
Why are hospitals cold? It is one of the first things patients and visitors notice the moment they walk through the doors.
That chill is not an accident, a broken thermostat, or an oversight by facilities management.
Hospitals are cold on purpose — and the reasons are rooted in infection control, patient safety, equipment performance, and staff efficiency.
In 2026, strict ASHRAE and Joint Commission standards govern exactly how cold different areas must be.

Most people assume hospitals are cold simply because of powerful air conditioning systems. That assumption is only partially right.
The actual drivers are infection control, humidity management, equipment performance, and staff comfort — all working together. Every zone in a hospital has a defined temperature range tied to a specific clinical or operational purpose.
The cold is deliberate, regulated, and enforced by multiple national standards organizations.
Hospital temperatures vary significantly by department. There is no single thermostat setting for an entire facility.
| Hospital Zone | Recommended Temperature | Humidity Range |
|---|---|---|
| Operating Rooms | 68°F – 75°F (20°C – 24°C) | 20% – 60% |
| ICU / Intensive Care | 70°F – 75°F (21°C – 24°C) | 30% – 60% |
| General Patient Rooms | 70°F – 75°F (21°C – 24°C) | 30% – 60% |
| Emergency Department | 68°F – 73°F (20°C – 23°C) | 30% – 60% |
| Endoscopy Suites | 68°F – 73°F (20°C – 23°C) | 20% – 60% |
| Recovery / PACU | 70°F – 75°F (21°C – 24°C) | 30% – 60% |
| Laboratory Areas | 65°F – 72°F (18°C – 22°C) | 30% – 50% |
| Pharmacy / Drug Storage | Below 75°F (24°C) | Below 60% |
These ranges are set by ASHRAE Standard 170 (Ventilation of Healthcare Facilities) and enforced by the Joint Commission, CMS, and state health departments.
Bacteria and viruses thrive in warm, humid environments. Most pathogenic microorganisms reproduce most rapidly between 77°F and 86°F (25°C – 30°C).
Cooler temperatures slow bacterial cell division, reduce microbial activity on surfaces, and lower pathogen concentration in the air. This directly reduces the risk of hospital-acquired infections (HAIs).
Hospital-acquired infections (HAIs) are infections patients develop during a hospital stay that were not present on admission. They typically appear 48 hours or more after admission.
Common HAIs include surgical site infections (SSI), central line-associated bloodstream infections (CLABSI), catheter-associated urinary tract infections (CAUTI), and hospital-acquired pneumonia (HAP). The CDC’s National Healthcare Safety Network monitors these infections closely across all U.S. healthcare facilities.
Operating rooms are typically the coldest spaces in any hospital — maintained at 68°F to 75°F with humidity between 20% and 60% per ASHRAE 170 guidelines.
This environment minimizes bacterial contamination of open wounds, surgical instruments, and sterile fields. The risk of surgical site infections increases sharply when OR temperatures rise above the recommended range.
Some surgeons prefer even colder conditions — as low as 60°F – 65°F. These lower temperatures require specialized HVAC systems with desiccant wheels or low-temperature chilled water systems, since standard hospital HVAC cannot maintain humidity compliance at those extremes.

Warm air holds more moisture. When warm, humid air meets cooler surfaces — equipment, walls, floors, ceilings — it creates condensation.
Condensation is a breeding ground for mold, mildew, and bacterial colonies. In a clinical environment, moisture on sterile surfaces or medical instruments directly compromises patient safety.
Cooler air holds less moisture, which naturally keeps relative humidity lower throughout the building. The CDC and ASHRAE both specify humidity must stay below 60% in most clinical areas for this exact reason.
Hospital lab environments are especially sensitive to humidity. Laboratory workers often report wearing hoodies and zip-ups year-round because their zones must stay at optimal temperature and humidity to protect sample integrity and testing accuracy.
Medical imaging machines, diagnostic analyzers, and surgical instruments are precision instruments. Excess moisture causes corrosion, calibration errors, and equipment failure.
Keeping the hospital cool and dry ensures that multi-million-dollar diagnostic and treatment equipment functions reliably every time it is needed.
Nurses, surgeons, and other clinical staff are physically active throughout their entire shift. They walk miles per day, lift patients, perform procedures, and respond to emergencies.
