sores lasting more than one to two weeks.
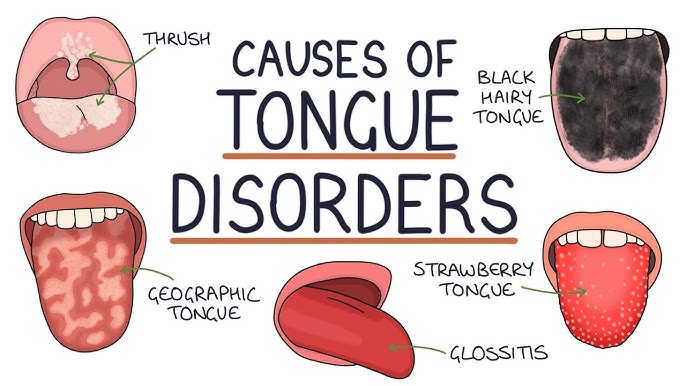
Understanding why your tongue hurts starts with identifying the location, type, and duration of the pain. Below are the most well-documented causes confirmed across top medical sources.
One of the most frequent causes of tongue pain is simply biting it. This happens while eating, talking, or even sleeping. The resulting sore can swell, sting, and take several days to heal.
Sharp teeth, chipped fillings, or ill-fitting dental appliances like braces or dentures can also scrape the tongue repeatedly. This constant friction delays healing and worsens pain.
Minor trauma usually heals on its own within three to seven days without any treatment.
Canker sores are small, round ulcers that appear inside the mouth, including on the tongue. They look white or yellow with a red border and cause a stinging, burning sensation.
Triggers include stress, hormonal changes, minor injuries, acidic foods like citrus and tomatoes, and vitamin deficiencies. They are not contagious and typically heal within seven to ten days.
If canker sores recur more than three times per year, a dentist or doctor should evaluate the pattern.
Burning mouth syndrome causes a continuous burning, tingling, or numb feeling on the tongue without any visible sore or lesion. The sensation can feel like you scalded your tongue on hot coffee.
It is more common in middle-aged and older women, especially after menopause. Possible triggers include hormonal changes, dry mouth, nerve damage, nutritional deficiencies, and certain medications.
There is no single cure, but treatments can reduce symptoms significantly.
Oral thrush is a fungal infection caused by an overgrowth of Candida yeast. It produces white or yellow patches on the tongue and inner cheeks that cause pain, a cotton-like feeling, and sometimes a loss of taste.
It is more common in people with weakened immunity, diabetes, or those who use corticosteroid inhalers or antibiotics. Treatment requires prescription antifungal medication.
Good oral hygiene and avoiding unnecessary antibiotic use help prevent thrush.
Low levels of vitamin B12, iron, folate, and zinc are closely linked to a sore or inflamed tongue. These nutrients are essential for maintaining healthy oral tissue.
Deficiencies can cause a condition called glossitis — inflammation of the tongue — where the tongue becomes smooth, pale, red, and painful. The tongue may also lose its normal bumpy texture.
Improving your diet or taking supplements under medical guidance usually resolves this type of tongue pain.
Geographic tongue is a harmless condition where smooth, red patches with white borders appear on the tongue, giving it a map-like appearance. The patches shift location from day to day.
Some people feel a burning or stinging sensation, especially when eating spicy or acidic foods. The exact cause is unknown, but there may be a link to psoriasis.
Anti-inflammatory medications or topical numbing agents can help manage discomfort.
Glossitis means inflammation of the tongue. It causes the tongue to swell, change color, and lose its normal surface texture. The tongue may appear smooth, red, and very tender.
Causes include low vitamin B levels, anemia, certain medications, infections, and allergic reactions. Treatment depends on the underlying cause and may involve antibiotics, antifungals, or dietary changes.
Untreated glossitis can make it difficult to eat, speak, or swallow properly.
A rushed sip of hot coffee or a bite of freshly baked food can scald the tongue. Burned tongue tissue becomes tender, swollen, and sensitive for several days.
This type of tongue pain typically resolves on its own within three to five days with cool foods and gentle care. Avoid further heat exposure while the tissue heals.
Cold water, ice chips, and soft foods speed up recovery significantly.
Braces, retainers, dentures, and sharp-edged crowns can continuously rub against the tongue, creating persistent soreness. The friction is often worse on the sides of the tongue where it makes frequent contact with hardware.
Pain from dental appliances will continue until the source of irritation is addressed. A dentist can smooth sharp edges or adjust the appliance.
Never ignore tongue pain linked to new or recently adjusted dental work.
Various infections can cause tongue pain. The herpes simplex virus causes clusters of painful blisters. Bacterial infections like syphilis produce mouth sores requiring antibiotics. Hand, foot, and mouth disease causes small painful ulcers throughout the mouth.
