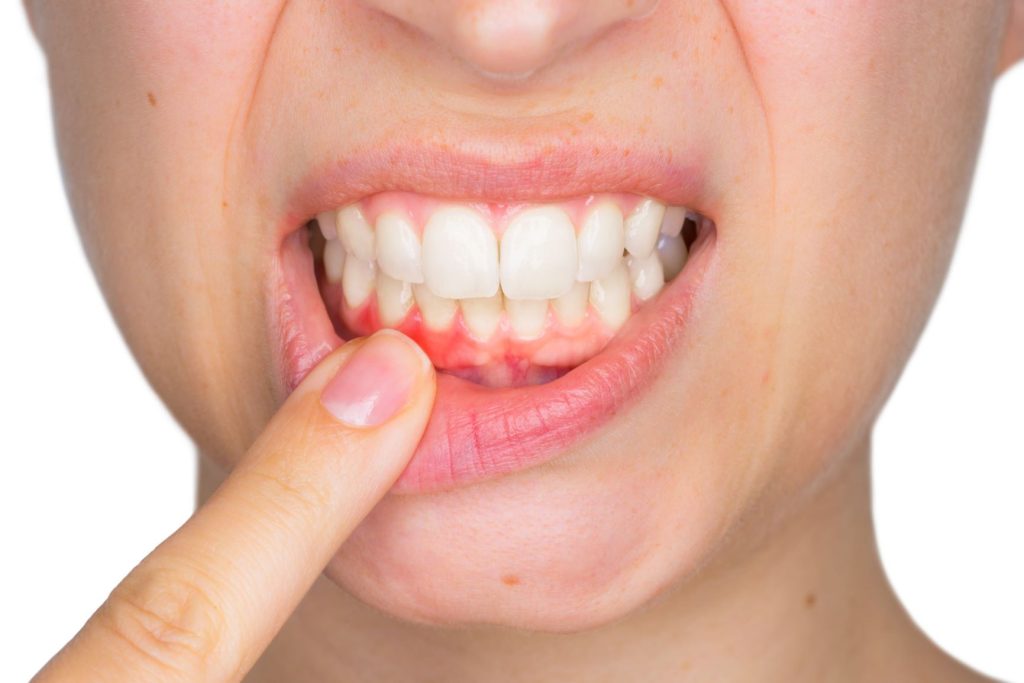
Why do my gums suddenly hurt? It is a question millions of people search every day, and the answer is rarely just one thing.
Sudden gum pain can appear out of nowhere — sharp, throbbing, or dull — and it almost always means your mouth is sending you a message worth paying attention to.
From early gum disease and trapped food debris to hormonal shifts and dental infections, the causes vary widely.

Why do my gums suddenly hurt without warning? In most cases, sudden gum pain means inflammation is already underway.
The most common culprits are gingivitis, trapped food or debris, aggressive brushing, hormonal changes, and dental infections. Some of these are minor and resolve with simple home care. Others need prompt professional treatment before they get worse.
The tricky part is that gum problems often develop silently. Pain that appears “sudden” may have actually been building for weeks beneath the surface before it became noticeable.
Your gums — also called gingiva — are soft tissue that surrounds and supports your teeth and underlying jawbone. They are rich in blood vessels and nerve endings, which is why even minor irritation can cause sharp or throbbing pain.
When bacteria, pressure, hormonal changes, or physical trauma affect the gum tissue, the body responds with inflammation. That inflammation is what produces the swelling, redness, sensitivity, and pain you feel.
Understanding this helps explain why gum pain can come from so many different directions.
Gingivitis is the earliest and most reversible stage of gum disease. It affects roughly 42% of adults aged 30 and older in some form.
Plaque — a sticky film of bacteria — builds up along the gum line when teeth are not cleaned consistently. The immune system responds to that bacterial buildup with inflammation, causing gums to become red, swollen, tender, and prone to bleeding when brushed.
The unsettling truth is that gingivitis can stay largely painless for a long time, then suddenly flare up with noticeable tenderness. That is why many people feel the pain came out of nowhere, even though the underlying buildup has been present for weeks.
