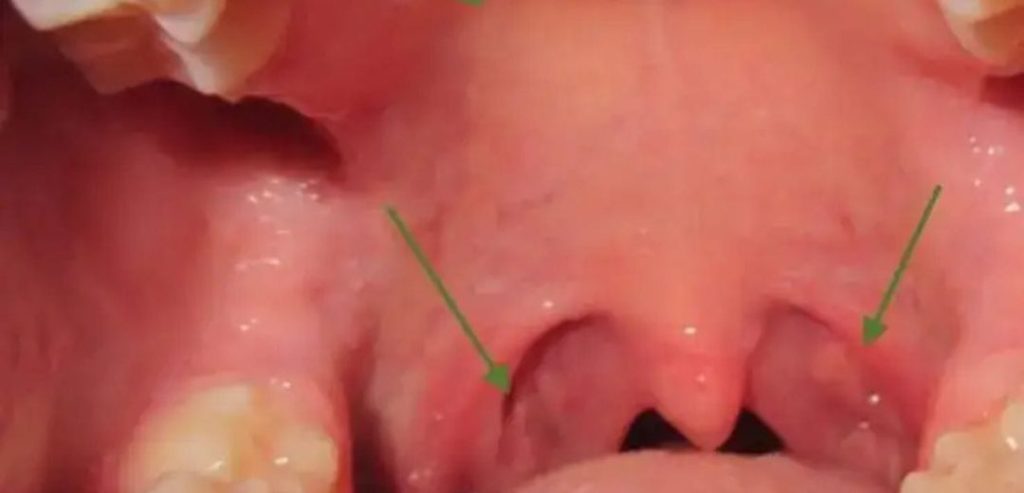
If the roof of your mouth is itchy You are not alone — this is one of the most common oral complaints people search for in 2026.
An itchy palate can signal anything from a seasonal allergy to a fungal infection or even a serious reaction.
Most cases are mild and resolve quickly, but some require medical attention.
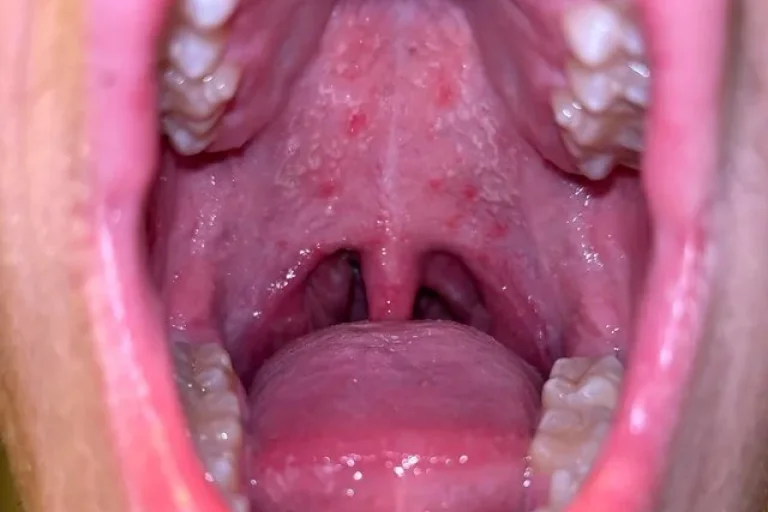
The roof of your mouth is called the palate. It has two parts — the hard palate at the front and the soft palate at the back. Both areas contain sensitive tissues that react quickly to allergens, infections, irritants, and dry conditions.
The palate sits just below the nasal sinuses. This is why nasal congestion, postnasal drip, and sinus pressure can all directly cause itching in this area.
| Cause | Common Trigger | Severity |
|---|---|---|
| Oral Allergy Syndrome (OAS) | Raw fruits, vegetables, nuts | Mild to moderate |
| Seasonal Allergies / Hay Fever | Pollen, grass, ragweed | Mild to moderate |
| Food Allergies | Nuts, shellfish, dairy | Moderate to severe |
| Oral Thrush (Fungal Infection) | Candida overgrowth | Mild to moderate |
| Common Cold or Flu | Viral infection | Mild |
| Postnasal Drip / Sinusitis | Mucus dripping over palate | Mild |
| Cold Sores (Oral Herpes) | HSV-1 virus | Mild to moderate |
| Dry Mouth (Xerostomia) | Low saliva production | Mild |
| Dental Irritation | Ill-fitting dentures, dental work | Mild |
| Anaphylaxis | Severe allergen exposure | Life-threatening |
Oral allergy syndrome (OAS), also called pollen-food allergy syndrome, is the single most frequent cause of an itchy roof of the mouth. It happens when your immune system confuses proteins in certain raw foods with pollen proteins.
