Why are my gums bleeding is one of the most searched dental questions in 2026 — and for good reason. Bleeding gums are rarely “just irritation.”
They are your body’s early warning system, signaling that something beneath the surface needs attention. Whether it happens when you brush, floss, or even randomly without any contact, gum bleeding is almost never normal.
Understanding the root causes, recognizing the warning signs, and knowing when to act can save your teeth, your smile, and even your overall health.
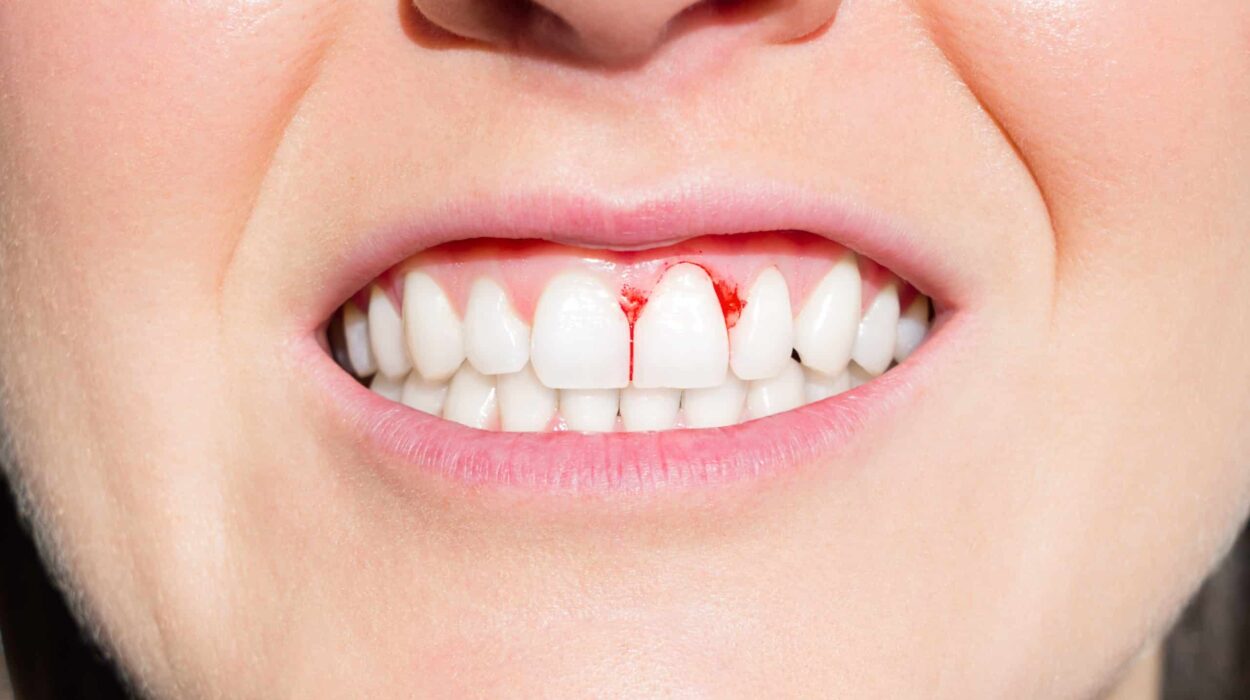
Bleeding gums happen when the soft tissue surrounding your teeth becomes inflamed, irritated, or infected. Inflamed gum tissue has fragile blood vessels that break easily under the slightest pressure — from a toothbrush, floss, or even food.
Healthy gums are firm, pale pink, and do not bleed during regular brushing or flossing. If yours do, that is your mouth asking for help.
The medical term for gum tissue is the gingiva. When it becomes inflamed, the condition is called gingivitis. Left untreated, it progresses to periodontitis — a far more serious infection that damages the bone and tissue holding your teeth in place.
Plaque is a sticky, colorless film of bacteria that forms on your teeth throughout the day. When plaque is not removed by brushing and flossing, it builds up along the gumline and irritates the surrounding tissue.
Your immune system responds by inflaming the gums. This inflammation makes the blood vessels in your gum tissue more fragile and prone to bleeding.
If plaque is not removed within 24 to 72 hours, it hardens into tartar (also called calculus). Tartar cannot be removed at home — only a professional dental cleaning can eliminate it.
Gingivitis is the earliest and most reversible form of gum disease. At this stage, gums appear red and swollen and bleed easily during brushing or flossing.