On top of that, they wear multiple layers — scrubs, sterile gowns, gloves, masks, and sometimes full personal protective equipment (PPE). This layering traps significant body heat.
If hospitals were kept at room temperature (72°F – 76°F), clinical staff in full PPE would overheat rapidly. Overheating causes fatigue, reduced concentration, and impaired decision-making — serious risks in a high-stakes environment.
Cooler ambient temperatures offset the heat generated by protective clothing, allowing staff to remain alert and physically functional across long 12-hour shifts.
Bright surgical lights generate substantial heat directly over the operating table. Surgeons and scrub nurses stand under these lights for hours during complex procedures.
Without cold air conditioning compensating for the heat from surgical lighting, operating rooms would become uncomfortably warm for the surgical team. The cold environment keeps the entire OR team focused and physically comfortable throughout lengthy procedures.
Hospital equipment — MRI machines, CT scanners, X-ray units, patient monitors, anesthesia machines, and laboratory analyzers — generates significant heat during operation.
Heat is the primary enemy of electronic components. Elevated temperatures cause processors to throttle performance, sensors to drift in accuracy, and circuit boards to degrade faster.
Cooler ambient temperatures dissipate this equipment-generated heat more effectively, keeping every machine running within its designed operating parameters.
Many medications, vaccines, and biological samples require strict temperature control to remain effective. ASHRAE Standard 170 specifies that sterile storage areas must stay below 75°F with humidity no higher than 60%.
Pharmacy areas within hospitals are often even colder, since certain drugs degrade rapidly if exposed to higher temperatures. Blood products, certain biologics, and chemotherapy agents have tight storage temperature windows that must be maintained continuously.
In 2026, hospitals use automated remote temperature monitoring systems throughout their facilities. Digital data loggers record temperature and humidity readings at minimum every 30 minutes.
These systems send automatic alerts when any zone drifts outside its required range. The Joint Commission requires continuous monitoring of operating rooms and medication storage areas, and inspectors typically accept only temporary deviations resolved within 24 hours.
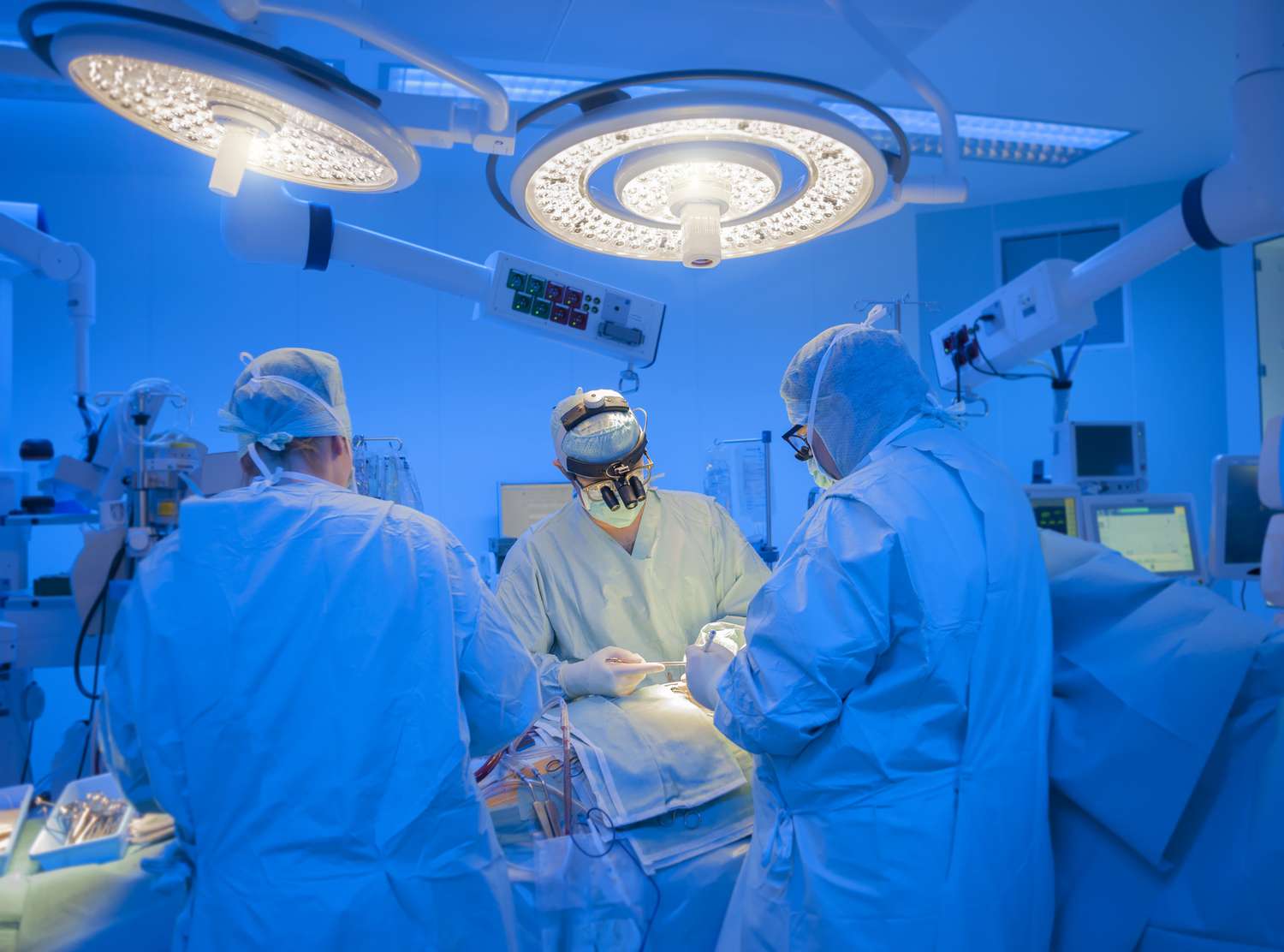 5: Airflow, Ventilation, and Positive Pressure Systems
5: Airflow, Ventilation, and Positive Pressure Systems
Hospital HVAC systems are not the same as standard commercial building air conditioning. They are engineered to achieve multiple clinical goals simultaneously — temperature control, humidity management, air filtration, and directional airflow.
