
Why does my tooth filling hurt after months? This is one of the most common questions patients ask their dentist — and it is completely valid. Dental fillings are meant to fix pain, not cause it. Yet many people experience lingering discomfort, sensitivity, or throbbing aches long after the procedure is done.
While minor sensitivity in the first few days is normal, pain that persists or returns after months is your body sending an important signal. Understanding the causes, warning signs, and treatment options can help you protect your tooth and avoid more serious complications in 2026.
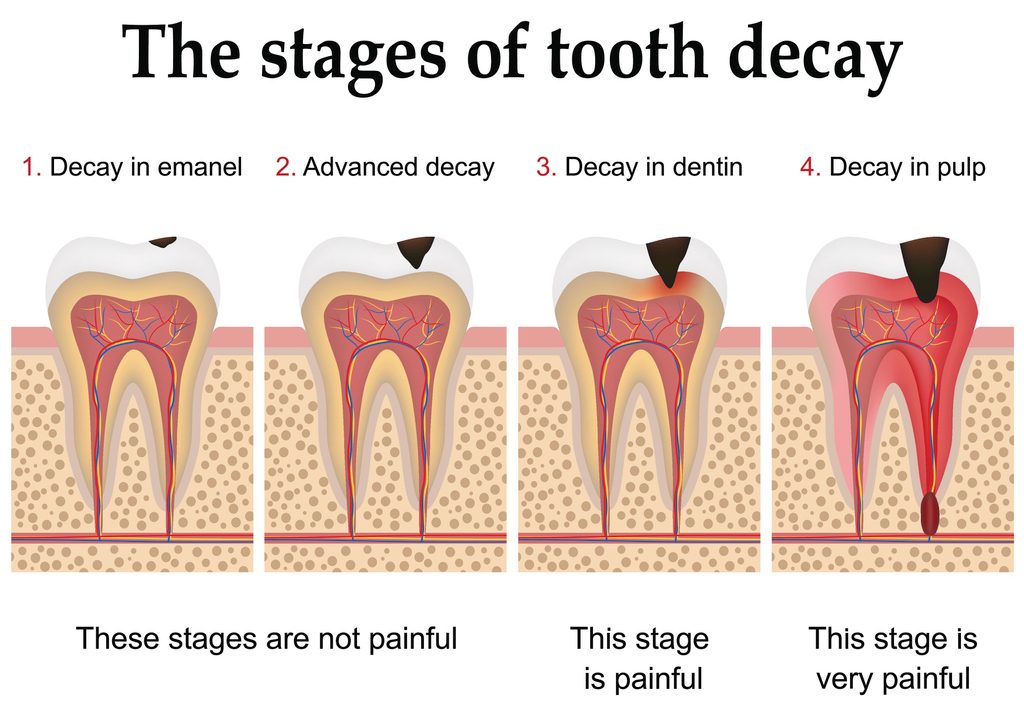
A dental filling is a restorative procedure where your dentist removes decayed tooth material and fills the cavity with a durable material. Common filling materials include composite resin, amalgam (silver), gold, and ceramic.
After the procedure, mild sensitivity for a few days is completely normal. The tooth has been drilled, cleaned, and filled, and the surrounding tissue needs time to recover.
Most post-filling discomfort resolves within one to two weeks. If sensitivity is still present at six weeks, or if pain appears or returns months later, something more is likely going on.
No. Pain that persists or reappears months after a filling is not a normal part of the healing process.
Short-term sensitivity to hot, cold, or pressure is expected. But a tooth that starts hurting weeks or months after the initial discomfort had settled down is giving you a warning sign.
Persistent or returning pain after months almost always indicates an underlying problem that requires professional evaluation. The sooner you act, the simpler and less expensive the fix usually is.
A high filling is one of the most common and easily corrected causes of prolonged pain. If the filling was placed even slightly above your natural bite line, it creates uneven pressure every time your teeth meet.
Over time, this constant extra pressure causes soreness in the filled tooth and can even lead to jaw discomfort. You may notice sharp pain when biting down or chewing.