Your body thinks the food is an allergen and fires off a reaction — leading to itching, tingling, and swelling inside the mouth. Studies show that 50–75% of adults with birch pollen allergies also develop OAS.
| Pollen Type | Trigger Foods |
|---|---|
| Birch pollen | Apples, pears, cherries, peaches, plums, almonds |
| Grass pollen | Celery, melons, oranges, tomatoes |
| Ragweed pollen | Bananas, cucumbers, melons, zucchini |
| Mugwort pollen | Carrots, celery, spices, garlic |
Symptoms usually appear within minutes of eating a raw trigger food. They typically last less than 20 minutes. Cooking or peeling these foods often eliminates the reaction because heat changes the protein structure.
Hay fever (allergic rhinitis) is another leading cause. When pollen levels are high — especially in spring and fall — your immune system releases histamines that cause widespread inflammation.
This inflammation is not limited to your nose and eyes. It spreads to the soft tissues of your mouth and palate, causing that familiar itchy, tingly feeling. Sneezing, runny nose, and watery eyes usually accompany this type of palate itch.
Food allergies are more serious than OAS. They involve a different immune response and can escalate rapidly. Common culprits include nuts, shellfish, dairy, eggs, and wheat.
Unlike OAS, food allergy symptoms go beyond the mouth. Watch for hives, swelling of the lips or tongue, stomach cramps, or difficulty breathing. These are warning signs of anaphylaxis — a life-threatening emergency that needs an EpiPen and immediate 911 response.
Your sinuses sit directly above the roof of your mouth. When a sinus infection or allergy causes mucus to build up and drip down the back of the throat, it flows right over the palate.
This constant mucus contact irritates the delicate tissue and creates a persistent itchy or tickling sensation. Steam inhalation, nasal saline rinses, and antihistamines help manage this effectively.
Oral thrush is caused by an overgrowth of Candida albicans, a naturally occurring fungus in your mouth. When your immune system is weakened, the fungus multiplies and causes infection.
White or yellowish patches on the tongue, inner cheeks, or roof of the mouth are the hallmark signs. The patches may look like cottage cheese and cause itching, soreness, and difficulty swallowing. Oral thrush requires antifungal medication prescribed by a doctor.
People with weakened immune systems are most vulnerable. This includes those with uncontrolled diabetes, HIV/AIDS, or cancer. People undergoing chemotherapy, using inhaled corticosteroids, or who recently completed a course of antibiotics are also at elevated risk.
Good oral hygiene — brushing, flossing, rinsing your mouth after using inhalers — lowers your risk significantly.