Most clinical areas require a minimum of 15 to 20 air changes per hour (ACH). Operating rooms often require 20+ ACH. This constant air turnover keeps airborne pathogens diluted and maintains sterile conditions.
Operating rooms and immunocompromised patient rooms use positive pressure — air flows outward when the door opens, preventing outside contaminants from entering.
Isolation rooms for infectious patients use negative pressure — air flows inward, preventing airborne pathogens from escaping into hallways. These pressure differentials are maintained by the same HVAC systems that control temperature and humidity.
High-efficiency particulate air (HEPA) filters capture 99.97% of particles including bacteria, mold spores, and many viruses. These filters work best in environments with controlled temperature and humidity — another reason why hospital cold air is not just comfort-related but deeply tied to air quality and infection control.
When you are sick, your metabolism changes. Fever, medications, anesthesia, and illness itself all affect your body’s thermoregulation.
Anesthesia is particularly disruptive — it impairs the hypothalamus’s ability to regulate core body temperature. Patients under general anesthesia are highly susceptible to perioperative hypothermia, which is why warming blankets and forced-air warming systems are standard in surgical and recovery settings.
The classic thin hospital gown was designed for clinical access — not warmth. It exposes the back, provides minimal insulation, and leaves limbs largely uncovered.
Combined with cool room temperatures, IV fluids (which enter the body at room temperature), and reduced mobility, patients feel significantly colder than the thermostat reading would suggest.
Intravenous fluids are typically stored and administered at room temperature — around 68°F – 72°F. When these fluids enter the bloodstream, they cool the body from the inside.
Large volumes of IV fluids during surgery or trauma care can significantly drop core body temperature. This is one reason anesthesia teams actively monitor core body temperature and use warming interventions throughout surgical procedures.
Intensive care units run at 70°F – 75°F, consistent with general clinical recommendations. But the ICU feels colder to patients because they are largely immobile, sedated, connected to monitoring equipment, and often receiving IV fluids continuously.
Staff in ICUs are extremely active — monitoring multiple patients, adjusting equipment, responding to alarms, and performing hands-on care. The cooler environment supports staff performance while clinical warming interventions manage individual patient body temperature.
