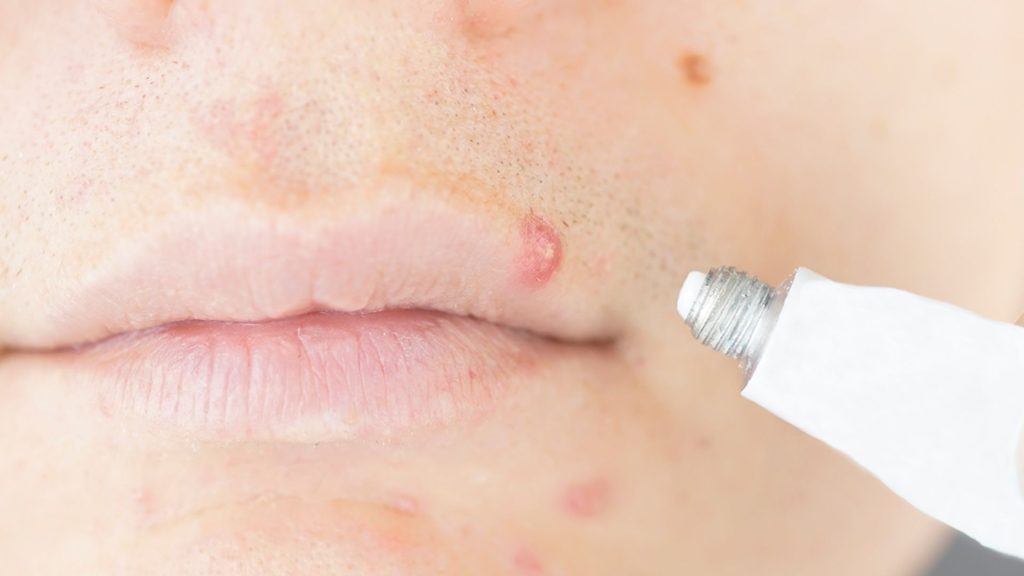
Why do I have a bump on my lip is a question almost everyone asks at some point in their life. Lip bumps are incredibly common and can appear suddenly, without warning, in different shapes, sizes, and colors.
Some are painless. Some sting, itch, or swell. Most are completely harmless and go away on their own within a week or two.
A few, however, signal something that needs medical attention. Understanding what type of bump you have is the most important first step.
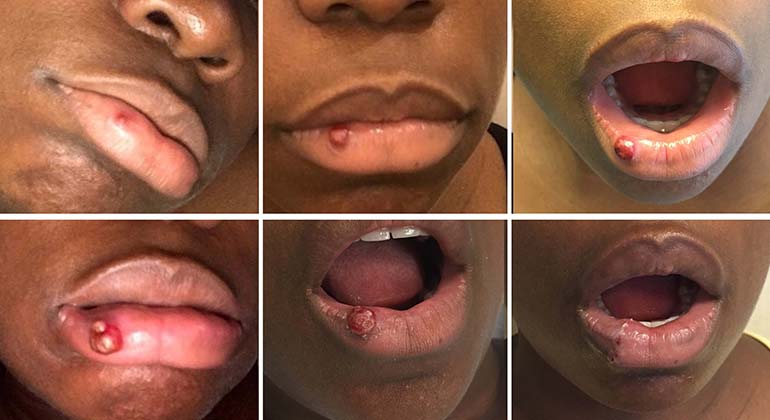
Lip bumps are not all the same. They vary significantly in appearance depending on what is causing them.
They can be tiny white or yellow dots, soft bluish dome-shaped cysts, red raised pimples, clusters of fluid-filled blisters, or flat ulcers with a white center and red border. Some sit on the outer edge of the lip. Others appear inside the mouth on the inner lip lining.
The color, texture, location, and associated symptoms are all clues that help narrow down the cause quickly and accurately.
There are more than a dozen conditions that can cause a bump on your lip. The most common ones account for the vast majority of cases. Here is a detailed breakdown of each.