Fungal infections like oral thrush are among the most common. Each type requires a specific treatment — antifungals, antivirals, or antibiotics depending on the cause.
See a doctor if your tongue pain is accompanied by fever, visible pus, spreading sores, or a bad taste in the mouth.
Lie bumps are small, inflamed taste buds that appear as white or red bumps on the tongue. They are painful but usually disappear within a few days without treatment.
The exact cause is unclear, but stress and hormonal changes are common triggers. They are different from canker sores and do not spread to others.
Salt rinses and avoiding irritating foods can ease discomfort while they heal.
Oral lichen planus is a chronic inflammatory condition that causes pain, burning, and white lacy patches or open sores on the tongue and inner cheeks. It is an autoimmune condition.
It cannot be cured, but symptoms are managed with corticosteroid gels, mouthwashes, and immune-modulating medications. Regular dental monitoring is essential.
Flares are often triggered by stress, certain foods, or dental materials.
Food allergies and oral allergy syndrome can make the tongue hurt, swell, or tingle shortly after eating raw fruits, vegetables, or tree nuts. This is also called pollen-food syndrome.
Products like toothpastes and mouthwashes containing sodium lauryl sulfate or strong flavoring agents can also trigger tongue sensitivity or irritation.
Severe allergic reactions causing significant tongue swelling require emergency care immediately.
Grinding or clenching teeth during sleep puts pressure on the tongue, especially along its edges. Many people wake up with soreness along the sides of the tongue from pressing it against the teeth overnight.
A dentist may recommend a custom mouthguard to protect the tongue and teeth during sleep. Stress management also plays a key role in reducing grinding.
Persistent morning tongue pain with no visible sores is a strong signal of nighttime bruxism.
A persistent sore, lump, or lesion on the tongue that does not heal within two to three weeks could signal oral cancer. Risk factors include tobacco use, heavy alcohol consumption, and HPV infection.
Oral cancer may not cause pain in its early stages, making regular oral cancer screenings critically important. Early diagnosis leads to significantly better treatment outcomes.
See a dentist or doctor immediately if any sore on the tongue fails to heal after two to three weeks.
The location of your tongue pain can help narrow down the cause. Here is a quick reference:
| Location | Common Causes |
|---|---|
| Tip of tongue | Burns, biting, lie bumps, canker sores |
| Side of tongue | Dental appliances, sharp teeth, bruxism, canker sores |
| Underside of tongue | Canker sores, irritation, salivary gland issues |
| Back of tongue | Infections, tonsil issues, acid reflux |
| Entire tongue | Glossitis, nutritional deficiency, burning mouth syndrome |
| White patches | Oral thrush, leukoplakia, geographic tongue |
| Cause | Duration | Contagious | Needs Doctor? |
|---|---|---|---|
| Accidental bite | 3–7 days | No | Rarely |
| Canker sore | 7–14 days | No | If recurring |
| Burns from heat | 3–5 days | No | Rarely |
| Oral thrush | Weeks | No | Yes |
| Nutritional deficiency | Weeks to months | No | Yes |
| Burning mouth syndrome | Months to years | No | Yes |
| Geographic tongue | Recurring | No | Sometimes |
| Oral cancer | Does not heal | No | Immediately |
Most mild tongue pain responds well to home care. The following remedies are widely recommended and backed by dental experts.
Mix half a teaspoon of salt into one cup of warm water and rinse for 30 seconds two to three times per day. Salt has natural antiseptic properties that cleanse the tongue surface and reduce inflammation around canker sores and minor injuries.
This is the single most recommended home remedy across all major medical sources and works for nearly every type of tongue pain.
Apply a small ice chip directly to the painful area or eat cold yogurt, smoothies, or sorbet. Cold temperatures numb the nerve endings in the tongue and reduce swelling quickly.
Avoid chewing ice directly as this can damage teeth. Sipping cold water slowly throughout the day also helps maintain comfort.
Over-the-counter benzocaine gels such as Orajel or Zilactin-B create a temporary numbing barrier over sore spots. Apply directly to the painful area before meals to make eating more comfortable.
These are especially useful for canker sores and bite injuries. Follow package instructions and avoid swallowing the gel.
Mix one teaspoon of baking soda into half a cup of warm water and rinse gently. Baking soda neutralizes acids in the mouth and reduces inflammation, particularly helpful for canker sores and minor ulcers.
It can also be made into a paste and applied directly to a sore spot for targeted relief.
Both honey and aloe vera gel have natural anti-inflammatory and antibacterial properties. Applying a small amount directly to the sore area can reduce pain and speed up healing.
Pure aloe vera juice can also be used as a mouth rinse two to three times per day. Look for food-grade aloe vera products.
Swishing a tablespoon of coconut oil in the mouth for five to ten minutes then spitting it out may help reduce bacterial load and soothe a sore tongue. Coconut oil has antifungal, antibacterial, and antiviral properties.