If gingivitis is left untreated, it progresses to periodontitis — a more serious stage where bacteria spread below the gum line and begin destroying the bone and connective tissue that hold teeth in place.
At this stage, gums may pull away from teeth, creating pockets where bacteria accumulate further. You may notice persistent bad breath, teeth that feel loose, or deep aching pain around specific teeth.
Unlike gingivitis, periodontitis is not fully reversible. It can be managed and slowed, but the bone loss it causes does not fully regenerate.
| Stage | Reversible? | Common Symptoms | Treatment |
|---|---|---|---|
| Gingivitis | Yes | Red, swollen, bleeding gums | Improved hygiene, professional cleaning |
| Mild Periodontitis | Partially | Gum pockets, some bone loss | Scaling and root planing |
| Moderate Periodontitis | No | Deeper pockets, more bone loss | Deep cleaning, antibiotics |
| Severe Periodontitis | No | Tooth movement, significant bone loss | Surgery may be needed |
Something as small as a popcorn kernel hull, a sesame seed, or a nut skin can wedge itself between the gum and a tooth and cause intense, localized pain very quickly.
The debris creates direct pressure on the gum tissue, and if left there, bacteria begin to accumulate around it. Within hours, you can develop noticeable swelling and tenderness in that one specific spot.
Gentle flossing and a warm water rinse can usually dislodge the debris. If the pain does not resolve within a day or two, see a dentist to rule out a developing abscess.
Aggressive brushing is one of the most overlooked causes of sudden gum soreness. Using a hard-bristle brush or scrubbing back and forth with too much pressure can strip and damage the delicate gum tissue.
Over time, this leads to gum recession — where the gum line pulls back, exposing the root of the tooth. In the short term, it creates raw, sensitive, painful gum tissue that hurts when you brush, eat, or drink.
Switching to a soft-bristle toothbrush and using gentle circular motions rather than a scrubbing action can make a significant difference within a few weeks.

A gum abscess is a pocket of pus caused by a bacterial infection in the gum tissue or in the space between the gum and the tooth. It is one of the most painful dental conditions you can experience.
The pain from an abscess is typically intense, throbbing, and may radiate to the jaw, ear, or neck. You may also notice visible swelling, a bad taste in the mouth, fever, or a small pimple-like bump on the gum.
There are two main types of gum abscesses. A gingival abscess affects only the surface gum tissue, often triggered by foreign debris lodging into the gum. A periodontal abscess forms in the deep space between the tooth and gum and is more common in people who already have gum disease.
A gum abscess cannot be treated at home. While a warm salt water rinse can ease discomfort temporarily, the infection must be drained and treated by a dentist. Do not attempt to pop or press on the abscess.
Canker sores — also called mouth ulcers — are small, painful sores that develop on the soft tissues inside the mouth, including the gums. They appear as round or oval lesions with a white or yellow center and a red border.
The precise cause is not fully understood, but known triggers include minor injuries from brushing, acidic or spicy foods, stress, hormonal changes, and certain nutritional deficiencies.
Canker sores typically heal on their own within 7 to 14 days. They can be very painful — especially when brushing or eating — but they are not contagious and do not indicate gum disease.
Hormonal fluctuations significantly affect gum sensitivity and susceptibility to inflammation. This is especially true for women at several life stages.
During menstruation, rising progesterone levels can cause gum swelling and tenderness. During pregnancy, increased blood flow and hormonal shifts make gums highly prone to inflammation — a condition sometimes called pregnancy gingivitis. During menopause, declining estrogen levels can cause gum tissue to become dry, sensitive, and more vulnerable to pain and bleeding.
If you notice gum pain that follows a predictable hormonal pattern, that is an important detail to share with your dentist.
Pericoronitis is inflammation of the gum tissue surrounding a partially erupted tooth — most often a wisdom tooth. When the tooth only partially breaks through the gum, a flap of tissue can trap food and bacteria underneath, leading to pain, swelling, and sometimes infection.
The pain from pericoronitis can be severe and may radiate to the ear and throat. Swallowing and opening the mouth may become difficult in more serious cases.
Treatment ranges from professional cleaning of the area to antibiotics or, in persistent cases, surgical removal of the wisdom tooth.