The good news is that gingivitis is fully reversible with consistent oral hygiene and professional cleaning. The bad news is that most people ignore the bleeding until it progresses further.
If gingivitis is left untreated, it advances into periodontitis. At this stage, the infection moves below the gumline and starts destroying the bone and connective tissue that anchor your teeth.
Gums begin to pull away from the teeth, forming deep pockets where bacteria thrive. Teeth can become loose or even fall out. This stage requires professional intervention — it cannot be reversed at home.
Many people believe harder brushing equals cleaner teeth. This is a myth. Aggressive brushing traumatizes delicate gum tissue and causes bleeding, recession, and enamel wear.
The correct technique is gentle circular motions with a soft-bristled toothbrush, angled at 45 degrees toward the gumline. A back-and-forth scrubbing motion damages gums every single time.
If you have just started flossing after a long gap, your gums may bleed for the first few days. This happens because the gum tissue is inflamed from accumulated plaque between teeth.
This bleeding is temporary. With consistent daily flossing, it typically stops within 3 to 10 days as gums tighten and heal. If it continues past two weeks, see a dentist.
Hormonal fluctuations during puberty, pregnancy, and menopause cause gums to become more sensitive and reactive to bacteria. Pregnancy gingivitis is a well-documented condition that affects many expectant mothers.
Increased blood flow to the gums during pregnancy makes them puff up and bleed more easily. This does not mean gum disease is inevitable — consistent oral hygiene keeps it under control.
Blood thinners such as warfarin, aspirin, and certain antidepressants reduce your blood’s ability to clot. This makes bleeding gums more likely and more prolonged.
Always tell your dentist which medications you are taking. They will adjust their approach to your care accordingly.
Low levels of Vitamin C and Vitamin K are directly linked to gum bleeding. Vitamin C supports gum tissue strength and wound healing. Vitamin K supports proper blood clotting.
A severe Vitamin C deficiency leads to scurvy — a condition where gums swell, bleed, and teeth become loose. While rare today, mild deficiencies are more common than many people realize.
| Vitamin | Role in Gum Health | Food Sources |
|---|---|---|
| Vitamin C | Strengthens gum tissue, supports healing | Citrus fruits, strawberries, bell peppers, broccoli |
| Vitamin K | Helps blood clot properly | Spinach, kale, leafy greens |
| Vitamin D | Reduces inflammation, supports immune response | Sunlight, fatty fish, fortified foods |
| B12 | Supports red blood cell production | Eggs, dairy, meat |
Uncontrolled blood sugar makes it harder for your body to fight infections, including gum infections. People with diabetes are significantly more prone to gum disease, and gum disease in turn makes blood sugar harder to control — creating a dangerous cycle.
Swollen or bleeding gums in a diabetic patient are a serious signal that needs prompt attention from both a dentist and a physician.
Smoking and chewing tobacco reduce blood flow to the gums and weaken the immune system. This creates the ideal environment for bacterial growth along the gumline.
A particularly dangerous aspect of tobacco use is that it can mask the early signs of gum disease — including bleeding — by suppressing the normal inflammatory response. By the time symptoms become visible, the disease may be significantly advanced.
Chronic stress suppresses your immune system, making it harder to fight off bacterial infections in the gums. Research has consistently linked high stress levels to increased inflammation throughout the body, including in gum tissue.
