Why are my feet peeling? This is one of the most common foot health questions people ask, and the answer is not always simple.
Peeling feet can be caused by a fungal infection, dry skin, a skin condition like eczema or psoriasis, or even something as ordinary as sunburn.
While the peeling itself is usually not dangerous, it can be uncomfortable, embarrassing, and sometimes a sign of something that needs treatment.
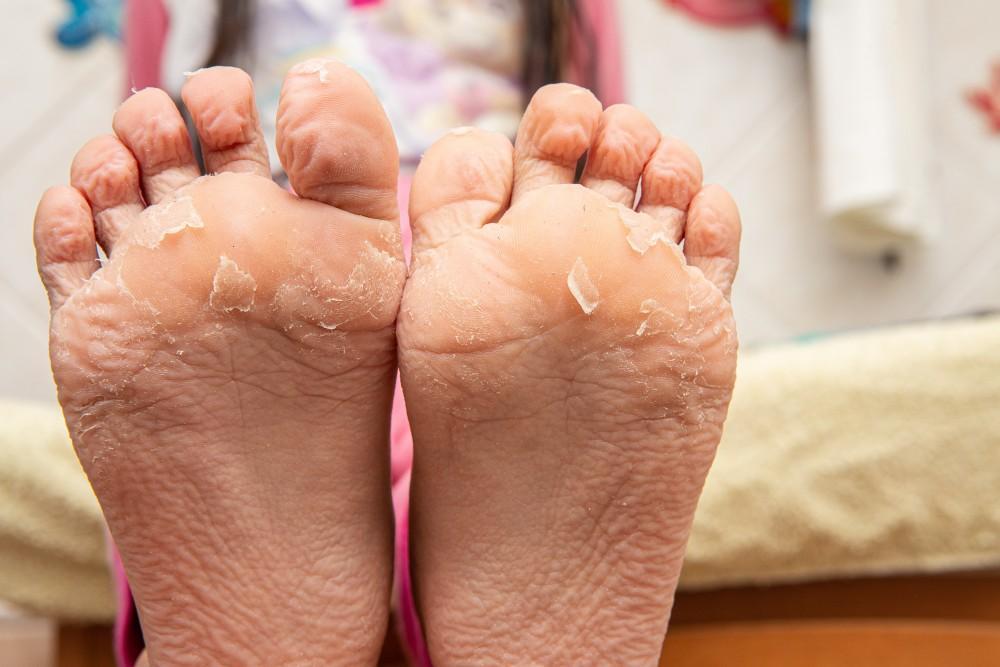
The outer layer of skin naturally sheds dead cells every few weeks. On most parts of the body, this process goes unnoticed. On feet, however, the combination of pressure, friction, heat, and sweat makes skin turnover more visible — and sometimes more dramatic.
When peeling is mild, it is usually just dry skin. When it is heavy, recurring, or comes with itching, burning, or cracking, it is worth investigating the cause more carefully.