Gum soreness after a dental cleaning, filling, crown placement, or extraction is completely normal and expected. The gum tissue is disturbed during these procedures, and some inflammation and tenderness in the following days is a standard healing response.
If the soreness lasts longer than a week, worsens instead of improves, or is accompanied by swelling and fever, call your dentist. Those could be signs of an infection at the treatment site.
Vitamin C is essential for collagen production, and collagen is the building block of healthy gum tissue. A deficiency in vitamin C weakens the gum tissue, making it more fragile, prone to bleeding, and susceptible to pain.
Vitamin B12 and folate deficiencies can also contribute to mouth ulcers and gum inflammation. People following restrictive diets or those with absorption issues are at higher risk.
Adding bell peppers, citrus fruits, strawberries, and leafy greens to your diet supports gum tissue health from the inside out.
Some commercial toothpastes contain ingredients that can irritate sensitive gum tissue. Sodium lauryl sulfate (SLS), an ingredient that creates foam, is a known irritant for many people and can trigger gum soreness and mouth ulcers.
Highly abrasive whitening and tartar-control toothpastes can also erode gum tissue over time when used excessively. If you switched toothpaste recently and gum pain followed, that is worth investigating.
Chronic stress can impact oral health in two ways. First, it weakens the immune response, making gums more vulnerable to bacterial infection. Second, stress commonly triggers bruxism — grinding or clenching the teeth during sleep.
Bruxism creates repeated trauma along the gum line, disrupting the seal between gum and tooth and contributing to gum recession and soreness. A custom nightguard from your dentist can prevent this damage while you work on managing stress.
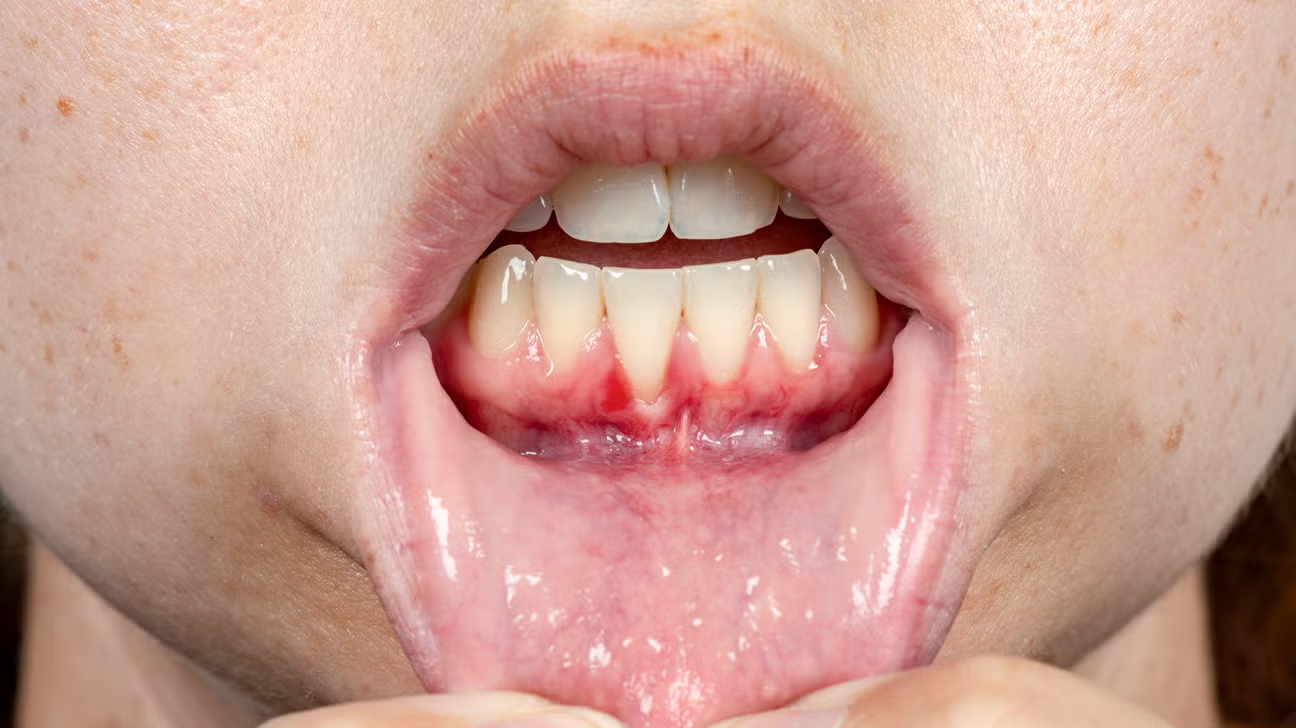
Reading your symptoms carefully can help narrow down the likely cause before you see a dentist.