Controlled cooling is actually used as a medical treatment in specific situations. Therapeutic hypothermia (targeted temperature management) is used after cardiac arrest to protect the brain from oxygen deprivation injury.
Patients undergoing therapeutic hypothermia are intentionally kept at core temperatures of 89°F – 93°F (32°C – 34°C). Monitoring these patients requires precise environmental temperature control — another reason ICU environments must be cold and stable.
Emergency rooms receive a constant flow of patients, families, staff, and equipment. Staff are continuously moving — triaging, transporting, assessing, and treating patients. The physical activity of a busy ER generates significant body heat.
Cold temperatures keep the ER comfortable for staff during high-intensity work. Equipment running continuously also contributes heat that the HVAC system must offset.
Trauma bays — where the most invasive emergency procedures occur — are kept closest to operating room standards. Open wounds during trauma resuscitation carry high infection risk, and cool temperatures help minimize pathogen activity on exposed tissue and instruments.
Newborns, especially premature infants, cannot regulate their own body temperature. The neonatal ICU (NICU) is kept warmer than the rest of the hospital — typically 72°F – 78°F — and individual incubators maintain even warmer microenvironments for each infant.
Premature babies lose heat extremely rapidly and can suffer serious complications from even mild hypothermia. Every NICU room is designed to offset this vulnerability.
Children have a higher surface area relative to body mass than adults, making them lose heat faster. Pediatric wards are generally maintained at the warmer end of clinical temperature recommendations to keep younger patients comfortable and support their thermoregulation.
Multiple organizations establish and enforce hospital temperature standards in the United States:
| Organization | Role |
|---|---|
| ASHRAE | Sets Standard 170 for ventilation and temperature in healthcare facilities |
| CDC | Recommends temperature ranges by zone for infection control |
| Joint Commission | Enforces compliance through accreditation surveys |
| CMS | Links compliance to Medicare and Medicaid certification |
| AORN | Provides OR-specific guidelines for nursing and surgical teams |
| FGI | Sets design and construction standards for new healthcare facilities |

If an operating room drifts outside its required temperature or humidity range, staff must document the deviation immediately. The Joint Commission typically accepts temporary deviations resolved within 24 hours.
Persistent non-compliance puts a hospital’s Joint Commission accreditation at risk — which in turn threatens its Medicare and Medicaid certification. The financial and regulatory consequences are severe, making temperature compliance a genuine institutional priority.
Warmed blankets are one of the simplest and most effective patient comfort tools in a hospital. Many facilities use blanket warmers that heat blankets to safe therapeutic temperatures before delivery to patients.
Forced-air warming blankets — used in operating rooms and recovery rooms — actively circulate warm air against the patient’s skin to raise peripheral and core body temperature during and after surgery.
Surgical tables and patient beds in some units are equipped with warming pads or heated mattress overlays. These devices maintain the patient’s surface temperature without affecting the ambient room temperature needed for infection control.
Hospitals increasingly inform patients before admission that clinical areas will be cold and to bring personal items — socks, a robe, or a personal blanket — to supplement clinical warming measures.
This proactive communication reduces patient distress and complaint, and helps patients arrive mentally prepared for the temperature environment they will experience.
| Tip | Why It Helps |
|---|---|
| Bring warm socks | Feet lose heat rapidly on cold tile floors |
| Bring a personal robe or light layer | Hospital gowns provide minimal insulation |
| Ask for extra blankets | Most hospitals have warming blanket supplies |
| Stay hydrated | Dehydration makes you feel colder |
| Request a warming pad if available | Especially useful during long procedures or recovery |
| Tell your nurse if you are shivering | Shivering can signal problematic core temperature loss |
Patients should always tell their care team if they feel excessively cold. Uncontrolled shivering increases oxygen consumption and metabolic demand — both of which can complicate recovery from illness or surgery.
Research suggests that cold environments can increase patient anxiety. Patients who feel physically cold tend to rate their pain higher and report lower satisfaction with their care experience.
Addressing a patient’s thermal comfort is not just a nicety — it is a genuine component of quality care. Many hospitals now include thermal comfort as a standard nursing assessment alongside pain level, vital signs, and mobility.