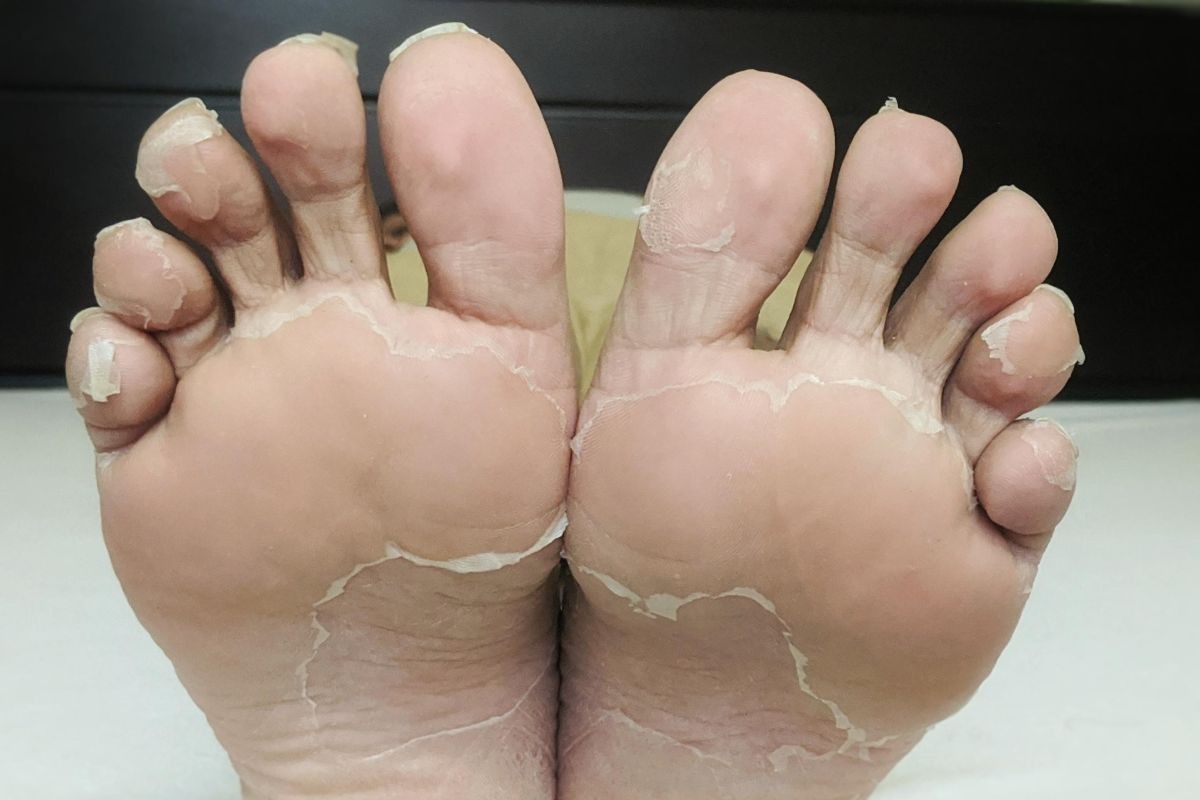
Athlete’s foot is the most common cause of peeling feet. It is a fungal infection caused by dermatophytes — fungi that thrive in warm, damp environments like locker rooms, pool decks, and the insides of tight shoes.
The infection usually starts between the toes and spreads to the soles and sides of the feet. Symptoms include itching, burning, redness, scaling, and skin peeling in flakes or sheets.
You do not need to be an athlete to get it. Anyone who walks barefoot in communal areas or wears tight, non-breathable shoes is at risk.
Key symptoms:
Treatment:
Dry skin is one of the simplest and most overlooked reasons why feet peel. When the skin lacks enough moisture, it becomes rough, tight, and flaky. On the feet, where natural oils are fewer and pressure is constant, dryness gets worse fast.
Common triggers include hot showers, low humidity, prolonged sun exposure, dehydration, aging, smoking, and wearing open-backed sandals that allow moisture to evaporate from the heel.
Key symptoms:
Treatment:
Eczema is an inflammatory skin condition that can affect the feet, causing dry, itchy, cracked, and peeling skin. Three types can appear on the feet: atopic dermatitis, contact dermatitis, and dyshidrotic eczema.
Contact dermatitis is triggered by allergens or irritants — often the materials in shoes, socks, or laundry detergent. Dyshidrotic eczema causes intensely itchy blisters that dry out and peel over 2–3 weeks.
Key symptoms:
Treatment:
Psoriasis is an autoimmune condition that speeds up the skin cell turnover cycle, causing thick, scaly plaques to form. When it affects the feet and hands, it is called palmoplantar psoriasis.
The dead skin builds up faster than the body can shed it, resulting in thick, silvery-white scales that flake off aggressively. In severe cases, the entire sole of the foot can be affected, and painful cracks can form that bleed when walking.