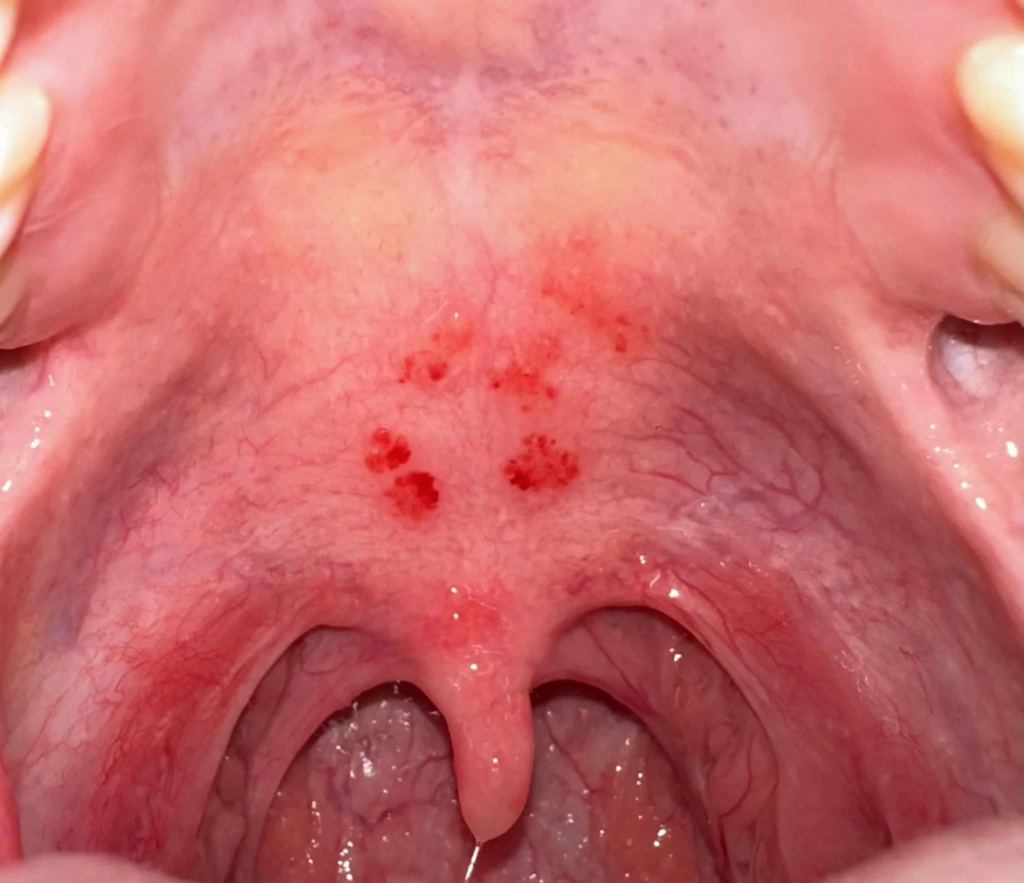
A cold or flu virus can make the roof of your mouth feel itchy or sore, especially in the early stages. The itching usually comes paired with a sore throat, runny nose, and congestion.
Cold-related mouth itching usually resolves on its own within 7–14 days. Rest, hydration, and OTC remedies like acetaminophen are enough for most people. If symptoms persist beyond two weeks, it may be seasonal allergies rather than a cold.
Cold sores are caused by the herpes simplex virus (HSV-1). Before a blister appears, the area often tingles, burns, or itches — sometimes on the roof of the mouth. This is called the prodromal stage.
Cold sores have no cure, but antiviral medications (like acyclovir) can shorten the duration and reduce severity. They typically clear up within two weeks on their own.
Saliva keeps the mouth moist and protects soft tissues. When saliva production drops — due to dehydration, medications like antihistamines, or conditions like Sjögren’s syndrome or diabetes — the palate becomes dry, irritated, and itchy.
Drinking more water, chewing sugar-free gum, and using saliva substitutes or special dry-mouth rinses can offer significant relief.
Poorly fitting dentures, braces, retainers, or recent dental procedures can rub against the delicate tissue on the roof of the mouth. This friction causes localized irritation and itching.
If you notice itching started after a dental visit or new appliance fitting, contact your dentist. The fit may need adjustment to prevent chronic irritation or sores.
Hot pizza, coffee, soup, or any scalding food can burn the palate. As the tissue heals, itching is a normal part of the recovery process — your nerves are regenerating.
The same applies to sharp-textured foods like chips or crackers that scratch the palate. Avoiding further irritants and eating soft, cool foods speeds recovery.
Some toothpastes, mouthwashes, or medications can irritate the palate. Flavoring agents, SLS (sodium lauryl sulfate) in toothpaste, and strong alcohol-based mouthwashes are common culprits.
Cancer medications like Afinitor, Gilotrif, and Nexavar are known to cause mouth itching as a side effect. Always inform your doctor if any medication causes oral discomfort — it may indicate a drug allergy.
Psychological stress can heighten nerve sensitivity throughout the body, including inside the mouth. Some people experience tingling or itching in the palate during periods of high anxiety even without any physical cause.