This remedy is particularly helpful when tongue pain is related to oral thrush or general bacterial irritation.
Chamomile is believed to have anti-inflammatory properties. Rinsing with cooled strong chamomile tea or applying a wet chamomile tea bag directly to the sore area may provide mild relief.
This is a gentle option suitable for people sensitive to stronger treatments. Repeat two to three times daily.
If tongue pain is related to a nutritional deficiency, taking a vitamin B complex supplement or a multivitamin may help. Vitamin B12, iron, folate, and zinc are the most commonly linked to tongue inflammation.
Always consult a doctor before starting supplements, especially if you suspect a specific deficiency. Blood tests can confirm exactly what you are low in.
Until your tongue heals, avoid spicy foods, acidic fruits like citrus and pineapple, salty snacks, and very hot beverages. These foods worsen inflammation and slow healing.
Stick to soft, mild foods like mashed potatoes, yogurt, oatmeal, bananas, and cooked vegetables. Staying well-hydrated also prevents dryness that can intensify soreness.
| Eat These | Avoid These |
|---|---|
| Yogurt, smoothies | Citrus fruits, pineapple |
| Oatmeal, mashed potatoes | Spicy sauces, hot peppers |
| Bananas, avocado | Hot coffee or tea |
| Cooked soft vegetables | Salty chips, crackers |
| Ice cream, sorbet | Tomato-based sauces |
| Cool water | Alcohol-based mouthwash |
Most tongue pain is minor and heals within one to two weeks. However, certain symptoms indicate that professional evaluation is necessary and should not be delayed.
See a dentist or doctor if any of the following apply:
The sore or pain has lasted more than seven to ten days without improvement. The sore is growing larger, bleeding, or hardening. You notice white, red, or dark patches that do not rub off. Your tongue feels persistently swollen or unusually smooth. Pain spreads to the throat, jaw, or ear. Swallowing, speaking, or eating becomes noticeably difficult. You have a visible lump or thickening on or under the tongue. The sore returns repeatedly in the same location.
Any lesion that has not healed within two to three weeks must be professionally examined to rule out oral cancer. Early detection is the single biggest factor in successful treatment outcomes.

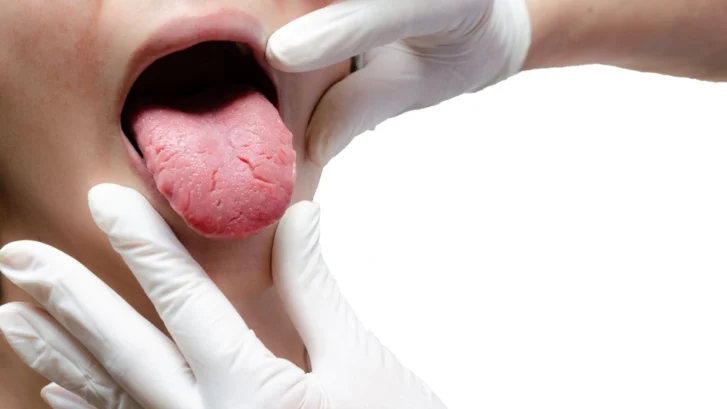
A healthcare provider will begin with a visual examination of the tongue and a full oral health history. They will ask about your diet, stress levels, medications, oral hygiene habits, and how long the pain has lasted.
Depending on what they find, they may recommend an oral swab to check for fungal or viral infections, blood tests to identify deficiencies or systemic illness, or a biopsy if a lesion looks suspicious or fails to heal.
Treatment depends entirely on the underlying cause and may range from a simple vitamin prescription to antifungal medication or further specialist referral.
When home remedies are not enough, medical treatment targets the specific cause of tongue pain.
Antifungal medications like fluconazole or clotrimazole treat oral thrush effectively within one to two weeks.
Antibiotics are prescribed when a bacterial infection such as syphilis or a severe dental abscess is responsible for tongue pain.
Corticosteroid gels or mouthwashes reduce inflammation for oral lichen planus, severe canker sores, and geographic tongue.
Antiviral medications help manage outbreaks caused by the herpes simplex virus, reducing both severity and duration.
Vitamin injections or supplements correct nutritional deficiencies that cause glossitis and chronic tongue soreness.
Mouthguards protect the tongue and teeth from nighttime grinding pressure for people with bruxism.
Prevention is always easier than treatment. These daily habits significantly reduce your risk of developing tongue pain.
Brush your teeth twice daily with a soft-bristled toothbrush and avoid aggressive scrubbing. Floss once daily and consider using a tongue scraper to remove bacteria from the surface.
Get regular dental cleanings and ask your dentist to perform oral cancer screenings at each visit. Early detection of any lesion is critical.