Key symptoms:
Treatment:
Hyperhidrosis is a condition where the body produces sweat far beyond what is needed for temperature regulation. When feet sweat excessively, the constant moisture softens and breaks down the outer skin layer, leading to irritation, redness, maceration, and peeling.
The damp environment inside shoes also creates perfect conditions for fungal infections like athlete’s foot, making the problem compound quickly.
Key symptoms:
Treatment:
This is a surprisingly common and frequently forgotten cause of foot peeling, especially in summer. Many people apply sunscreen to their legs and arms but skip the tops of their feet when wearing sandals or going barefoot on the beach.
The result is sunburned skin that turns red and tender, then peels a few days later — sometimes in large sheets. The peeling is the body shedding damaged skin cells.
Key symptoms:
Treatment:
Some people develop allergic or irritant reactions to the materials in their footwear — rubber, leather dyes, adhesives, or synthetic fabrics in socks. The rash often mirrors the shape of the shoe’s contact points (toe box, heel counter, strap lines).
Over time, the inflamed skin breaks down and peels, especially in areas of friction and heat.
Key symptoms:
Treatment:
Trench foot develops when feet are exposed to wet, cold, or damp conditions for extended periods — soggy socks, wet boots, or standing in water for hours. The constant moisture breaks down the skin barrier, and when drying begins, the damaged skin peels off.
Key symptoms:
Treatment:
This is a rare, inherited genetic condition that causes painless, spontaneous peeling of the outer skin layer, particularly on the hands and feet. It is not caused by any infection or environmental factor.
The peeling is lifelong but does not usually cause other health problems. There is no cure, but moisturizers can help manage the appearance and comfort of the skin.
People with diabetes are at higher risk of dry, cracked, and peeling feet because the condition can reduce circulation and nerve function in the extremities. Poor blood flow means the skin receives less nourishment, and poor nerve sensation means small injuries or infections may go unnoticed.
For anyone with diabetes, peeling feet should be taken seriously and evaluated by a podiatrist, as small wounds can escalate into serious complications.
Warning signs in diabetics:
| Cause | Main Location | Key Symptom | First Treatment |
|---|---|---|---|
| Athlete’s Foot | Between toes, sole | Itch, odor, scaling | OTC antifungal cream |
| Dry Skin | Heels, sole | Flaky, tight skin | Daily moisturizer |
| Eczema | Anywhere on foot | Intense itch, blisters | Fragrance-free moisturizer |
| Psoriasis | Sole, heel | Thick silvery plaques | Prescription topical cream |
| Hyperhidrosis | Full sole | Wet skin, maceration | Antiperspirant, sock change |
| Sunburn | Top of foot | Red, tender, peeling sheets | Aloe vera, cool compress |
| Contact Dermatitis | Shoe-contact areas | Rash matching shoe outline | Switch footwear |
| Trench Foot | Full foot | Waterlogged, numb skin | Dry and warm the foot |
| Diabetes-Related | Heels, sole | Slow-healing cracks | Podiatrist evaluation |
Moisturizing is the single most effective daily treatment for most types of foot peeling. Use a thick, fragrance-free cream with active ingredients like urea (10–25%), lactic acid, glycerin, or shea butter. Apply immediately after bathing while skin is still slightly damp to lock in moisture.
Wear cotton socks over the moisturizer overnight for deeper penetration. This simple overnight routine can visibly improve peeling within a week.
If athlete’s foot or fungal infection is the cause, moisturizing alone will not fix it. Use a proven OTC antifungal like clotrimazole, terbinafine, or miconazole. Apply it consistently for the full recommended duration — usually 2 to 4 weeks — even after symptoms seem to clear.
Stopping early is the most common reason athlete’s foot comes back.
Once or twice a week, use a pumice stone or foot file on softened skin (after soaking feet for 10 minutes) to remove dead, peeling skin. This does not cure the underlying cause but makes feet more comfortable and helps creams absorb better.
Do not aggressively scrub broken, cracked, or infected skin.