The good news is this is one of the quickest fixes in dentistry. Your dentist can reshape the filling in a single short appointment, often with immediate relief.
Pulpitis is inflammation of the dental pulp, the soft inner tissue of the tooth containing nerves and blood vessels. It develops when a filling is deep and close to the pulp, or when drilling causes significant thermal or mechanical stress on the nerve.
There are two types that matter here. Reversible pulpitis is mild inflammation that the tooth can heal on its own. The pain is brief, triggered by stimuli like cold, and fades quickly.
Irreversible pulpitis is more serious. The pain is spontaneous, lingering, often worse at night, and may radiate to the jaw or ear. This type will not resolve on its own and typically requires root canal treatment.
Fillings can crack, chip, or lose their seal over time — especially with age, teeth grinding, or chewing hard foods. A cracked or leaking filling creates a gap where bacteria and food particles can enter.
Once bacteria penetrate beneath the filling, they begin attacking the tooth structure again. This leads to secondary decay, nerve irritation, and persistent pain.
You might notice a change in sensation when biting, a new sharp edge you can feel with your tongue, or pain that suddenly reappears after months of no discomfort.
Even a perfectly placed filling is only as protective as the oral hygiene around it. If plaque and bacteria accumulate at the margins where the tooth and filling meet, new decay can form.
Secondary decay — sometimes called recurrent decay — eats into the tooth structure around the filling. As it progresses toward the inner layers of the tooth, it causes pain and sensitivity.
This is why regular dental checkups and X-rays matter. Decay around a filling can often be caught early before it causes significant damage or requires a root canal.
Some cavities are very deep, sitting close to the dental pulp where the nerve lives. When a dentist fills a cavity this deep, the nerve can remain irritated even after the procedure is complete.
In these cases, the tooth may feel fine immediately after and then develop sensitivity or aching as the nerve responds over the following months.
If the nerve eventually becomes inflamed beyond recovery, root canal therapy will be needed. In some cases, the nerve heals on its own as it rebuilds protective secondary dentin — but this needs to be monitored by your dentist.
If bacteria reach the dental pulp through a failed filling, crack, or inadequate seal, an infection can develop inside the tooth. This infection can spread to the surrounding bone and tissue.
Signs of a tooth infection include throbbing pain that does not stop, swelling in the gum or jaw area, a bad taste or smell in the mouth, sensitivity to pressure, and sometimes fever.
A dental abscess is a serious condition. It will not resolve on its own. You need professional treatment — usually a root canal or, in severe cases, tooth extraction — to remove the infection and prevent it from spreading.
Bruxism is the habit of grinding or clenching teeth, often during sleep. Most people who grind are not even aware they do it. If you have a filling and also grind your teeth, the constant pressure and friction can crack or loosen the filling over time.
Bruxism also puts stress on the nerve inside the tooth, contributing to pulp irritation and sensitivity that can worsen over months.
If bruxism is the underlying cause, your dentist may recommend a custom night guard to protect your fillings and prevent further damage.
If you have two adjacent fillings made from different metals — for example, one silver amalgam and one gold — they can create a mild electrical current when they touch. This is called galvanic shock.
The resulting sharp, momentary pain is usually brief but can be unpleasant. This is less common today since tooth-colored composite resin fillings are widely used, but older metal fillings can still be responsible.
Replacing one of the metal fillings with a different material typically resolves the issue.
Though uncommon, some patients have a sensitivity or allergic reaction to the materials used in their filling. Amalgam fillings contain small amounts of mercury, nickel, and other metals that can trigger reactions in sensitive individuals.
Composite resin fillings use chemical bonding agents that may cause irritation in rare cases. Symptoms of a material reaction can include swelling, soreness, a persistent bad taste, or rash-like irritation around the tooth.
If an allergy is suspected, your dentist can switch you to a different material. This often resolves the symptoms entirely.