| Symptom Pattern | Most Likely Cause |
|---|---|
| Pain all along the gum line, bleeding when brushing | Gingivitis or periodontitis |
| Sharp pain in one specific spot | Trapped debris, canker sore, or abscess |
| Throbbing pain with swelling and bad taste | Gum abscess or dental infection |
| Pain near back teeth with difficult swallowing | Pericoronitis from wisdom tooth |
| Pain following a predictable monthly cycle | Hormonal gum changes |
| Soreness after recent dental work | Normal post-procedure inflammation |
| Pain with visible white sore | Canker sore |
| Raw, sore gums with no bleeding | Overbrushing or SLS irritation |
Many cases of mild, sudden gum pain can be managed at home while you wait for a dental appointment or while a minor issue heals on its own.
Salt water is a natural disinfectant that reduces inflammation and promotes healing in gum tissue. Mix half a teaspoon of salt into a glass of warm water, swish gently for 30 seconds, and spit. Repeat two to three times a day.
Applying a cold pack to the outside of your cheek near the sore area for 15 to 20 minutes reduces swelling and numbs local pain. This works especially well for swelling from trauma or abscess pain while you wait to see a dentist.
A diluted hydrogen peroxide rinse can kill oral bacteria and help reduce gum inflammation. Mix equal parts of 3% hydrogen peroxide and water, swish gently for 30 seconds, then spit. Do not swallow.
Clove oil contains eugenol, a natural analgesic with anti-inflammatory properties. Applying a small amount to the painful gum area with a cotton ball can provide temporary numbing relief. Use it sparingly and avoid swallowing.
Pure aloe vera gel applied directly to the affected gum tissue has documented anti-inflammatory and antibacterial effects. Use a product without added sugars or alcohol for best results.
Products containing benzocaine provide short-term topical numbing for gum pain. These are available at most pharmacies and can make eating and brushing more comfortable during a painful flare.
Avoid these common mistakes that can make the problem significantly worse.
Do not ignore pain that lasts more than two days. Do not press or pop a visible abscess — this can spread the infection. Do not brush harder thinking it will clean more. Do not use aspirin directly on the gum — this is an old myth and causes chemical burns to the tissue. Do not skip flossing because it hurts — gentle flossing is often necessary to remove the debris causing the pain.
Some gum pain situations require same-day or emergency dental care. Do not wait and see in the following scenarios.
| Symptom | Action Required |
|---|---|
| Throbbing pain with visible swelling | See dentist same day — possible abscess |
| Fever alongside gum pain | Urgent dental care or emergency room |
| Pain radiating to jaw, ear, or throat | Same-day dental visit |
| Difficulty breathing or swallowing | Emergency room immediately |
| Pus or foul taste in the mouth | Emergency dental appointment |
| Gum pain lasting more than 2 weeks | Schedule dental visit |
| Pain after dental procedure getting worse | Call your dentist right away |
If pain does not improve with home remedies within 48 hours, or if it comes alongside fever, visible swelling, or a foul taste, do not delay. Gum infections can spread to the jaw, neck, and in rare cases, deeper tissues.
Depending on the cause, your dentist has several proven tools to resolve gum pain at its source.
For gingivitis-related pain, a professional cleaning (prophylaxis) removes plaque and tartar buildup that brushing cannot reach. Most patients notice a dramatic improvement in gum soreness within days of a cleaning.