A vinegar foot soak (1 part white vinegar to 2 parts cool water, 10–15 minutes) can chemically loosen dead skin and has mild antifungal and antimicrobial properties. It is a useful home remedy for mild cases of dry skin and early athlete’s foot.
Avoid soaking if skin is cracked or has open sores, as the acidity can sting and delay healing.
Coconut oil is rich in moisturizing fatty acids and has mild antifungal properties. Apply it generously to clean, dry feet before bed. Layer a pair of socks on top to lock in moisture overnight. It works best as a complement to a proper moisturizing cream rather than a standalone treatment.
Preventing peeling feet is much easier than treating them. Small daily habits make a significant difference.
Keep feet clean and dry every day, especially between toes. Moisture trapped between toes is the number one trigger for fungal infections.
Wear breathable, well-fitting footwear. Tight, synthetic shoes trap heat and sweat, creating the perfect environment for skin breakdown and fungal growth.
Change socks daily. If you sweat heavily, change socks mid-day and choose moisture-wicking materials like merino wool or technical synthetics designed for foot use.
Apply sunscreen to the tops of your feet before outdoor activities. Many people forget this simple step and end up with a painful sunburn that peels for days.
Moisturize every day, especially after showering. Make it a habit, like brushing your teeth.
Wear flip-flops or shower shoes in communal areas like gyms, pool decks, and locker rooms to avoid picking up fungal infections from contaminated surfaces.
Stay hydrated. Drinking enough water keeps skin supple from the inside. Dehydration is a contributing factor to dry, peeling skin throughout the body.

Most cases of peeling feet clear up with home care within 1–2 weeks. However, you should see a podiatrist or doctor if:
A podiatrist can perform a skin culture, patch test, or other diagnostic tests to identify the exact cause and prescribe targeted treatment.
Most cases have a cause — often dry skin, mild athlete’s foot, or a reaction to footwear or products. If you cannot identify a trigger and peeling is persistent, a podiatrist can help find the answer.
It can be. Athlete’s foot is the most common fungal cause and is often accompanied by itching, burning, and odor between the toes or along the sole.
Yes. Diabetes can reduce circulation and nerve function, leading to dry, cracking, and peeling skin on the feet. Diabetics should see a podiatrist for any foot skin changes.
The bottom of the feet can peel due to dry skin, athlete’s foot (moccasin type), psoriasis, or eczema. A thick, scaly sole that peels in sheets often points to fungal infection or psoriasis.
Peeling between toes is most commonly caused by athlete’s foot, excessive moisture, or contact dermatitis from shoe materials. Keep the area clean, dry, and treat with antifungal cream if itching is present.
Moisturize daily with a urea-based or glycerin-rich cream, wear breathable socks and shoes, keep feet dry, and treat any underlying infection with appropriate antifungal medication.
Yes. Deficiencies in vitamins B3 (niacin), B7 (biotin), and vitamin A can contribute to dry, peeling skin. A balanced diet or supplementation under medical guidance can help.
No. Pulling or peeling skin off can tear healthy skin underneath, create open wounds, and increase the risk of infection. Use gentle exfoliation with a pumice stone after soaking instead.
It helps as a supporting measure. Hydration contributes to overall skin health, but topical moisturizers are more directly effective at treating dry, peeling foot skin.
Mild dry skin can improve in days with consistent moisturizing. Athlete’s foot typically clears in 2–4 weeks with antifungal treatment. Psoriasis and eczema require ongoing management and may take longer.
Why are my feet peeling? As this guide shows, the answer depends on a combination of factors — from fungal infections and dry skin to autoimmune conditions and sun damage.
The good news is that most causes of peeling feet are treatable, and many can be managed effectively at home with the right moisturizer, antifungal cream, or lifestyle adjustment.
The key is identifying the correct cause and addressing it consistently. If home treatment does not help within 2–4 weeks, or if you have underlying health conditions like diabetes, do not hesitate to consult a podiatrist. Healthy, comfortable feet are entirely achievable with the right approach in 2026.