Not all post-filling pain is the same. Some symptoms are minor and can be monitored. Others are serious warning signs that demand a prompt dental visit.
| Warning Sign | What It May Indicate | Urgency |
|---|---|---|
| Throbbing, constant pain | Tooth infection or abscess | See dentist immediately |
| Pain that wakes you at night | Irreversible pulpitis | See dentist within 24–48 hours |
| Swelling in gum, jaw, or face | Spreading infection or abscess | See dentist immediately |
| Fever with tooth pain | Systemic infection spreading | Emergency dental or urgent care |
| Sharp pain when biting | High filling or cracked tooth | See dentist within a few days |
| Bad taste or smell near tooth | Infection or leaking filling | See dentist this week |
| Pain radiating to jaw or ear | Advanced pulpitis or nerve involvement | See dentist urgently |
| Visible crack or gap in filling | Failed filling, bacteria entry | See dentist soon |
| Gum pimple or bump near tooth | Dental abscess draining | See dentist immediately |
| Sensitivity that keeps worsening | Progressing decay or nerve damage | Do not wait — see dentist |
Do not wait out any of these symptoms. Early treatment is almost always simpler, cheaper, and more effective than waiting until the situation worsens.
Understanding the type of pain you are experiencing gives you and your dentist important diagnostic clues.
Brief, sharp pain triggered by cold or sweet foods — Usually nerve sensitivity. If it fades within seconds, this is often reversible and may resolve over time.
Lingering pain after cold or hot that lasts more than 30 seconds — Points toward irreversible pulpitis. The nerve is not recovering and may need a root canal.
Sharp pain when biting down — Classic sign of a high filling or cracked tooth. Localized and pressure-triggered.
Dull, constant ache or throbbing — May indicate infection or significant nerve involvement. Does not require a trigger — it is just always there.
Pain that radiates — When tooth pain spreads to the jaw, ear, temple, or other teeth, the nerve involvement is advanced. This needs evaluation quickly.
Spontaneous pain with no trigger — The tooth aches on its own without eating or drinking. A strong sign that the pulp is significantly inflamed or infected.
Different filling materials carry different risk profiles for long-term sensitivity and pain.
| Filling Type | Material | Pain Risk | Lifespan | Notes |
|---|---|---|---|---|
| Composite Resin | Tooth-colored plastic/glass | Moderate | 7–10 years | Can shrink slightly; may create micro-gaps |
| Amalgam | Silver/mercury alloy | Low-moderate | 10–15+ years | Expands/contracts with temperature; galvanic risk |
| Gold | Cast gold alloy | Low | 15–30 years | Very durable; rarely causes sensitivity |
| Ceramic/Porcelain | Tooth-matched ceramic | Low | 10–15 years | Biocompatible; minimal sensitivity |
| Glass Ionomer | Glass/acrylic | Moderate | 5–7 years | Releases fluoride; weaker than composite |
Composite resin fillings, the most commonly used today, can shrink slightly during placement. This micro-shrinkage can cause gaps between the filling and tooth wall, increasing the risk of sensitivity and secondary decay over time.
Gold fillings carry the lowest long-term pain risk but are the most expensive and visible option.
The depth of a cavity directly affects how likely you are to experience prolonged sensitivity or pain.
Shallow Enamel Fillings — Only affect the outermost layer of the tooth. Recovery is fast and sensitivity is minimal.
Mid-Depth Dentin Fillings — Reach the dentin layer just below enamel. Sensitivity to temperature is more common and may last a few weeks.
Deep Dentin Near Pulp Fillings — Very close to the nerve. Higher risk of prolonged sensitivity, pulpitis, and eventual need for root canal.
Pulp-Adjacent Fillings — Extremely deep. In some cases, the dentist may place a medicated liner to protect the nerve. Even so, the nerve may become inflamed months later.
The deeper the cavity, the more closely you should monitor the tooth after the filling and report any returning or worsening pain to your dentist promptly.
Ignoring pain from a filled tooth does not make the problem go away. In almost every case, delay makes the situation worse.
Secondary decay left untreated progresses deeper into the tooth, eventually reaching the pulp and requiring root canal treatment — or worse, tooth extraction.
An infection left untreated can spread to the jawbone, neighboring teeth, and in severe cases enter the bloodstream — a potentially life-threatening condition called sepsis.