Cold sores are one of the most frequent causes of a bump on the lip, especially along the outer lip border. They are caused by the herpes simplex virus type 1 (HSV-1).
Most people feel a tingling, burning, or itching sensation at the spot before anything is even visible. Within 24–48 hours, small fluid-filled blisters appear in a cluster. These blisters rupture, crust over, and typically heal within 7–10 days.
HSV-1 is extremely common — studies estimate that up to 67% of adults worldwide carry the virus. Once infected, the virus stays dormant in nerve tissue and can reactivate during periods of stress, illness, sun exposure, or a weakened immune system.
Cold sores are contagious. They spread through direct contact with an active sore, including kissing and sharing utensils or lip products.
Treatment for Cold Sores: Antiviral creams such as acyclovir or penciclovir applied at the first tingle can significantly shorten healing time. Oral antiviral medications like valacyclovir are used for frequent or severe outbreaks. OTC numbing gels (such as Orajel) help manage pain while the sore heals.
Canker sores are small, shallow ulcers that form inside the mouth — on the inner lip, cheeks, tongue, or gum line. They are not caused by a virus and are not contagious.
They appear as round or oval sores with a white or yellowish center and a red border. They can be quite painful, especially when eating acidic or spicy foods.
Common triggers include stress, minor injuries (like biting the inside of your lip), certain foods (coffee, peanuts, tomatoes, citrus), nutritional deficiencies (iron, B12, folate), and hormonal changes. They tend to occur more often in women and typically first appear during teen years or early adulthood.
Most canker sores heal on their own within 1–2 weeks without any treatment.
Treatment for Canker Sores: Warm saltwater rinses (half a teaspoon of salt in a glass of warm water) reduce discomfort and promote healing. OTC oral analgesic gels provide temporary pain relief. For severe or recurring cases, doctors may prescribe corticosteroid rinses or pastes. Avoiding known trigger foods speeds recovery.
Fordyce spots are tiny, painless white or yellowish bumps that appear along the edge of the lips or inside the cheek. They are not infections, not contagious, and not dangerous in any way.
They are simply visible sebaceous (oil) glands — enlarged oil glands that are normally present in skin but are visible on the lip because lip skin is very thin. They affect roughly 80% of adults and become more noticeable during puberty as hormones change.
Fordyce spots measure just 1–3 millimeters in diameter and typically appear in clusters. They do not cause pain, itching, or discomfort of any kind.
Treatment for Fordyce Spots: No treatment is medically necessary. For cosmetic removal, options include topical retinoid creams (which may take 2–6 weeks to show results), carbon dioxide laser treatment, electrodessication, or cryotherapy. Many Fordyce spots naturally fade over time.
A mucocele is a smooth, soft, dome-shaped cyst that forms on the inside of the lower lip. It develops when a salivary gland duct becomes blocked or damaged, causing saliva to pool beneath the surface.
The cyst appears as a painless, bluish or translucent bump. It typically measures between 2 and 10 millimeters. The most common cause is accidental trauma — repeatedly biting the lower lip, sucking the lip, or injury from dental work or a piercing.
Mucoceles often rupture on their own and release a clear fluid. They may refill and return repeatedly. Most resolve without treatment, but persistent or large mucoceles may require professional removal.
Treatment for Mucoceles: Leave mild mucoceles alone — they often rupture and heal on their own. For persistent cysts, a doctor or dentist can perform surgical excision under local anesthesia. Alternative procedures include laser ablation, cryotherapy, and marsupialization (opening and stitching the lesion open). Recurrence after complete removal is uncommon.
Pimples can appear directly on the lip line or just outside it. They form when oil, dead skin cells, or bacteria clog a hair follicle or pore in the skin around the mouth.
A lip pimple looks like a red, raised bump. It may have a white or yellow head at the tip. It is usually tender to the touch. Unlike cold sores, pimples do not tingle before appearing and do not form fluid-filled blisters in clusters.