Managing stress through mindfulness, yoga, or therapy may reduce these sensations. If itching only happens during stressful periods, this connection is worth discussing with a doctor.
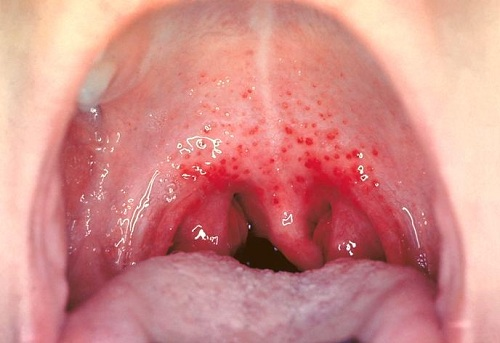
Anaphylaxis is a severe, life-threatening allergic reaction. An itchy roof of the mouth is often one of the earliest signs. What starts as palate itching can quickly escalate to throat swelling, difficulty breathing, a rapid heartbeat, and loss of consciousness.
If you experience any of these symptoms alongside mouth itching, call emergency services immediately. Use an EpiPen if you have one. Do not wait for symptoms to pass on their own.
| Symptom | Urgency |
|---|---|
| Itchy mouth and throat | Early warning — monitor closely |
| Lip or tongue swelling | Seek medical attention now |
| Difficulty breathing or swallowing | Call 911 immediately |
| Rapid heartbeat or dizziness | Call 911 immediately |
| Loss of consciousness | Emergency — use EpiPen |
The additional symptoms you notice alongside palate itching are valuable clues for identifying the cause.
Many people notice the itch intensifies at night. This has several explanations. Allergen exposure throughout the day accumulates. Mouth breathing during sleep dries out the palate tissue.
Postnasal drip worsens when lying flat, meaning more mucus flows over the palate. Low humidity in the bedroom also dries the soft tissues. Using a humidifier, sleeping with the mouth closed, and managing nighttime allergies with a long-acting antihistamine can help.
These remedies are safe, effective for mild cases, and easy to try at home.
| Remedy | How It Helps |
|---|---|
| Warm saltwater rinse | Reduces irritation and keeps the mouth clean |
| Cold water or ice chips | Numbs the tissue and reduces inflammation |
| Honey | Coats and soothes the palate naturally |
| Aloe vera gel | Cooling anti-inflammatory effect |
| Chamomile tea rinse | Calms inflammation and irritation |
| Staying hydrated | Prevents dryness that worsens itching |
| Sugar-free gum | Stimulates saliva production |
Avoid spicy, acidic, or rough-textured foods while the palate is irritated. Stick to soft, cool foods until symptoms improve.
For allergy-related itching, OTC antihistamines are the most effective first-line treatment. Options include:
Cetirizine (Zyrtec) — works within one hour, lasts 24 hours, minimally sedating.
Loratadine (Claritin) — non-drowsy, good for daytime use, once daily.
Diphenhydramine (Benadryl) — fast-acting but causes drowsiness, better for nighttime.
Fexofenadine (Allegra) — non-sedating, 24-hour coverage, good for chronic allergy sufferers.
For OAS triggered by seasonal pollen, taking antihistamines before your allergy season starts (at least one week early) significantly reduces symptoms.
Most cases of an itchy palate resolve on their own or with basic home care. But certain situations require professional evaluation.
See a doctor if the itching lasts more than 7–14 days without improvement. Also seek care if you notice white patches (possible oral thrush), recurring cold sores, swelling, difficulty eating or swallowing, or if symptoms began after starting a new medication.
See a specialist — an allergist or ENT — if the cause is unclear, if over-the-counter treatments are not working, or if you suspect a food allergy that could cause a serious reaction.
If you frequently experience an itchy palate with no clear cause, allergy testing can pinpoint specific triggers.
Skin prick test — small amounts of allergens are applied to the skin via tiny pricks. Reactions are read after 15 minutes.
Blood test (IgE test) — measures allergen-specific antibodies in the blood. Good for people who cannot stop antihistamines for skin testing.
Oral food challenge — done under medical supervision, you consume small amounts of a suspected trigger food to confirm or rule out an allergy.