Avoid tobacco in all forms. Smoking and chewing tobacco irritate oral tissue and significantly raise the risk of oral cancer. Limit alcohol consumption for the same reason.
Eat a balanced diet rich in vitamin B12, iron, folate, and zinc. Include lean meats, leafy greens, eggs, dairy, and nuts in your regular meals.
Manage stress through regular exercise, adequate sleep, and relaxation techniques. Stress is one of the most commonly reported triggers for canker sores and burning mouth syndrome.
Stay well hydrated throughout the day. Dry mouth reduces saliva, which is a natural protectant and cleanser for oral tissues.
Children can also experience tongue pain, most commonly from biting, hand-foot-mouth disease, and oral thrush. Infants with thrush may appear fussy during feeding and have visible white patches on the tongue.
Canker sores are also common in children and teenagers, often linked to stress or nutritional deficiencies. Most childhood tongue problems resolve quickly with gentle care and do not require medical intervention.
See a pediatrician if tongue pain in a child lasts more than a week, is accompanied by fever, or prevents eating or drinking normally.
The tongue is sometimes called a mirror of the body. Changes in the tongue can reflect broader health issues that go beyond the mouth alone.
Autoimmune conditions like lupus, Sjögren’s syndrome, and Behçet’s disease can cause painful sores or ulcers in the mouth including the tongue. Diabetes increases the risk of oral thrush and slows healing of any mouth sore. Thyroid disorders and anemia can both manifest with tongue inflammation.
If you have a known systemic condition and develop tongue pain, report it to your doctor during your next visit so they can assess whether it is related.
Certain medications can cause or worsen tongue pain as a side effect. Antibiotics disrupt the natural balance of oral bacteria and fungi, increasing thrush risk. Some blood pressure medications cause dry mouth, which worsens tongue soreness. Chemotherapy often causes painful mouth sores as a well-documented side effect.
If you suspect a medication is causing your tongue pain, speak with your prescribing doctor. Never stop a prescribed medication without medical advice. Alternative drugs or protective rinses may be available.
Stress is one of the most underappreciated triggers of tongue pain. It is directly linked to canker sore outbreaks, burning mouth syndrome flares, and increased bruxism, all of which cause significant tongue discomfort.
Stress also weakens the immune system, making the body more vulnerable to oral infections like thrush and herpes outbreaks. Practicing daily stress management — through exercise, mindfulness, or adequate sleep — can noticeably reduce how often tongue pain occurs.
Tongue pain without an obvious cause is often linked to burning mouth syndrome, nutritional deficiencies, or stress-triggered canker sores. A blood test and dental exam can identify most hidden causes.
One-sided tongue pain usually comes from local irritation like a small bite, a canker sore, or a sharp dental appliance rubbing against that side. Nerve conditions can also cause it.
Tip pain commonly results from accidental biting, lie bumps (inflamed taste buds), burns from hot food, or canker sores that form at the very front of the tongue.
Eating triggers pain because food and drink contact the inflamed or injured area. Acidic, spicy, or very hot foods are the worst offenders and significantly worsen existing sores.
Minor tongue pain from biting or a canker sore heals in seven to fourteen days. Pain lasting longer than two weeks should be evaluated by a dentist or doctor.
Yes. Low levels of vitamin B12, iron, folate, and zinc are among the most common causes of chronic tongue soreness and glossitis. A simple blood test confirms deficiencies.
A painful sore alone is rarely oral cancer, but a sore or lump on the tongue that does not heal within two to three weeks must be professionally examined. Early detection is critical.
A warm salt water rinse, benzocaine topical gel, and cold soft foods provide the fastest relief for most common causes. Avoiding spicy and acidic foods during healing also speeds recovery.
Yes. Stress triggers canker sore outbreaks, worsens burning mouth syndrome, and increases teeth grinding, all of which create or worsen tongue pain. Managing stress reduces recurrence.
See a doctor if pain lasts more than seven to ten days, if you notice white, red, or dark patches, if there is a lump on the tongue, or if eating and speaking become significantly difficult.
Why does my tongue hurt is a question with many possible answers, but most cases are manageable with the right care.
The majority of tongue pain comes from everyday causes — an accidental bite, a canker sore, a hot drink, or a mild nutritional deficiency — and heals within one to two weeks with basic home treatment. Salt rinses, cool foods, topical gels, and avoiding food irritants resolve most cases quickly.
The key is knowing the difference between minor pain and persistent symptoms that signal something more serious.
Any sore or lesion that does not heal within two to three weeks, any visible lump, or any pain accompanied by difficulty swallowing deserves professional evaluation without delay. Oral cancer caught early is far more treatable than cancer found late.
Maintain good oral hygiene, eat a nutrient-rich diet, manage stress, and visit your dentist regularly. Your tongue works hard every day — take care of it and it will take care of you.