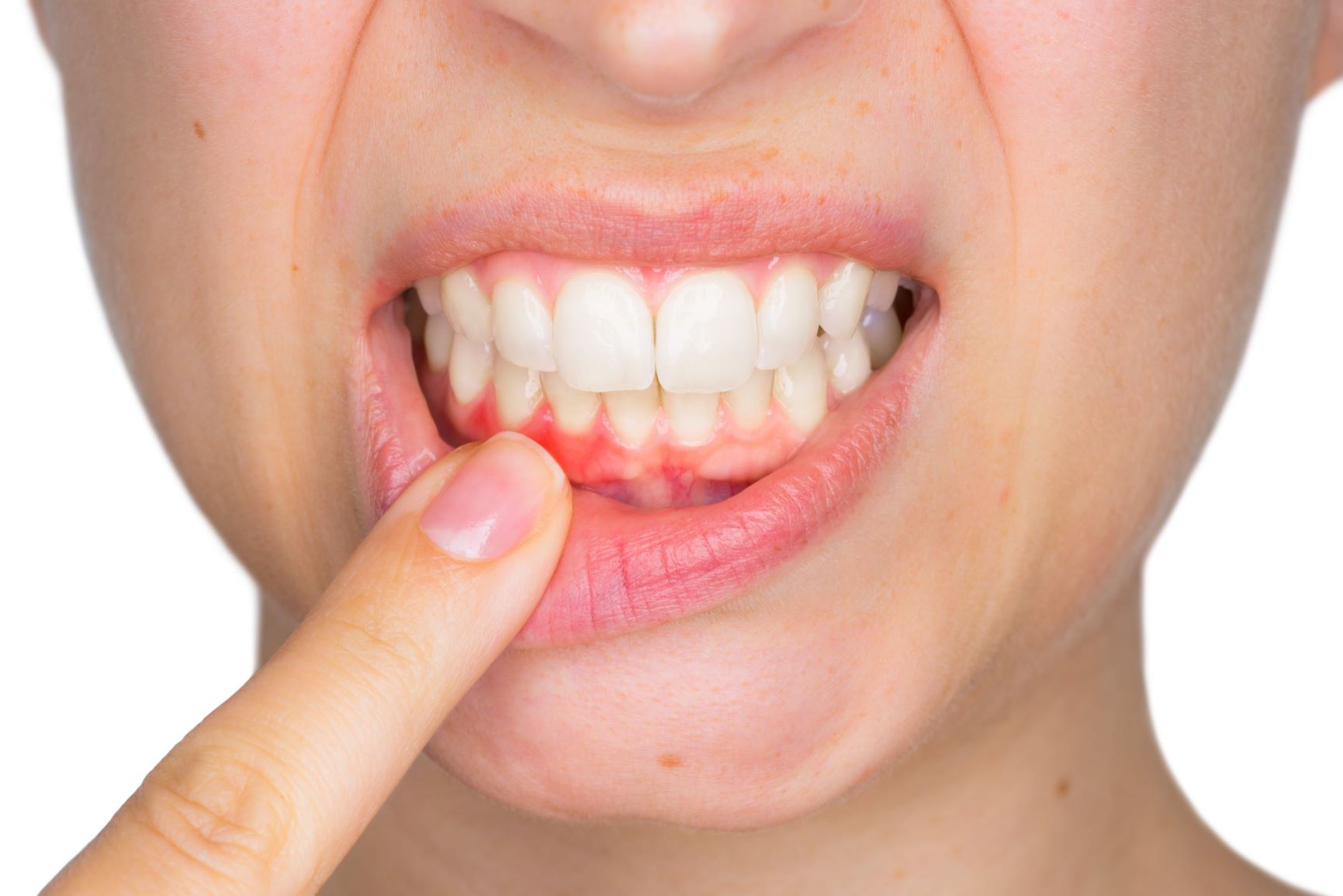
For periodontitis, scaling and root planing is a deep-cleaning procedure that removes bacteria from below the gum line and smooths the root surfaces to prevent bacteria from reattaching. Local anesthetic is used to keep the procedure comfortable.
For gum infections, your dentist may prescribe oral antibiotics or place antibiotic gel directly into infected gum pockets. Antibiotics alone cannot cure gum disease but are an important tool alongside mechanical cleaning.