A cracked filling left in place continues to allow bacteria to enter, accelerating decay and increasing the chance of nerve death.
Irreversible pulpitis left untreated progresses to complete pulp necrosis. The nerve dies, but the infection does not — it spreads to the root tip and surrounding bone.
Acting quickly when filling pain appears or returns after months is always the better choice. Early intervention saves teeth, saves money, and prevents serious health complications.

The right treatment depends entirely on what is causing the pain. Here is a breakdown of the most common solutions.
| Cause of Pain | Treatment | Typical Outcome |
|---|---|---|
| High filling / bite misalignment | Bite adjustment — dentist reshapes the filling | Fast relief, often same visit |
| Cracked or failed filling | Filling replacement or dental crown | Tooth restored, pain resolves |
| Secondary decay around filling | Remove decay, replace filling or crown | Stops progression, relieves pain |
| Reversible pulpitis | Monitor, use desensitizing toothpaste, avoid triggers | Often resolves over weeks |
| Irreversible pulpitis | Root canal therapy | Eliminates nerve pain, saves tooth |
| Tooth infection / abscess | Root canal + antibiotics, or extraction | Clears infection, prevents spread |
| Bruxism damage | Night guard + filling repair or crown | Protects fillings and nerve |
| Galvanic shock | Replace one of the conflicting metal fillings | Immediate resolution |
| Allergic reaction | Replace filling with different material | Symptoms clear with new material |
The earlier you identify the cause, the simpler the treatment tends to be. A bite adjustment takes minutes. A root canal takes an hour but saves the tooth. An extraction is permanent and requires replacement options like implants or bridges.
While you should always see a dentist for persistent filling pain, there are some steps that can provide temporary relief while you wait for your appointment.
Warm salt water rinse — Dissolve half a teaspoon of salt in a glass of warm water and rinse gently for 30 seconds. This helps reduce bacterial load and soothe irritated tissue.
Over-the-counter pain relievers — Ibuprofen (an anti-inflammatory) is generally more effective for dental pain than acetaminophen because it also reduces inflammation. Always follow dosage instructions.
Desensitizing toothpaste — Toothpastes containing potassium nitrate or stannous fluoride can help calm nerve sensitivity over time with regular use.
Avoid triggers temporarily — Skip very hot, cold, sweet, or acidic foods on the affected side until you are evaluated. This limits stimulation of the already-irritated nerve.
Chew on the opposite side — Reducing mechanical pressure on the filled tooth limits additional irritation and discomfort while you wait for treatment.
These measures manage symptoms only. They do not treat the underlying cause. A dental visit remains essential.
Prevention reduces the risk of your filling causing problems months or years down the line.
Maintain excellent oral hygiene — Brush twice daily with fluoride toothpaste and floss daily. This prevents secondary decay from forming at filling margins.
Use a soft-bristled toothbrush — Hard brushing can wear down filling material and irritate the gum tissue around it.
Avoid chewing ice, hard candy, or very hard foods — These can crack composite and amalgam fillings, especially older ones.
Wear a night guard if you grind — Bruxism is a major cause of cracked and damaged fillings. A custom night guard protects them while you sleep.
Attend regular dental checkups — Your dentist can detect early decay at filling margins and check for cracks before they cause significant problems. X-rays every 12–24 months are standard.
Limit sugary and acidic foods — These feed the bacteria that cause decay around filling edges.
Replace old fillings proactively — Fillings do not last forever. Composite fillings typically last 7–10 years, amalgam up to 15 years. Worn or aging fillings are more prone to cracking and leaking.
Root canal treatment becomes necessary when the nerve inside the tooth has been damaged beyond natural recovery. Here are the clearest indicators that a root canal is needed.
Pain that is spontaneous and does not require food, drink, or pressure to trigger it is a strong sign that the nerve is significantly inflamed or infected.
Lingering pain after a hot or cold stimulus — where the aching continues for 30 seconds or longer after the trigger is removed — indicates irreversible pulpitis.
Throbbing pain, especially at night or when lying down, combined with swelling or a bad taste in the mouth, suggests infection and possible abscess formation.