In less common cases, bleeding gums can point to more serious systemic issues:
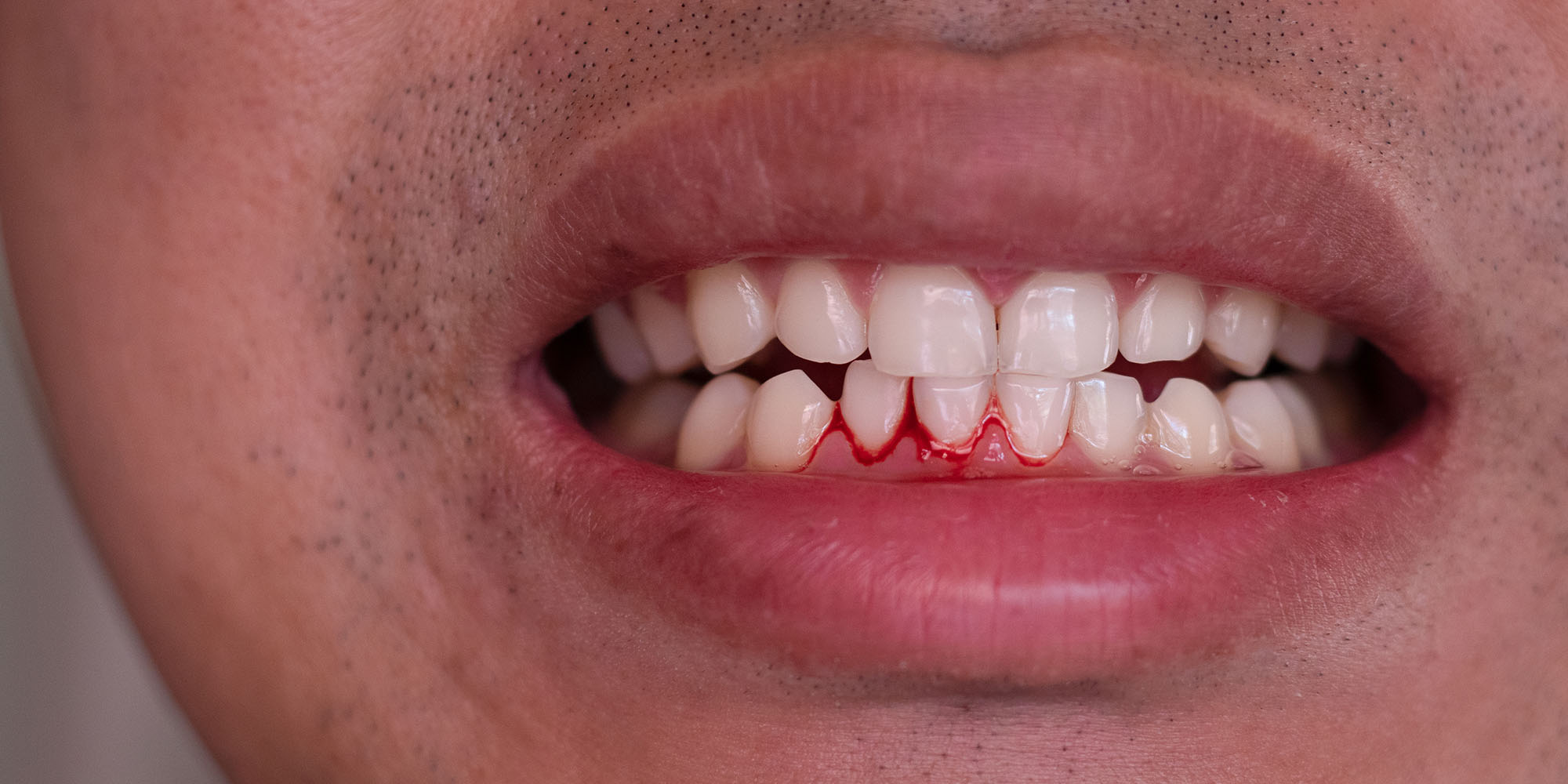
Occasional bleeding from brushing too hard is one thing. Gums that bleed consistently every time you brush, regardless of technique, are telling you that inflammation has taken hold.
Consistent bleeding is the hallmark symptom of gingivitis. Do not wait and hope it resolves on its own.
If your gums bleed without brushing, flossing, or eating — just randomly — this is a serious red flag. Spontaneous bleeding can indicate advanced periodontitis, a blood clotting disorder, or a systemic condition like leukemia.
This type of bleeding warrants an urgent dentist visit, not a wait-and-see approach.
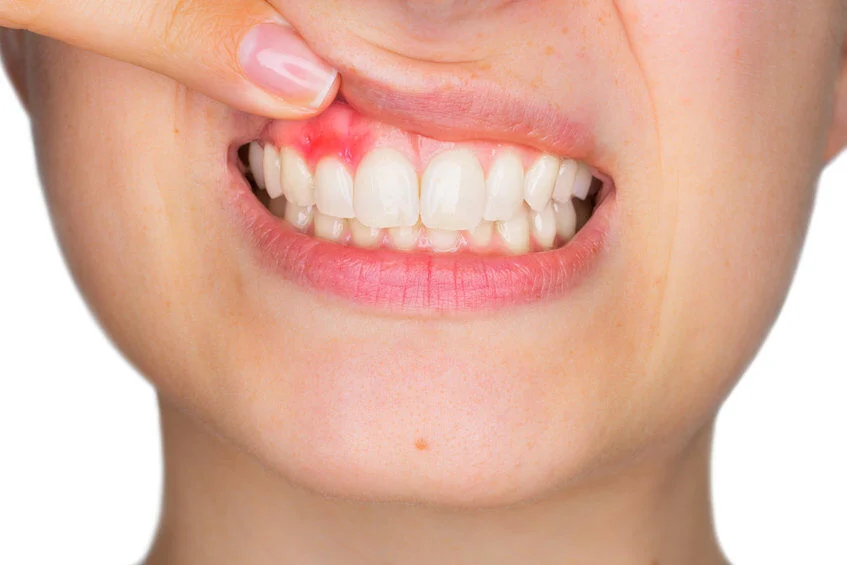
Healthy gums are light pink and firm. Gums that appear deep red, look shiny, feel puffy to the touch, or seem to bulge along the base of the teeth are actively inflamed.