A gum abscess must be drained by a dentist. The area is numbed, the abscess is opened and drained of pus, and the underlying infection is treated. Root canal treatment may be needed if the infection originated in a tooth.
Recurring pericoronitis usually requires removal of the partially erupted wisdom tooth to permanently resolve the problem and prevent future infections.
Once you have dealt with a painful gum episode, keeping gums healthy long-term comes down to a few consistent habits.
Brush twice daily with a soft-bristle brush using gentle circular strokes. Floss once daily — this is non-negotiable for removing the debris and plaque that brushing misses. Use an antiseptic mouthwash to reduce bacterial load between brushings. Stay hydrated, since dry mouth is a breeding ground for bacteria. Eat a diet rich in vitamin C and avoid excessive sugar. See your dentist every six months for professional cleanings and early detection of any developing problems. If you grind your teeth, ask about a nightguard.
The most important insight is this: gum pain that appears suddenly is almost always the visible symptom of something that has been quietly developing. Catching it early means simpler, faster, and less costly treatment.
Sudden gum pain almost always has a cause, even if it is not immediately obvious. Common triggers include early-stage gingivitis, trapped food debris, a developing abscess, hormonal changes, or a canker sore. A dentist can identify the exact cause quickly.
Yes. Chronic stress weakens the immune system, making gums more vulnerable to bacterial infection. Stress also triggers teeth grinding, which creates repeated physical trauma along the gum line and leads to soreness and recession.
Not always. While gingivitis is the most common cause of sudden gum pain, trapped debris, aggressive brushing, canker sores, hormonal changes, and post-dental procedure soreness can all cause pain without underlying gum disease.
If gum pain does not improve within 48 hours of home care, or if it is accompanied by swelling, fever, bad taste, or throbbing pain, see a dentist right away. Minor irritation typically resolves within one to two days on its own.
Yes. Hormonal fluctuations during menstruation, pregnancy, and menopause are well-documented causes of sudden gum sensitivity and pain. The tissue becomes more reactive to bacteria and physical irritation during these times.
A warm salt water rinse provides the fastest broad relief — it reduces inflammation, kills surface bacteria, and soothes irritated tissue within minutes. For more intense pain, a cold compress applied to the cheek alongside an over-the-counter pain reliever works quickly.
Yes. Vitamin C deficiency weakens gum tissue and collagen, leading to fragile, sore, bleeding gums. Low levels of B12 and folate are also linked to oral ulcers and inflammation. Improving your diet or taking supplements under a doctor’s guidance can help.
Localized gum pain in a single spot is often caused by trapped food debris, a canker sore, an early abscess, or a broken tooth or filling with a sharp edge irritating the gum. Gently flossing and rinsing the area is a good first step. If it persists beyond two days, see your dentist.
Yes — but gently. Stopping brushing makes plaque and bacterial buildup worse, which will worsen the pain. Switch to an extra-soft bristle brush, use light pressure, and rinse with salt water after brushing. Avoid skipping oral hygiene even when the area feels tender.
Minor causes like a canker sore, temporary irritation from hard food, or post-brushing soreness will often resolve on their own within a few days. However, pain caused by gingivitis, periodontitis, abscess, or infection will not resolve without treatment and will worsen over time.
Why do my gums suddenly hurt? The honest answer is that your mouth is rarely silent without reason.
Sudden gum pain — whether it is a sharp twinge in one spot or a dull ache across the whole gum line — is your body’s way of flagging something that needs attention.
In many cases, the fix is straightforward: better brushing technique, removing trapped debris, managing hormonal effects, or a professional cleaning that removes plaque you cannot reach at home.
What matters most is that you do not ignore it or wait too long.
Conditions like gingivitis are completely reversible when caught early. But left untreated, gum disease progresses to bone loss, tooth movement, and much more complex treatment.
If your gum pain has lasted more than two days, involves visible swelling, or feels like throbbing pressure, schedule a dental appointment without delay.
Consistent daily hygiene, regular dental visits, and a nutrient-rich diet are the most powerful tools for keeping your gums pain-free and healthy for the long term.