Triggers include hormonal changes, greasy cosmetics or lip products, poor hygiene, certain foods, and friction from face masks.
Treatment for Lip Pimples: Apply a warm compress for 10–15 minutes several times a day to bring the pimple to a head. OTC topical treatments containing benzoyl peroxide or salicylic acid help clear the area. Do not squeeze or pop a lip pimple — it can push bacteria deeper and cause scarring or infection.
Allergic reactions are a very common cause of bumps and swelling on the lips. Two main types occur.
Allergic contact cheilitis is a form of eczema triggered by contact with an allergen in lip balms, lipsticks, toothpaste, mouthwash, fragrances, or dental materials. It causes redness, inflammation, peeling, and small bumps on and around the lips.
Angioedema is deeper swelling beneath the skin’s surface. It is triggered by food allergies (shellfish, nuts, eggs, certain fruits), medication allergies (especially antibiotics and NSAIDs), or environmental allergens. Angioedema can cause sudden, dramatic swelling of the lips and surrounding area.
Treatment for Allergic Lip Bumps: Identify and eliminate the allergen. Stop using any new lip products, cosmetics, or toothpastes that may be causing the reaction. Oral antihistamines reduce itching and swelling. A doctor may prescribe topical corticosteroids to speed healing. Severe allergic reactions (anaphylaxis) require emergency epinephrine.
Milia are tiny white cysts filled with keratin — a protein found in skin. They look similar to Fordyce spots but are slightly more raised and firm to the touch.
They form when dead skin cells become trapped beneath the skin’s surface instead of shedding normally. They commonly appear around the eye area but can also appear on and around the lips.
Milia are completely harmless and not contagious. They often resolve on their own within a few weeks to months.
Treatment for Milia: Most milia resolve without treatment. A dermatologist can extract them safely with a sterile needle if desired. Do not attempt to squeeze or pop them at home. Gentle exfoliation and non-comedogenic lip products can help prevent recurrence.
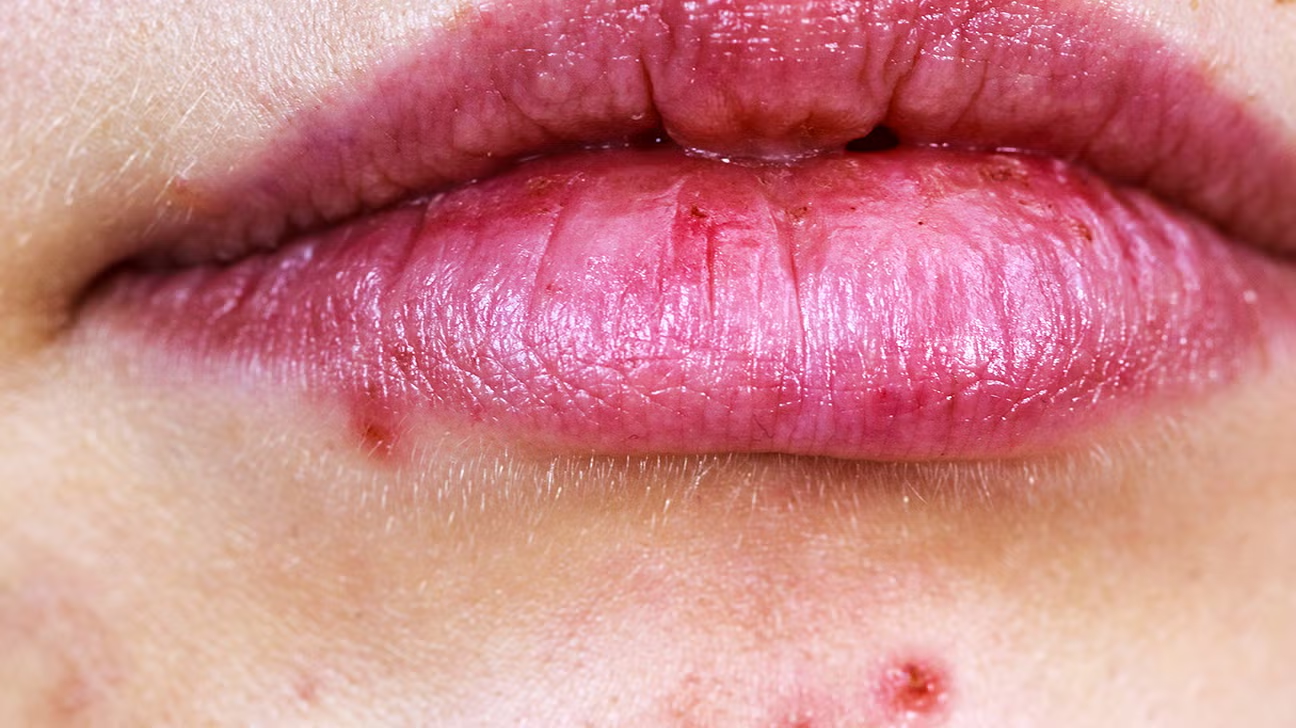
Oral thrush is a fungal infection caused by an overgrowth of Candida yeast in the mouth. While it primarily affects the inner cheeks, tongue, and palate, it can occasionally extend to the lips, creating white, swollen patches.
Risk factors include antibiotic use (which disrupts normal mouth bacteria), a weakened immune system, uncontrolled diabetes, wearing dentures, and very young or elderly age.