If palate itching is a recurring problem tied to seasonal allergies or OAS, a long-term plan makes life significantly easier.
Allergy immunotherapy (allergy shots) gradually desensitizes your immune system to specific allergens over time. Sublingual immunotherapy (drops or tablets under the tongue) is an alternative that can be done at home after an initial doctor visit.
Identify and avoid your personal trigger foods and allergens. Keep a symptom journal to track what causes flare-ups. This data is valuable for your allergist when designing a personalized treatment plan.
Preventing the itch is always better than treating it. These daily habits lower your risk.
Cook or peel trigger fruits and vegetables before eating — heat destroys the cross-reactive proteins that cause OAS. Check pollen forecasts and limit outdoor time on high-pollen days. Shower after outdoor activities to remove pollen from skin and hair.
Maintain good oral hygiene — brush twice daily, floss regularly, rinse your mouth after using inhaled corticosteroids. Stay well hydrated and limit alcohol, caffeine, and tobacco which all dry out the mouth. Replace toothpaste or mouthwash if you suspect a sensitivity.
| Condition | Key Symptom | Best First Step |
|---|---|---|
| Oral Allergy Syndrome | Itching after raw food | Avoid raw trigger foods |
| Seasonal Allergies | Itching with sneezing/runny nose | Antihistamines |
| Oral Thrush | White patches, soreness | See a doctor for antifungal |
| Common Cold | Itching with congestion | Rest, fluids, OTC relief |
| Anaphylaxis | Throat tightening, breathing difficulty | Call 911, use EpiPen |
| Dry Mouth | Persistent dryness and itch | Hydration, saliva substitutes |
| Cold Sore | Tingling before blister | Antiviral medication |
| Sinus Infection | Post-nasal drip, facial pressure | Saline rinse, decongestants |
This is most likely oral allergy syndrome. The proteins in raw fruits like apples, peaches, and melons mimic pollen, triggering a mild immune reaction in the mouth.
Yes, absolutely. Hay fever triggers histamine release which inflames the soft tissues of the palate, causing itching, tingling, and discomfort — especially during spring and fall.
It can be a symptom in some cases. However, it is far more commonly linked to allergies or the common cold. Get tested if other COVID symptoms are present.
Rinse with cold water or salt water, suck on ice chips, or apply honey to the area. For allergy-caused itching, an antihistamine like Benadryl works quickly.
It appears as white or yellowish cottage cheese-like patches on the palate, tongue, or inner cheeks. It may cause soreness, itching, and a burning feeling.
Yes. High stress increases nerve sensitivity throughout the body. Some people experience tingling or itching sensations in the mouth purely from anxiety, without any infection or allergen.
Most causes are mild and harmless. However, if itching is accompanied by throat swelling, difficulty breathing, or rapid heartbeat, seek emergency care immediately — these are anaphylaxis warning signs.
Yes. Low saliva production leaves the palate dry and exposed to irritation. Dehydration, certain medications, and conditions like Sjögren’s syndrome all cause dry mouth and palate itching.
Postnasal drip worsens when lying flat, mouth breathing dries out tissues, and bedroom air is often drier. Allergen accumulation from the day also peaks at night.
See a doctor if itching persists beyond two weeks, if white patches appear, if swelling or breathing problems occur, or if the condition does not respond to home treatments and OTC antihistamines.
An itchy roof of the mouth is almost always your body sending a clear signal — whether that is an allergy, an infection, dryness, or a food reaction.
The vast majority of cases are mild and respond well to antihistamines, home remedies, and simple lifestyle changes like staying hydrated and avoiding known triggers.
However, it is important never to dismiss a rapidly worsening itch accompanied by throat tightening or breathing difficulty.
Anaphylaxis can develop fast and is life-threatening.
Always carry an EpiPen if you have a known severe allergy.
The best approach in 2026 is to identify your personal trigger, whether that is birch pollen season, raw apples, poorly fitting dentures, or a new medication.
Once you know the cause, targeted treatment becomes straightforward.
Consult an allergist or ENT specialist if symptoms are recurring or unexplained.
Your palate health is part of your overall wellbeing — and the right diagnosis puts you back in control fast.