Human beings associate warmth with safety, comfort, and care at a very fundamental level. When patients feel cold and exposed in a thin gown, the sensation reinforces vulnerability.
Providing warming interventions — even a simple heated blanket — has been shown to improve patient satisfaction scores, reduce anxiety before procedures, and improve cooperation with clinical staff.
Federal energy and construction policy changes in 2026 have increased attention to healthcare facility energy efficiency. Modern hospital HVAC systems are being designed to meet both clinical temperature requirements and stricter energy performance standards simultaneously.
New construction guidelines from the Facility Guidelines Institute (FGI) reflect this dual mandate — maintaining ASHRAE 170 clinical compliance while reducing overall energy consumption per square foot.
The COVID-19 pandemic accelerated investment in hospital HVAC infrastructure. Many facilities upgraded filtration systems, increased air change rates, and added ultraviolet germicidal irradiation (UVGI) systems to operating rooms and high-risk clinical zones.
These upgrades work best in cooler, humidity-controlled environments — reinforcing rather than replacing the clinical case for cold hospital temperatures.
In 2026, hospital temperature monitoring uses IoT-connected sensors with cloud-based dashboards, real-time alerts, and automated compliance reporting. Facilities can now track and document thousands of temperature and humidity readings per day across every clinical zone.
This precision monitoring means any deviation from required ranges is detected and corrected faster than ever before — making hospital temperature management more reliable and defensible during regulatory surveys.
Hospitals are cold to prevent bacterial growth, control humidity, protect medical equipment, and keep active clinical staff comfortable. Most public buildings prioritize occupant comfort; hospitals prioritize infection control and clinical function.
Operating rooms must be maintained at 68°F to 75°F (20°C to 24°C) with relative humidity between 20% and 60%, per ASHRAE Standard 170, enforced by the Joint Commission and CMS.
Yes. Most pathogenic bacteria reproduce most rapidly at 77°F to 86°F. Cooler temperatures slow bacterial cell division and reduce microbial activity on surfaces and in the air, directly lowering infection risk.
Illness, anesthesia, thin hospital gowns, limited mobility, and room-temperature IV fluids all lower how warm a patient feels. The body’s thermoregulation is often impaired during illness and medical procedures.
Yes. NICUs are kept at 72°F – 78°F for premature infants, and pediatric rooms trend warmer. Operating rooms and labs are the coldest, while patient rooms and recovery areas are maintained at moderate clinical temperatures.
Patients can ask for extra blankets, warming pads, or additional warming measures. Individual room temperature cannot usually be changed because it is tied to building-wide clinical HVAC systems that serve infection control and equipment needs.
Lab areas must maintain tighter temperature and humidity control to protect sample integrity and the accuracy of diagnostic equipment. Lab workers commonly wear extra layers due to the colder conditions required for their environment.
Not if managed properly. Hospitals use warming blankets, heated mattresses, and forced-air warming systems to protect patient body temperature. However, unmanaged patient hypothermia does carry real risks, including surgical site infections and impaired immune response.
ERs are cold for the same core reasons as the rest of the hospital — infection control, equipment performance, and staff comfort. High staff activity levels, continuous equipment operation, and trauma bay requirements all drive ER temperatures toward the cooler end of the recommended range.
Most countries follow similar clinical guidelines for operating rooms (20°C – 24°C). The specific feel of coldness may vary by country depending on general patient room standards, climate, building design, and local regulatory requirements.
Why are hospitals cold? The answer goes far deeper than a preference for air conditioning.
Cold temperatures in hospitals are a carefully engineered clinical tool — one that simultaneously controls bacterial growth, manages humidity, protects equipment, offsets the heat of medical lighting and active staff, and supports precise infection control across every zone of the facility.
In 2026, ASHRAE Standard 170, Joint Commission accreditation requirements, and CDC infection control guidelines all mandate and enforce these temperatures with precision monitoring systems that never stop running.
Patients who feel cold in hospitals are not being neglected — they are inside a clinical environment designed above all to keep them safe.
Knowing why the cold exists makes it easier to ask for a warm blanket, understand what your care team is managing, and appreciate that the chill in the air is part of the medicine.