Treatment for Oral Thrush: Antifungal medications are highly effective. Doctors typically prescribe nystatin oral suspension (rinse and swallow) or fluconazole tablets for more persistent cases. Good oral hygiene and treating underlying risk factors prevent recurrence.
Hand, foot, and mouth disease (HFMD) is a viral infection that primarily affects young children, though adults can get it too. It causes painful sores and bumps on the lips, inside the mouth, and sometimes on the hands and feet.
HFMD is contagious and spreads through direct contact. Most people recover fully without medical treatment within 7–10 days.
Treatment for HFMD: Management is supportive — rest, fluids, and OTC pain relievers (ibuprofen or acetaminophen) to manage fever and discomfort. Cold foods like ice chips or yogurt can soothe painful mouth sores.
Syphilis is a bacterial sexually transmitted infection (STI) that can cause a painless, firm sore (chancre) on the lips or inside the mouth in its primary stage. This sore is often mistaken for a cold sore or minor injury.
If untreated, syphilis progresses through later stages that cause serious systemic complications. Doctors treat it effectively with antibiotics, particularly penicillin.
If you have a painless lip sore and any risk of STI exposure, see a doctor promptly for testing.
Leukoplakia appears as thick, white or grayish patches on the lips, inside the cheeks, or gums. It is most often associated with tobacco use, excessive alcohol consumption, sun exposure, or HPV infection.
It is not immediately dangerous on its own, but some cases of leukoplakia can become cancerous over time. Any white patch that does not rub off and persists for more than two weeks should be evaluated by a doctor or dentist.
Treatment for Leukoplakia: Eliminating tobacco and alcohol is the most important step. A doctor may perform a biopsy to rule out malignancy. Laser removal or surgical excision may be recommended in certain cases.
Lip cancer is rare but real. It most often appears on the lower lip as a persistent sore, lump, or thickening that does not heal. Other warning signs include a spot that bleeds easily, changes in color, numbness, or a sore that keeps growing.
Risk factors include chronic sun exposure, tobacco use, heavy alcohol consumption, fair skin, and HPV infection. Lip cancer is treatable — especially when caught early. Early detection dramatically improves outcomes.