Redness and swelling alongside bleeding is the classic trio of early gum disease. Catching it at this stage is the easiest and least expensive time to treat it.
Bad breath caused by bacteria in the mouth — known as halitosis — is a direct companion to gum disease. The bacteria living in inflamed gum pockets release sulfur compounds that cause a persistent, foul odor.
If mouthwash provides only temporary relief and the bad breath returns quickly, the source is likely bacterial buildup deep along the gumline.
Gum recession — where the gum tissue pulls back and exposes more of the tooth root — is a sign that gum disease is advancing. It creates deeper pockets between teeth and gums where bacteria accumulate unchecked.
Receding gums also cause increased tooth sensitivity to cold or hot foods and drinks. This is not a cosmetic issue — it is a structural one.
Adult teeth should never feel loose. If one or more teeth feel wobbly, shift position, or you notice gaps forming between teeth, the bone supporting them may already be deteriorating due to periodontitis.
This is a late-stage warning sign and requires immediate professional treatment to prevent tooth loss.
Pus oozing from between the gum and tooth is a sign of a bacterial infection — specifically, a periodontal abscess. It may come with pain, swelling, and a bad taste in the mouth.
This is a dental emergency. Do not delay seeking treatment.
The connection between gum disease and systemic health is well-established by 2026 research. Chronic gum inflammation does not stay in the mouth.
Bacteria from infected gums can enter the bloodstream and contribute to the buildup of arterial plaque. Research has linked chronic periodontitis to an elevated risk of heart attack and stroke.
The relationship between diabetes and gum disease is bidirectional. Gum disease raises blood sugar levels and makes diabetes harder to manage. Controlling one helps control the other.
Untreated periodontal disease during pregnancy has been associated with an increased risk of preterm birth and low birth weight. Pregnant women are strongly encouraged to maintain dental cleanings throughout their pregnancy.
Bacteria inhaled from an infected mouth can reach the lungs and worsen conditions like pneumonia and chronic obstructive pulmonary disease (COPD).
| Stage | Name | Key Signs | Reversible? |
|---|---|---|---|
| Stage 1 | Gingivitis | Red, puffy gums; bleeds when brushed | Yes — with proper care |
| Stage 2 | Early Periodontitis | Gum pockets forming; slight bone loss | Partially — with professional help |
| Stage 3 | Moderate Periodontitis | Deeper pockets; noticeable bone loss | Manageable, not fully reversible |
| Stage 4 | Advanced Periodontitis | Loose teeth; significant bone loss; tooth loss risk | Requires surgery; irreversible damage |
Use a soft-bristled toothbrush and gentle circular motions angled at 45 degrees toward the gumline. Brush for two full minutes. Replace your toothbrush every three months or sooner if the bristles fray.
Electric toothbrushes with pressure sensors can be especially useful for people who tend to brush too aggressively.
Many people stop flossing when their gums bleed. This is the opposite of what you should do. Flossing removes the plaque between teeth that a toothbrush cannot reach.
If you have just started flossing, bleeding for 3 to 5 days is expected. Keep going. It stops as inflammation resolves.
Dissolve half a teaspoon of table salt in a cup of warm water. Swish for 30 seconds, then spit. Do this once or twice a day.
Saltwater reduces bacteria, soothes inflamed tissue, and has a mild astringent effect that helps gums heal. It is not a cure, but it is a helpful daily addition.
An antimicrobial rinse can reduce bacteria along the gumline when used after brushing and flossing — not instead of them. Look for products with chlorhexidine or cetylpyridinium chloride.
Mouthwash is never a standalone treatment. It works as support, not a substitute for mechanical cleaning.
Load up on citrus fruits, strawberries, bell peppers, broccoli, spinach, and kale. These foods directly support gum tissue strength and healthy blood clotting.