Tooth discoloration, where the tooth becomes darker than its neighbors without injury, can indicate the nerve is dying or has died.
If any of these apply to your filled tooth months after your procedure, contact your dentist or an endodontist — a root canal specialist — promptly.

Patients often ask whether the filling material they received affects their chances of developing pain months later.
Composite resin (tooth-colored) fillings are more aesthetically pleasing and bond directly to the tooth. However, the bonding process can cause micro-gaps if not placed correctly, and composite resin can shrink slightly during curing — creating a tiny space between the filling and tooth wall. This micro-gap allows bacteria in, raising the risk of secondary decay and sensitivity.
Amalgam (silver) fillings are harder and more durable. However, they expand and contract with temperature changes more than the surrounding tooth structure, which can gradually stress the tooth and contribute to micro-cracks over years of use.
Neither material is perfect, but composite resin — the most commonly placed filling today — carries a somewhat higher risk of early sensitivity due to bonding and shrinkage. The dentist’s technique and thoroughness of decay removal matter as much as the material chosen.
Many patients who experience recurring filling pain or cracked fillings have undiagnosed bruxism. They grind their teeth at night, applying tremendous force to the filled teeth without realizing it.
Signs that bruxism may be affecting your fillings include waking with jaw soreness or headaches, a partner reporting that you grind in your sleep, multiple fillings cracking over time, and teeth that appear flattened or worn on the biting surface.
If your dentist identifies bruxism as a factor, treatment includes a custom-fitted night guard to protect all your teeth and fillings from nighttime grinding forces.
Addressing the grinding prevents future filling damage and also protects against jaw joint disorders (TMJ issues) that can compound facial pain.
Delayed filling pain often means the nerve was irritated during the procedure and is now inflamed, the filling has cracked or leaked, or secondary decay has formed around the edges. See your dentist for evaluation.
Mild sensitivity for one to two weeks is normal. Some deep fillings may cause sensitivity up to six weeks. Pain that continues or returns after months is not normal and needs professional attention.
Yes. A loose or partially dislodged filling exposes the inner tooth to bacteria, temperature, and pressure, causing significant pain and increasing the risk of infection.
Not always. The cause could be as simple as a high filling needing a quick adjustment. However, if the nerve is irreversibly inflamed or infected, a root canal becomes necessary to save the tooth.
Infected filling pain typically feels like a constant, throbbing ache that does not stop on its own. It may be accompanied by swelling, a bad taste in the mouth, and sensitivity to pressure or biting.
You can manage symptoms temporarily with warm salt water rinses, ibuprofen, and desensitizing toothpaste. However, home care does not address the underlying cause. A dental visit is essential.
Pain when biting down months after a filling is often caused by a high filling creating uneven bite pressure, a crack in the tooth or filling, or secondary decay progressing beneath the restoration.
Yes. Throbbing tooth pain is a warning sign of significant nerve involvement or infection. It should not be ignored. Contact your dentist promptly for an examination and X-rays.
Yes. Bruxism puts constant pressure and friction on fillings, eventually cracking them or stressing the nerve inside the tooth. A night guard can prevent further damage.
See your dentist if pain persists for more than two weeks, returns after settling, is accompanied by swelling or fever, keeps you awake at night, or is throbbing and constant. Do not delay.
Why does my tooth filling hurt after months? Because a filled tooth is not always a fixed tooth — and pain is your most important signal that something needs attention.
From a simple bite adjustment to treatment for irreversible pulpitis or infection, the causes of delayed filling pain are varied but well understood by dental professionals.
The single most important thing you can do is not ignore the symptoms. A small problem caught early — a cracked filling, a bit of secondary decay, a slightly high bite — is quick and straightforward to fix. Left for months or years, that same problem can escalate into an abscess, nerve death, or tooth loss.
If your filled tooth has been hurting for weeks or months, trust your instincts and schedule a dental evaluation. Modern dentistry can resolve almost every cause of post-filling pain, restore your comfort, and protect your natural tooth for years to come. Your smile and your health are worth it.