See a doctor immediately if any bump on your lip has not healed within 2–3 weeks, grows rapidly, bleeds, causes numbness, or does not fit the appearance of common harmless conditions.
| Type | Location | Appearance | Pain Level | Contagious | Heals On Its Own |
|---|---|---|---|---|---|
| Cold Sore | Outer lip border | Fluid-filled blister clusters | Moderate | Yes (HSV) | Yes, 7–10 days |
| Canker Sore | Inner lip, cheeks, tongue | White/yellow ulcer, red border | Moderate–High | No | Yes, 1–2 weeks |
| Fordyce Spots | Lip edge, inner cheek | Tiny white/yellow dots | None | No | Sometimes (fade slowly) |
| Mucocele | Inner lower lip | Soft, bluish dome-shaped cyst | None–Mild | No | Often yes |
| Lip Pimple | Outer lip line | Red raised bump, possible white head | Mild | No | Yes, within days |
| Milia | Around lip border | Tiny firm white cysts | None | No | Yes, weeks–months |
| Allergic Reaction | Outer/inner lip | Swelling, redness, bumps | Mild–Moderate | No | Yes, if allergen removed |
| Oral Thrush | Inner lip, mouth | White swollen patches | Mild | Rare | Needs antifungal |
| Leukoplakia | Lower lip, inner cheek | Thick white/gray patch | None | No | Needs treatment |
| Lip Cancer | Usually lower lip | Persistent lump or non-healing sore | Varies | No | No — see a doctor |
Several home treatments are supported by evidence and widely recommended by healthcare professionals.
When home remedies are not enough, or when the bump requires professional diagnosis, several effective medical treatments are available.
| Treatment | Best For | How It Works |
|---|---|---|
| Antiviral creams (acyclovir, penciclovir) | Cold sores | Suppresses HSV replication |
| Oral antivirals (valacyclovir) | Frequent cold sores | Systemic antiviral control |
| Corticosteroid rinses/pastes | Severe canker sores | Reduces inflammation |
| Oral antihistamines | Allergic reactions | Blocks histamine response |
| Topical corticosteroids | Allergic contact cheilitis | Reduces allergic inflammation |
| Antifungal medications (nystatin, fluconazole) | Oral thrush | Eliminates Candida overgrowth |
| Surgical excision | Mucoceles, cysts | Removes blocked gland completely |
| Laser ablation | Mucoceles, Fordyce spots | Precise, minimally invasive removal |
| Cryotherapy | Mucoceles, Fordyce spots, milia | Freezes and destroys abnormal tissue |
| Topical retinoids | Fordyce spots (cosmetic) | Reduces appearance of sebaceous glands |
| Antibiotics | Bacterial infections, syphilis | Eliminates bacterial infection |
| Biopsy | Suspicious or non-healing lesions | Rules out malignancy |
A doctor or dentist diagnoses a lip bump primarily through visual examination and medical history. In most cases, the appearance and location of the bump make the cause immediately obvious.
For less clear-cut cases, additional diagnostic approaches include allergy patch testing (to identify contact allergen triggers), swab cultures (to test for HSV or bacterial infection), blood tests (for syphilis or STI screening), and biopsy or exfoliative cytology (to rule out oral cancer or leukoplakia in persistent or unusual lesions).
Do not delay seeing a professional if the bump has unusual features or fails to improve within 2–3 weeks.
Most lip bumps are harmless and resolve on their own. However, certain signs indicate you should seek professional evaluation promptly.
See a doctor if the bump has not healed after 2–3 weeks despite home care, if it is growing in size, bleeding, or changing in color, if it is accompanied by difficulty swallowing, numbness, or spreading swelling, if you have a painful sore and any concern about an STI, if you experience recurring cold sores more than 6 times per year, or if the bump is accompanied by systemic symptoms like fever, fatigue, or swollen lymph nodes.
Never ignore a persistent lump on the lower lip — this is the most common location for lip cancer, and early evaluation is always the safest approach.
Preventing lip bumps involves managing known triggers and maintaining good oral hygiene habits.
Use a lip balm with SPF 30 or higher daily to protect against UV exposure, which triggers cold sore outbreaks and increases skin cancer risk. Avoid sharing lip products, utensils, or drinks with anyone who has an active cold sore. Practice good oral hygiene — brush twice daily, floss once daily, and replace your toothbrush every 3 months or after any oral infection. Manage stress through regular exercise, adequate sleep, and relaxation techniques, as stress is a primary trigger for both cold sores and canker sores.