Avoid excessive refined sugar and simple carbohydrates — they feed the bacteria responsible for plaque buildup.
Quitting tobacco is one of the most impactful things you can do for your gum health. Even cutting back reduces the bacterial burden and allows better blood flow to the gums.
High cortisol levels from chronic stress increase inflammation throughout the body, including in gum tissue. Regular exercise, adequate sleep, and stress management techniques all support healthier gums.
Do not wait if you notice any of the following:
The two-week rule is a clear guideline: if your gums have not improved within two weeks of consistent, gentle care, it is time to get a professional opinion.
| Treatment | Used For | What It Does |
|---|---|---|
| Professional Cleaning (Prophylaxis) | Gingivitis, plaque, tartar removal | Removes hardened deposits a toothbrush can’t reach |
| Scaling and Root Planing | Early to moderate periodontitis | Deep cleans below the gumline; smooths root surfaces |
| Antibiotics (topical or oral) | Bacterial infections in gum pockets | Reduces bacterial load in deep pockets |
| Osseous Surgery | Moderate to advanced periodontitis | Reshapes bone to eliminate deep pockets |
| Laser Periodontal Therapy | Moderate periodontitis | Removes infected tissue with minimal discomfort |
| Gum Grafting | Severe gum recession | Replaces lost gum tissue to protect tooth roots |
Preventing gum disease is far simpler and less expensive than treating it.
Brush twice daily with a soft-bristled toothbrush using the correct technique. Floss every day without exception. Use an antimicrobial rinse as part of your routine.
Visit your dentist every six months for professional cleaning and a periodontal evaluation. Early detection is everything.
Eat a balanced diet with adequate vitamins. Stay hydrated. Avoid tobacco in any form. Manage blood sugar if you have diabetes. Tell your dentist about all medications you take.
These habits, done consistently, are the most powerful tools you have against gum disease.

| Action | Removes Plaque | Removes Tartar | Treats Infection | Monitors Bone Loss |
|---|---|---|---|---|
| Brushing | Yes | No | No | No |
| Flossing | Yes | No | No | No |
| Saltwater Rinse | Partially | No | Mildly | No |
| Mouthwash | Partially | No | Mildly | No |
| Professional Cleaning | Yes | Yes | Partially | No |
| Scaling & Root Planing | Yes | Yes | Yes | No |
| Dentist Exam + X-rays | — | — | — | Yes |
Bleeding during brushing almost always means gum inflammation from plaque buildup or gingivitis. Healthy gums do not bleed from routine brushing — this is your mouth’s early warning signal.
No. Healthy gums should never bleed during regular brushing or flossing. Even occasional bleeding indicates some level of inflammation and should be addressed.
In very mild cases of early gingivitis, consistent improved oral hygiene can resolve bleeding within one to two weeks. If it persists beyond that, a dentist visit is necessary.
No — keep flossing. Stopping allows more plaque to accumulate, which worsens the bleeding. The bleeding should decrease within a week of consistent, gentle daily flossing.
In rare cases, gum bleeding can be associated with leukemia due to low platelet counts. If bleeding is accompanied by unusual bruising, fatigue, or other systemic symptoms, see a doctor promptly.
Yes. Chronic stress weakens your immune system, making it harder to fight gum inflammation. It can worsen existing gingivitis and increase your susceptibility to gum disease.
Absolutely. Diabetes impairs the body’s ability to fight infection and slows healing, making gum disease more likely and more severe. Bleeding gums in a diabetic patient require prompt attention.
Vitamin C and Vitamin K are the most directly linked to gum health and bleeding prevention. A diet rich in citrus fruits, leafy greens, and colorful vegetables supports healthier gums.
With consistent oral hygiene improvements, early gingivitis can resolve in one to two weeks. More advanced gum disease requires professional treatment and longer healing time.
See a dentist if bleeding has persisted for more than two weeks, if you notice spontaneous bleeding, gum recession, loose teeth, pus, or persistent bad breath that does not improve with good oral care.
Why are my gums bleeding is a question that deserves a serious answer. Bleeding gums are almost never normal, and they are almost always telling you something important about the health of your mouth and your body.
From early gingivitis caused by plaque buildup to systemic conditions like diabetes and blood disorders, the causes are wide-ranging — but the solution almost always starts with consistent, proper oral care and professional dental evaluation.
Do not ignore the signs in 2026. Catch gum disease early, act on the warning signals your mouth is sending, and protect not just your smile, but your overall health.