Avoid biting or sucking your lips — this is the leading cause of mucoceles. If you notice a new reaction to any lip balm, lipstick, or toothpaste, switch to fragrance-free, dye-free alternatives designed for sensitive skin. Eat a balanced diet rich in iron, B12, folate, and zinc to reduce canker sore frequency caused by nutritional deficiencies.
If you have recently had lip filler injections, small bumps or lumps appearing in the days immediately after the procedure are usually normal and expected.
Post-filler bumps typically result from mild swelling, bruising, or uneven distribution of the filler product. Most resolve on their own within 2–4 weeks as swelling subsides and the filler settles.
If a lump is painful, firm, persists beyond one month, or is accompanied by redness or warmth, contact your aesthetic provider promptly. In rare cases, post-filler bumps can indicate infection, vascular occlusion, or a granuloma that needs professional management.

Lip bumps in children are very common and usually not serious. Hand, foot, and mouth disease is a frequent culprit, particularly in children under 5. Cold sores can also occur in young children if they have been exposed to HSV-1.
Mucoceles from lip biting are common in school-age children. Fordyce spots may begin appearing during puberty. If your child has a persistent or painful lip bump that does not resolve within 2 weeks, see a pediatrician or pediatric dentist for evaluation.
A bump lasting more than 2–3 weeks could be a persistent mucocele, leukoplakia, or in rare cases, lip cancer. See a doctor or dentist promptly for evaluation and diagnosis.
Cold sores appear on the outer lip border as clusters of fluid-filled blisters preceded by tingling. Pimples appear as single red raised bumps on the lip line without the tingling warning sign.
Yes. Stress is a well-known trigger for both cold sores (by reactivating the dormant HSV-1 virus) and canker sores (aphthous ulcers) that appear on the inner lip or mouth.
Most white bumps — such as Fordyce spots, milia, or canker sores — are completely harmless. However, white patches that persist, grow, or do not rub off may indicate leukoplakia and should be evaluated by a doctor.
For canker sores, use warm saltwater rinses and OTC gel. For cold sores, apply antiviral cream at the first tingle. For pimples, use warm compresses. Most bumps resolve within 1–2 weeks with proper care.
Yes. Some lip balms contain fragrances, dyes, or preservatives that cause allergic contact cheilitis — a reaction that produces redness, irritation, and small bumps. Switch to fragrance-free, hypoallergenic products to resolve the issue.
Not always, but mucoceles are the most common cause of bumps on the inner lower lip. Other possibilities include canker sores, minor salivary gland infections, or in rare cases, benign tumors.
No. Popping, squeezing, or draining any lip bump at home — whether a pimple, mucocele, or blister — can introduce bacteria, delay healing, worsen the condition, and cause scarring.
Cold sores last 7–10 days. Canker sores heal in 1–2 weeks. Mucoceles vary from days to months. Fordyce spots and milia may persist longer but are harmless. Bumps lasting more than 3 weeks need professional evaluation.
In rare cases, yes. Lip cancer usually appears as a persistent sore or lump on the lower lip that does not heal, may bleed, and changes in size or color. See a doctor immediately if a bump shows any of these features.
Why do I have a bump on my lip is a question with many possible answers — and most of them are reassuring. The vast majority of lip bumps are caused by everyday conditions like cold sores, canker sores, Fordyce spots, mucoceles, or pimples.
Most resolve on their own within one to two weeks with simple home care, good oral hygiene, and the right over-the-counter treatment. The key is identifying which type of bump you have so you apply the right remedy.
Warm saltwater rinses, antiviral creams, and avoiding known irritants handle most cases effectively. However, any bump that persists beyond three weeks, grows, bleeds, causes numbness, or looks unusual deserves professional evaluation.
Caught early, even the rare serious causes — like lip cancer or syphilis — are highly treatable. When in doubt, see a doctor. Your lips are worth it.